Abstracts
The aim of this study was analyze the effects of Square-Stepping Exercise (SSE) on depressive symptoms, balance and functional mobility in older adults. Participants were distributed into two groups: Trained Group (TG), who performed a 16-week intervention with SSE and Control Group (CG), who performed only evaluations. The Berg Balance Scale and Time Up and Go Test (TUG) constituted the evaluation protocol to verify balance and functional mobility. Geriatric Depression Scale-short form (GDS-15) was applied for measure depressive symptoms. Evaluations were realized pre and post 16-week. Significant improvements were observed in the TG with the maintenance of GDS-15 scores and on the time to perform the TUG test which reflects better functional mobility than the CG. This could lead to conclude that the SSE is an important tool for improve balance, prevent falls and decrease depression symptoms.
balance; mobility; depressive symptoms; aging
"Efeitos do Square-Stepping Exercise (SSE) no equilíbrio e sintomas depressivos de idosos." O objetivo desse estudo foi analisar os efeitos do Square-Stepping Exercise (SSE) nos sintomas depressivos, equilíbrio e mobilidade funcional de idosos. Os participantes foram distribuídos em dois grupos: Grupo Treinamento (TG), que realizou 16 semanas de intervenção com o SSE e Grupo Controle (CG), que penas respondeu as avaliações. A Escala de Equilíbrio de Berg e o Time Up and Go Test (TUG) constituíram o protocolo de avaliação, e verificaram o equilíbrio e a mobilidade funcional. A Escala Geriátrica de Depressão curta (GDS-15) foi aplicada para mensurar os sintomas depressivos. Avaliações Foram realizadas pré e após 16 semanas. Resultados significativos foram observados no TG, como a manutenção do escore da GDS-15 e melhora do tempo para realizar o TUG, o que reflete em uma mobilidade funcional melhor que no CG. Podemos concluir que o SSE é uma importante ferramenta para promover equilíbrio, prevenir que das e diminuir os sintomas depressivos.
equilíbrio; mobilidade; sintomas depressivos; envelhecimento
"Efectos del Square-Stepping Exercise (SSE) en equilibrio y síntomas depresivos en adultos mayores." El objetivo de este estudio fue analizar los efectos del SSE (Square-Stepping Exercise) en los síntomas depresivos, equilibrio y movilidad funcional de ancianos. Los participantes fueron divididos en dos grupos: Grupo de Entrenamiento (TG), que celebró 16 semanas de intervención con SSE y Grupo Control (GC), que respondió evaluaciones plumas. El rango de equilibrio de Berg Balance de el Time Up nd Go Test (TUG) constituyeron el protocolo de evaluación, y se encontró el equilibrio y la movilidad funcional. La Escala de Depresión Geriátrica breve (GDS-15) se utilizó para medir los síntomas depresivos. Las evaluaciones se realizaron antes y después de 16 semanas. Los resultados significativos se observaron en TG, como el mantenimiento de la puntuación GDS-15 y la mejora de tiempo para realizar el TUG, que se refleja en una mejor movilidad funcional en CG. Podemos concluir que la ESS es una herramienta importante para promover el equilibrio, la prevención y disminución de los síntomas depresivos.
equilibrio; movilidad; síntomas depresivos; envejecimiento
Introduction
The aging process can cause significant changes that seem to be associated with the reduction of functional capacity components, such as balance, agility, coordination and muscle strength, which could impair mobility (Nyberg, Gustafson, Berggren, Brannstrom, & Bucht, 1996Nyberg, L., Gustafson, Y., Berggren, D., Brannstrom, B., & Bucht, G. (1996). Falls leading to femoral neck fractures in lucid older people. Journal of American Geriatrics Society, 44, 156-160.). Decrease of functional ability is directly linked to increased risk of falls in older individuals (Pavol, Owings, Foley, & Grabiner, 2001Pavol, M.J., Owings, T.M., Foley, K.T., & Grabiner, M.D. (2001). Mechanisms leading to a fall from an induced trip in healthy older adults. Journals of gerontology. Series A, Biological sciences and medical sciences, 56, M428-437.). Physical exercises are an effective strategy used to improve functional fitness indexes with significant reduction of occurrence of falls (El-Khoury, Cassou, Charles, & Dargent-Molina, 2013El-Khoury, F., Cassou, B., Charles, M.A., Dargent-Molina, P. (2013). The effect of fall prevention exercise programmes on fall induced injuries in community dwelling older adults: systematic review and meta-analysis of randomised controlled trials. Britsh Medical Journal. Oct 29;347:f6234.). However, older people remain with lower levels of physical activity because of the perception of many environmental barriers that creates difficulties or impairs the practice of physical exercises (Nascimento, Gobbi, Hirayama, & Brazão, 2008Nascimento, C.M.C., Gobbi, S., Hirayama, M.S. & Brazão, M.C. (2008). Nível de atividade física e as principais barreiras percebidas por idosos de Rio Claro. Revista de Educação Física/UEM, 19, 109-118.; Sebastião et al., 2013Sebastião, E., Chodzko-Zajko, W., Schwingel, A., Gobbi, L.T.B., Papini, C.B., Nakamura,... Gobbi, S. (2013). Perceived barriers to leisure time physical activity: What Brazilians have to say? Open Journal of Preventive Medicine, 3, 491-499.). Additionally, fear of possible accidents resulting in injuries may be a limiting factor for older people to become physically active (Tu, Stump, Damush, & Clark, 2004Tu, W., Stump, T.E., Damush, T.M., & Clark, D.O. (2004). The effects of health and environment on exercise-class participation in older, urban women. Journal of Aging and Physical Activity, 12, 480-496.).
Lack of physical activity can lead to decreased ability to perform daily living activities in a safe way, impairing functional independency. Losses associated with aging are frequently connected to the development of depressive symptoms. Sai, Gallagher, Smith, and Logsdon (2010)Sai, A.J., Gallagher, J.C., Smith, L.M., & Logsdon, S. (2010). Fall predictors in the community dwelling elderly: a cross sectional and prospective cohort study. Journal of musculoskeletal and neuronal interactions, 10, 142-150. found differences in the Geriatric Depression Scale scores for both males and females fallers when they were compared with non-fallers, although positive effects of physical exercises both for mobility and mood depressive states in older adults are already consolidated (Hausdorff, Peng, Goldberger, & Stoll, 2004Hausdorff, J.M., Peng, C., Goldberger, L.A., & Stoll, A.L. (2004). Gait unsteadiness and fall risk in two affective disorders: A preliminary study. BioMed Central Psychiatry, 4, 39).
Considering the implications of physical inactivity for older people and the environmental barriers to exercising, Shigematsu and Okura (2006)Shigematsu, R., & Okura, T. (2006). A novel exercise for improving lower-extremity functional fitness in the elderly. Aging Clinical and Experimental Research, 18, 242-248. developed the Square-Stepping Exercise (SSE). It is a feasible method that can be easily performed indoors. Movements are similar to walking, involving multiple direction movements. This type of exercises is performed on a thin mat partitioned into 40 squares (25 cm each). The SSE seems to be a great method for preventing risk of falls and improving balance as it involves sensorimotor stimulation (Shigematsu et al., 2008Shigematsu, R., Okura, T., Nakagaichi, M., Tanaka, K., Sakai, T., Kitazumi, S., & Rantanen, T. (2008). Square-stepping exercise and fall risk factors in older adults: a single-blind, randomized controlled trial. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 63, 76-82.; Shigematsu, Okura, Sakai, & Rantanen, 2008Shigematsu, R., Okura, T., Sakai, T., & Rantanen, T. (2008). Square-stepping exercise versus strength and balance training for fall risk factors. Aging Clinical and Experimental Research, 20, 19-24.). SSE tasks require the integration of cognitive and motor information during the performance of dual-task. The long-term practice of these exercises may promote improvements on motor and cortical centers, which affect vestibular ratio and directional control, helping balance and mobility, especially in elderly (Tsang & Hi-Chan, 2004Tsang, W.W., & Hui-Chan, C.W. (2004). Effect of 4-and 8-wk intensive Tai Chi training on balance control in the elderly. Medicine and science in sports and exercise, 36, 648-657.). A Brazilian study found that SSE is a physical activity that contributes positively to improve multiple cognitive domains (Teixeira et al.,2013Teixeira, C.V.L., Gobbi, S., Pereira, J.R., Ueno, D.T., Shigematsu, R., Gobbi, L.T.B. (2013). Effect of square-stepping exercise and basic exercises on functional fitness of older adults. Geriatrics and Gerontology International, 13, 842-8). However, to the best of our knowledge, there are no papers reporting the influence of SSE exercise on symptoms of depression in healthy older people. A research about the benefits of physical interventions has found that long-term physical exercises reduce depressive symptoms (Blankevoort et al., 2010Blake, H., Mo, P., Malik, S., & Thomas, S. (2009). How effective are physical activity interventions for alleviating depressive symptoms in older people? A systematic review. Society for Research in Rehabilitation, 23, 873-887.) and improve functionality with significant positive effects on quality of life (Scott, Votova, Scanlan, & Close, 2007Scott, V., Votova, K., Scanlan, A., & Close, J. (2007). Multifactorial and functional mobility assessment tools for fall risk among older adults in community, home-support, long-term and acute care settings. Age and Ageing, 36, 130-139.). Regular physical exercises seem to have a positive impact on older adults' psychological wellbeing. Seniors who exercise regularly are more self-motivated, present better perception of self-efficacy and wellness (Lee, Lee, Brar, Rush, & Jolley, 2014Lee, H., Lee, J.A., Brar, J.S., Rush E.B., & Jolley C.J. (2014). Physical activity and depressive symptoms in older adults. Geriatric Nursing, 35, 37-41.). These gains may be related to the practice in group of people and in the establishment of new social networks. In addition to that, physical activity and social interactions counteract the effects of social retirement on functional decline, expanding activities of daily-living and well-being (Unger, Johnson, & Marks, 1997Unger, J.B., Johnson, C.A., & Marks, G. (1997). Functional decline in the elderly: evidence for direct and stress-buffering protective effects of social interactions and physical activity. Annals of Behavioral Medicine, 19, 152-160.).
The aim of this study was to analyze the effects of a 16-week intervention of a protocol of SSE on balance, functional mobility and symptoms of depression in older adults.
Method
Ethical aspects
The study was carried out in the Laboratory of Aging and Physical Activity, Department of Physical Education, Biosciences Institute, São Paulo State University at Rio Claro, Brazil. This study follows the guidelines of the Declaration of Helsinki and it was approved by the Local Ethics Committee (Protocol #2850). All participants were informed about the procedures, benefits and risks before giving and signing the written informed consent.
Participants
The participants were recruited through a cohort of older adults who took part of a geriatric day-care assistance mode. All participants who met the inclusion criteria and accepted to participate on the 16-week SSE program were included in the study.
The sample was composed of 32 older adults who were living in the city of Rio Claro, SP, Brazil. The inclusion criteria were: (a) not having any kind of cognitive impairment that would characterize a mild cognitive impairment or dementia; (b) to be classified as an older adult according the standard of Brazil, i.e., 60 years of age or older; (c) not having signs of dementia based on results in the Mini-Mental State Examination-MMSE (Folstein, Folstein, & McHugh, 1975Folstein, M.F., Folstein, S.E., & McHugh, P.R. (1975). "Mini-mental state." A practical method for grading the cognitive state of patients for the clinician. Journal of psychiatric research, 12, 189-198.) adjusted according to the patient's level of education, which was validated for Brazilian population (Brucki, Nitrini, Caramelli, Bertolucci, & Okamoto, 2003Brucki, S.M., Nitrini, R., Caramelli, P., Bertolucci, P.H., & Okamoto, I.H. (2003). [Suggestions for utilization of the mini-mental state examination in Brazil]. Arquivos de Neuropsiquiatria, 61, 777-781.); (d) not been on any physical exercise program for at least six months before starting this intervention program; (e) to have minimum of 75% attendance in the intervention sessions.
The participants were distributed into two groups: Trained Group (TG) (n=15) and Control Group (CG) (n=17). The TG attended the 16-week of training on SSE. The CG kept to their same daily routine and did not participate in any regular or structured exercise program. This was monitored by a Level of Physical Activity Questionnaire (Voorrips, Ravelli, Dongelmans, Deurenberg, & Van Staveren, 1991Voorrips, L.E., Ravelli, A.C., Dongelmans, P.C., Deurenberg, P., & Van Staveren, W.A. (1991). A physical activity questionnaire for the elderly. Medicine and Science in Sports and Exercise, 23, 974-979.) applied before the intervention period. All evaluations were conducted on the same period by the same single-blinded trained examiner.
Evaluation protocol
All participants were assessed at the baseline and after 16 weeks at the end of the SSE training. Outcome measures were evaluated, under the same conditions, at two moments by the same trained examiner, at the same time, at the same place. In order to characterize the sample, data of age, schooling and level of physical activity (evaluated by Baecke Questionnaire Modified for Elderly; QBMI) were collected.
The characterization of global status of cognitive functions, the Mini-Mental State Examination (MMSE) (Folstein et al., 1975Folstein, M.F., Folstein, S.E., & McHugh, P.R. (1975). "Mini-mental state." A practical method for grading the cognitive state of patients for the clinician. Journal of psychiatric research, 12, 189-198.) was employed. This instrument includes questions distributed into seven categories that represent specific cognitive functions: executive functions, memory, language, attention, immediate and delayed recall, and visuoconstruction praxis. Scores range from 0 to 30 points, and lower values could indicate some impairment on cognitive functions. Cut-off points were based on scores proposed by Brucki et al. (2003)Brucki, S.M., Nitrini, R., Caramelli, P., Bertolucci, P.H., & Okamoto, I.H. (2003). [Suggestions for utilization of the mini-mental state examination in Brazil]. Arquivos de Neuropsiquiatria, 61, 777-781. for Brazilian population according to their educational level. Using this adjustment, our sample was not detected to have cognitive impairment (Table 1).
The Geriatric Depression Scale short form (GDS-15) is one of the most used instruments for screening depression in later life. This instrument has been widely used in both clinical and research settings (Montorio & Izal, 1996Montorio, I., & Izal, M. (1996). The Geriatric Depression Scale: a review of its development and utility. International Psychogeriatrics, 8, 103-112.) and it is a short, 15-item instrument specifically designed to assess depression in geriatric populations. The items require a yes/no response. Almeida and Almeida (1999aAlmeida, O.P., & Almeida, S.A. (1999a). [Reliability of the Brazilian version of the ++abbreviated form of Geriatric Depression Scale (GDS) short form]. Arquivos de Neuropsiquiatria, 57, 421-426., 1999bAlmeida, O.P., & Almeida, S.A. (1999b). Short versions of the geriatric depression scale: a study of their validity for the diagnosis of a major depressive episode according to ICD-10 and DSM-IV. International Journal of Geriatric Psychiatry, 14, 858-865.) found good values for specificity and sensibility (90.9 and 64.5, respectively) for clinical diagnosis according to DSM-IV with cut-off point 5/6 for Brazilian patients. On GDS, a higher score represents greater presence of depressive symptoms.
The 14-item Berg Balance Scale evaluates balance impairment in older adults (Podsiadlo & Richardson, 1991Podsiadlo, D., & Richardson, S. (1991). The timed "Up & Go:" A test of basic functional mobility for frail elderly persons. Journal of American Geriatrics Society, 39, 142-148.). It assesses the individual's ability to maintain balance during the performance of 14 common tasks in daily life, such as sitting down and standing up from a chair, and standing on one leg. The performance of each task was evaluated on a 5-point ordinal scale, ranging from zero to four, according to either quality of movement or time spent to accomplish the task. The zero point represents the necessity of maximum assistance, and four points indicate that the individual is functionally independent to perform the task. A total score (maximum of 56 points) was calculated by the sum of each item. Higher scores reveal better ability to maintain good balance.
The Timed-Up-and-Go test (Podsiadlo & Richardson, 1991Podsiadlo, D., & Richardson, S. (1991). The timed "Up & Go:" A test of basic functional mobility for frail elderly persons. Journal of American Geriatrics Society, 39, 142-148.) consisted of a participant to stand up from a sitting position in an armless chair of seat height of 46.5 cm, walking a distance of 3 m then, going around a cone, returning, and sitting back in the chair. Each participant was instructed to perform the task as quickly as possible, without running. At least one practice trial was offered to the participants at the beginning of the procedure so that they could become familiar with the task. Three trials were performed for testing purposes, and the time to perform the task was measured in seconds. Time was recorded from the instant the person's buttocks left the chair until the next contact with the chair. The mean value of the three trials was considered for statistical analysis.
Exercise protocol
The TG group participated of a supervised training program twice-a-week for 16 weeks. The duration for intervention was defined as 16 weeks because previous investigations concluded that this period of SSE practice is enough to promote significant benefits for older people (Teixeira et al., 2013Teixeira, C.V.L., Gobbi, S., Pereira, J.R., Ueno, D.T., Shigematsu, R., Gobbi, L.T.B. (2013). Effect of square-stepping exercise and basic exercises on functional fitness of older adults. Geriatrics and Gerontology International, 13, 842-8). Moreover, shorter-term interventions may increase the chance of older people to become more physically active and decrease the chances of drop-out on prospective interventional research.
Each session consisted of 60 minutes of SSE. The detailed description of SSE protocol is provided by Shigematsu and Okura (2006)Shigematsu, R., & Okura, T. (2006). A novel exercise for improving lower-extremity functional fitness in the elderly. Aging Clinical and Experimental Research, 18, 242-248.. Briefly, the SSE is a sequence of different steps on a thin felt mat (100 X 250 cm) divided into 40 squares. The exercise session consists in walking from one side of the mat to the other according to a pattern of the protocol. The participant can only see the sequence made by the professional supervisor and, then, they must reproduce it. Many sequences are possible and the level of difficulty is higher after each accomplished sequence.
Statistical analysis
The distributions of all variables were tested for normality using the Shapiro-Wilk test. Descriptive statistics were calculated to demonstrate the groups' baseline sociodemographic characteristics, and the differences between groups were tested using one-way ANOVA. For multiple factors analyses (moment vs. groups), a general linear model for repeated-measures analysis of variance (two-way ANOVA) was used to determine group differences for balance and depressive symptoms. The effect over time (pre- and post-test intervention with SSE program) was treated as the within-subjects factor, and the differences between the TG and CG were treated as the between-subjects factor.
For statistical analyses, a significance level of 5% was defined and it was applied the SPSS 10.0 (SPSS, Inc.) software.
Results
The sample of 32 elderly people was distributed into two groups. Table 1 shows the sociodemographic and clinical characteristics of the participants. There were no differences between the groups regarding these variables (Table 1).
No significant reduction on depressive symptons was observed after the 16-week period of exercise for the TG. On the other hand, significant increase on this variable was observed for the CG. The between-subject factors for two-way ANOVA showed these significant changes (F 1,30=5.7; p= .03). Figure 1 displays scores for the symptoms of depression pre- and post-test intervention with the SSE program for both evaluated groups.
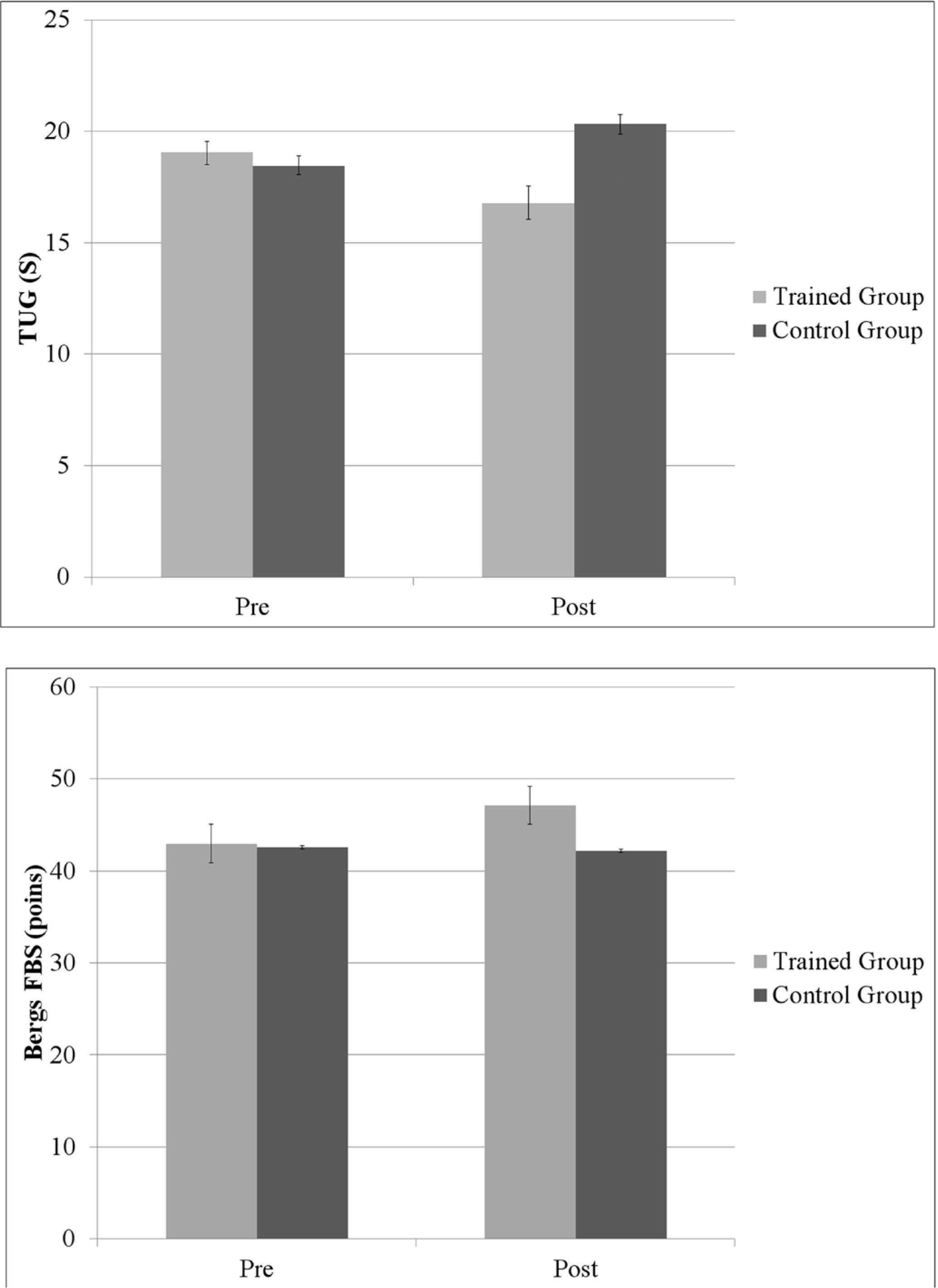
Mean and standard deviation of the scores on GDS-15 by the control and trained groups; *Between-subject effect F1,30= 5.7; p = .03 Figure 2. Mean and standard deviation of (A) time taken to complete the TUG and; (B) the score on Berg's FBS by both groups (control and trained groups); *p= .05
Regarding functional mobility using the TUG (time) test, the TG exhibited significant changes (F 1,30=3.8, p= .04), indicating that these participants reduced the time to complete the TUG task. Participants in the CG did show no significant change in this variable. However, our program did not demonstrate effectiveness and feasibility for improving balance, which was indicated by the lack of significant changes on TUG scores after a 16-week SSE practice (F 1,30=2.54; p= .13). Table 2 shows the descriptive results from both moments and groups evaluated. Figure 2 presents the results for functional mobility (TUG) and balance (Berg's FBS) pre- and post-test intervention in the SSE program for both groups.
Mean and standard deviation of (A) time taken to complete the TUG and; (B) the score on Berg's FBS by both groups (control and trained groups); *p= .05.
Discussion
The purpose of this study was to investigate the effects after practice in a SSE intervention program on depressive symptoms, mobility and functional balance in older people. The results showed positive effects of the SSE intervention program especially when taking into account that the CG who was not exposed to any exercise program presented worse results. Additionally, participants who were engaged in the 16-week SSE practice did not show a depressive mood state, whereas the control group showed improvement on these symptoms after the period of the research (Shumway-Cook, Baldwin, Polissar, & Gruber, 1997Shumway-Cook, A., Baldwin, M., Polissar, N.L., & Gruber, W. (1997). Predicting the probability for falls in community-dwelling older adults. Physiotherapy, 77, 812-819.). Values of the time spent to perform the TUG task by our sample were in both assessment moments below 20 s, and this could indicate that the participants were totally independent in tasks that involve functional mobility (Shumway-Cook, Brauer, & Woollacott, 2000Shumway-Cook, A., Brauer, S., & Woollacott, M. (2000). Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Physiotherapy, 80, 896-903.). This also can indicate that all participants included in our TG sample were able to safely perform their daily living activities. Shumway-Cook et al. (1997)Shumway-Cook, A., Baldwin, M., Polissar, N.L., & Gruber, W. (1997). Predicting the probability for falls in community-dwelling older adults. Physiotherapy, 77, 812-819.indicated that the attribution of poor balance accounts for 10-25% on the incidence of falls in older people. Lower values of walking speed are frequently associated with increases risk of falls. Recently, Kwan, Lin, Chen, Close, and Lord (2011)Kwan, M.M., Lin, S.I., Chen, C.H., Close, J.C., & Lord, S.R. (2011). Sensorimotor function, balance abilities and pain influence Timed Up and Go performance in older community-living people. Aging Clinical and Experimental Research, 23, 196-201. found that TUG test performance can be influenced by lower limb strength, poor balance, increased reaction time, low vision and pain. Also, the TUG test performance and speed of walking are variables associated with limitations on functional daily living activities and fear of falling (Kwan et al., 2011Kwan, M.M., Lin, S.I., Chen, C.H., Close, J.C., & Lord, S.R. (2011). Sensorimotor function, balance abilities and pain influence Timed Up and Go performance in older community-living people. Aging Clinical and Experimental Research, 23, 196-201.; Viccaro, Perera, & Studenski, 2011Viccaro, L.J., Perera, S., & Studenski, S.A. (2011). Is timed up and go better than gait speed in predicting health, function, and falls in older adults? Journal of American Geriatric Society, 59, 887-892.).
Shigematsu and Okura (2006)Shigematsu, R., & Okura, T. (2006). A novel exercise for improving lower-extremity functional fitness in the elderly. Aging Clinical and Experimental Research, 18, 242-248. found improved locomotion speed (walking around 2 cones) using the same SSE program of intervention, better neuromuscular function and coordination as a protective response to falls. Another research in this field indicated that SSE was as effective as a specific training to strength and balance to prevent falls in older people (Shigematsu et al., 2008Shigematsu, R., Okura, T., Nakagaichi, M., Tanaka, K., Sakai, T., Kitazumi, S., & Rantanen, T. (2008). Square-stepping exercise and fall risk factors in older adults: a single-blind, randomized controlled trial. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 63, 76-82.). The main difference of our study compared to others using the same protocol is that in our research SSE was not associated with any other exercise (even the warm-up, muscular resistance training, stretching or relaxing), showing the effects of SSE intervention individually. These effects were emphasized for functional mobility likely due to the specificity of the training session, which involves movements with steps in multiple directions, integration of cognitive and motor task to perform the correct sequence and some level of proprioceptive development. Thus, the present study demonstrated that SSE protocol alone can be effective on balance. It is possible to use this protocol with a fragile population, for example, an older one.
When a randomized clinical trial compared the SSE program with regular walking exercises (Shigematsu et al., 2008Shigematsu, R., Okura, T., Nakagaichi, M., Tanaka, K., Sakai, T., Kitazumi, S., & Rantanen, T. (2008). Square-stepping exercise and fall risk factors in older adults: a single-blind, randomized controlled trial. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 63, 76-82.), SSE showed better responses of a program of exercises designed for fall prevention than regular walking for older adults. Also, comparing SSE with a balance and strength training (Shigematsu et al., 2008Shigematsu, R., Okura, T., Nakagaichi, M., Tanaka, K., Sakai, T., Kitazumi, S., & Rantanen, T. (2008). Square-stepping exercise and fall risk factors in older adults: a single-blind, randomized controlled trial. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 63, 76-82.), researchers found significant decrease on risk of fall in both modalities of training. Putting them together, these results may indicate that specific components of functional capacity are needed to prevent falls. Specific trainings (i.e., balance and strength training) seem to improve mobility and, in this perspective, SSE may be a feasible and a simple tool to be employed as a specific training to mobility, with positive effects on fall prevention. Probably, this program could be efficient for mobility because it uses multidirectional steps (forward, backward, lateral and oblique directions) during one session. During the 16-week intervention, higher activation of the synergist and agonist muscles responsible to the locomotion (mainly legs) may have occurred to complete the sequences proposed by the SSE. Moreover, this seems to reflect on the improvement of specific components of functional mobility which, in turn may reflect on mobility improvement.
As for depressive symptons, the participants who remained physically inactive showed worse symptoms in the post-test. Our study did not investigate major depression symptoms qualified as a psychiatric condition. However, we did detect changes in mood states that may potentially predispose these participants to a mood disorder. Within physiological aging, there is social aging. Thus, older individuals show less social interaction than younger people and, although sometimes family relationships are narrowed, peripheral relationships reduced greatly, making the older individuals feel more depressed, which increases GDS scores (Cesari et al., 2002Cesari, M., Landi, F., Torre, S., Onder, G., Lattanzio, F., & Bernabei, R. (2002). Prevalence and risk factors for falls in an older community-dwelling population. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 57, M722-726.; Chu, Chi, & Chiu, 2005Chu, L.W., Chi, I., & Chiu, A.Y. (2005). Incidence and predictors of falls in the chinese elderly. Annals of the Academy of Medicine, Singapore, 34, 60-72.; Ilkivi, 2005Ilkiv, T.F. (2005). Avaliação da aptidão física de idosos do Centro de Convivência da Melhor Idade do município de Monte Alto. Dissertação (Mestrado em Promoção de Saúde). Universidade de Franca. Franca.; Mann et al., 2005Mann, W.C., Kimble, C., Justiss, M.D., Casson, E., Tomita, M., & Wu, S.S. (2005). Problems with dressing in the frail elderly. The American journal of occupational therapy, 59, 398-408.).
The role of physical activity on mood disorders is consolidated in the literature. The more physically active individuals are less symptoms of depression. The SSE intervention seems to be an outcome clinically relevant for older people (Blake, Mo, Malik, & Thomas, 2009Blake, H., Mo, P., Malik, S., & Thomas, S. (2009). How effective are physical activity interventions for alleviating depressive symptoms in older people? A systematic review. Society for Research in Rehabilitation, 23, 873-887.). In our study, the need to overcome challenges during sessions of SSE and the social network established during the 16-week intervention could likely be responsible for the changes observed and prevent the development of symptoms of depression- maintenance of GDS scores for the TG and increase of scores for the CG. The social contact during the practice can help to reduce stress, negative feelings, and isolation, promoting interaction and connection all participants (Goodwin, 2003Goodwin, R.D. (2003). Association between physical activity and mental disorders among adults in the United States. Preventive Medicine, 36, 698-703.; Heath & Stuart, 2002Heath, J.M., & Stuart, M.R. (2002). Prescribing exercise for frail elders. The Journal of the American Board of Family Practice, 15, 218-228.; Ku, McKenna, & Fox, 2007Ku, P.W., McKenna, J., & Fox, K.R. (2007). Dimensions of subjective well-being and effects of physical activity in Chinese older adults. Journal of aging and physical activity, 15, 382-397.). In our study, there was a concern with additionally stimulating the mental and social dimensions since physical interventions with moderate intensities have already presented positive results (Colcombe & Kramer, 2003Colcombe, S., & Kramer, A.F. (2003). Fitness effects on the cognitive function of older adults: a meta-analytic study. American Psychological Society, 14, 125-130.; Kramer, Erickson, & Colcombe, 2006Kramer, A.F., Erickson, K.I., & Colcombe, S.J. (2006). Exercise, cognition, and the aging brain. Journal of Applied Physiology, 101, 1237-1242.; Teri et al., 2003Teri, L., Gibbons, L.E., McCurry, S.M., Logsdon, R.G., Buchner, D.M., Barlow, W.E., ... Larson, E.B. (2003). Exercise plus behavioral management in patients with Alzheimer disease: a randomized controlled trial. Journal of the American Medical Association, 290, 2015-2022.), although alternatives depend on the degree of impairment due to aging.
Even patients with some pathological condition seem to be benefited by systematic physical exercises as shown by Arredondo et al. (2011)Arredondo, E.M., Mendelson, T., Elder, J.P., Marshall, S., La Flair, L., & Ayala, G.X. (2011). The Relation of Medical Conditions to Depressive Symptoms Among Latinos: Leisure Time Physical Activity as a Mediator. Journal of Health Psychology, 17, 742-52.. Their trial showed significant relationship between lower symptoms of depression and higher levels of physical activity in older hypertensive adults. Lucas et al. (2011Lucas, M., Mekary, R., Pan, A., Mirzaei, F., O'Reilly, E.J., Willett. W.C.,... Ascherio A. (2011). Relation Between Clinical Depression Risk and Physical Activity and Time Spent Watching Television in Older Women: A 10-Year Prospective Follow-up Study. American journal of epidemiology, 174, 1017-1027.) noticed a higher relative risk of depressive symptoms in people with lower levels of physical activity compared to those higher levels ones. Additionally, they showed a significant relationship between increased incidence of depression on a 10-year follow-up and higher television watching-time, indicating the importance of the social network in the mood dimension. In order to confirm the significance of social networks on functional status and mobility maintenance, other researches (Mendes de Leon et al., 1999Mendes de Leon, C.F., Glass, T.A., Beckett, L.A., Seeman, T.E., Evans, D. A., & Berkman, L.F. (1999). Social networks and disability transitions across eight intervals of yearly data in the New Haven EPESE. Journals of gerontology. Series B, Psychological sciences and social sciences, 54, S162-172.; Mendes de Leon, Gold, Glass, Kaplan, & George, 2001Mendes de Leon, C.F., Gold, D.T., Glass, T.A., Kaplan, L., & George, L.K. (2001). Disability as a function of social networks and support in elderly African Americans and Whites: the Duke EPESE 1986--1992. Journals of gerontology. Series B, Psychological sciences and social sciences, 56, S179-190.) confirmed that social activity especially during physical activity (Glass, de Leon, Marottoli, & Berkman, 1999Glass, T.A., de Leon, C.M., Marottoli, R.A., & Berkman, L.F. (1999). Population based study of social and productive activities as predictors of survival among elderly Americans. Britsh Medical Journal, 319, 478-483.) is related to less disabilities and better perception of quality of life, with impact on mood.
SSE is a low cost type of physical exercise method that does not require higher overload in patients and can promote great results on functional mobility with potential reduction of risk for falls. This could indicate that this method is a feasible alternative for older people, mainly for those who have a fragile health or those with some frail condition which might impair the practice of more intense exercise.
There are several limitations that may have affected the results of our study. First, we used a non-randomized sample, which can narrow generalizations. On the other hand, the longitudinal design allowed us to establish causality between the analyzed variables. Other follow-up study is suggested to control the maintenance of the gains after participation in a SSE program. Regarding these limitations, as participants were outpatients in a day-care center, our findings justify the importance of low intensity, low cost and low tech exercise as an alternative with positive gains for older individuals. These results may help healthcare professionals to recognize alternative options for preventing risk of falls and for improving mobility despite the low level of physical activity of the group of patients.
In conclusion, our findings suggest that a 16-week program of physical exercises based only on the SSE method could be a safety, low-cost and feasible alternative to practice physical activity with good impact on improvement of functional mobility and maintenance of mood states, preventing depressive symptons in older people.
References
- Almeida, O.P., & Almeida, S.A. (1999a). [Reliability of the Brazilian version of the ++abbreviated form of Geriatric Depression Scale (GDS) short form]. Arquivos de Neuropsiquiatria, 57, 421-426.
- Almeida, O.P., & Almeida, S.A. (1999b). Short versions of the geriatric depression scale: a study of their validity for the diagnosis of a major depressive episode according to ICD-10 and DSM-IV. International Journal of Geriatric Psychiatry, 14, 858-865.
- Arfken, C.L., Lach, H.W., Birge, S.J., & Miller, J.P. (1994). The prevalence and correlates of fear of falling in elderly persons living in the community. American Journal of Public Health, 84, 565-570.
- Arredondo, E.M., Mendelson, T., Elder, J.P., Marshall, S., La Flair, L., & Ayala, G.X. (2011). The Relation of Medical Conditions to Depressive Symptoms Among Latinos: Leisure Time Physical Activity as a Mediator. Journal of Health Psychology, 17, 742-52.
- Blake, H., Mo, P., Malik, S., & Thomas, S. (2009). How effective are physical activity interventions for alleviating depressive symptoms in older people? A systematic review. Society for Research in Rehabilitation, 23, 873-887.
- Blankevoort, C.G., van Heuvelen, M.J., Boersma, F., Luning, H., de Jong, J., & Scherder, E.J. (2010). Review of effects of physical activity on strength, balance, mobility and ADL performance in elderly subjects with dementia. Dementia Geriatric and Cognitive Disorders, 30, 392-402.
- Brucki, S.M., Nitrini, R., Caramelli, P., Bertolucci, P.H., & Okamoto, I.H. (2003). [Suggestions for utilization of the mini-mental state examination in Brazil]. Arquivos de Neuropsiquiatria, 61, 777-781.
- Cesari, M., Landi, F., Torre, S., Onder, G., Lattanzio, F., & Bernabei, R. (2002). Prevalence and risk factors for falls in an older community-dwelling population. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 57, M722-726.
- Colcombe, S., & Kramer, A.F. (2003). Fitness effects on the cognitive function of older adults: a meta-analytic study. American Psychological Society, 14, 125-130.
- Chu, L.W., Chi, I., & Chiu, A.Y. (2005). Incidence and predictors of falls in the chinese elderly. Annals of the Academy of Medicine, Singapore, 34, 60-72.
- El-Khoury, F., Cassou, B., Charles, M.A., Dargent-Molina, P. (2013). The effect of fall prevention exercise programmes on fall induced injuries in community dwelling older adults: systematic review and meta-analysis of randomised controlled trials. Britsh Medical Journal. Oct 29;347:f6234.
- Ferrucci, L., Guralnik, J.M., Studenski, S., Fried, L.P., Cutler, G.B., Jr., & Walston, J.D. (2004). Designing randomized, controlled trials aimed at preventing or delaying functional decline and disability in frail, older persons: a consensus report. Journal of American Geriatrics Soceity, 52, 625-634.
- Folstein, M.F., Folstein, S.E., & McHugh, P.R. (1975). "Mini-mental state." A practical method for grading the cognitive state of patients for the clinician. Journal of psychiatric research, 12, 189-198.
- Glass, T.A., de Leon, C.M., Marottoli, R.A., & Berkman, L.F. (1999). Population based study of social and productive activities as predictors of survival among elderly Americans. Britsh Medical Journal, 319, 478-483.
- Goodwin, R.D. (2003). Association between physical activity and mental disorders among adults in the United States. Preventive Medicine, 36, 698-703.
- Granacher, U., Muehlbauer, T., Zahner, L., Gollhofer, A., & Kressig, R.W. (2011). Comparison of traditional and recent approaches in the promotion of balance and strength in older adults. Sports Medicine, 41, 377-400.
- Hausdorff, J.M., Peng, C., Goldberger, L.A., & Stoll, A.L. (2004). Gait unsteadiness and fall risk in two affective disorders: A preliminary study. BioMed Central Psychiatry, 4, 39
- Heath, J.M., & Stuart, M.R. (2002). Prescribing exercise for frail elders. The Journal of the American Board of Family Practice, 15, 218-228.
- Iavarone, A., Milan, G., Vargas, G., Lamenza, F., De Falco, C., Gallotta, G., & Postiglione, A. (2007). Role of functional performance in diagnosis of dementia in elderly people with low educational level living in Southern Italy. Aging Clinical and Experimental Research, 19, 104-109.
- Iecovich, E., Jacobs, J.M., & Stessman, J. (2011). Loneliness, social networks, and mortality: 18 years of follow-up. International journal of aging & human development, 72, 243-263.
- Ilkiv, T.F. (2005). Avaliação da aptidão física de idosos do Centro de Convivência da Melhor Idade do município de Monte Alto. Dissertação (Mestrado em Promoção de Saúde). Universidade de Franca. Franca.
- James, B.D., Boyle, P.A., Buchman, A.S., & Bennett, D.A. (2011). Relation of late-life social activity with incident disability among community-dwelling older adults. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 66, 467-473.
- Judge, J.O., Schechtman, K., & Cress, E. (1996). The relationship between physical performance measures and independence in instrumental activities of daily living. The FICSIT Group. Frailty and Injury: Cooperative Studies of Intervention Trials. Journal of American Geriatrics Society, 44, 1332-1341.
- Karp, A., Paillard-Borg, S., Wang, H.X., Silverstein, M., Winblad, B., & Fratiglioni, L. (2006). Mental, physical and social components in leisure activities equally contribute to decrease dementia risk. Dementia Geriatric and Cognitive Disorders, 21, 65-73.
- Kivela, S.L., & Pahkala, K. (2001). Depressive disorder as a predictor of physical disability in old age. Journal of American Geriatrics Society, 49, 290-296.
- Kramer, A.F., Erickson, K.I., & Colcombe, S.J. (2006). Exercise, cognition, and the aging brain. Journal of Applied Physiology, 101, 1237-1242.
- Kressig, R.W., Wolf, S.L., Sattin, R.W., O'Grady, M., Greenspan, A., Curns, A., & Kutner, M. (2001). Associations of demographic, functional, and behavioral characteristics with activity-related fear of falling among older adults transitioning to frailty. Journal of American Geriatrics Society, 49, 1456-1462.
- Ku, P.W., McKenna, J., & Fox, K.R. (2007). Dimensions of subjective well-being and effects of physical activity in Chinese older adults. Journal of aging and physical activity, 15, 382-397.
- Kwan, M.M., Lin, S.I., Chen, C.H., Close, J.C., & Lord, S.R. (2011). Sensorimotor function, balance abilities and pain influence Timed Up and Go performance in older community-living people. Aging Clinical and Experimental Research, 23, 196-201.
- Lee, H., Lee, J.A., Brar, J.S., Rush E.B., & Jolley C.J. (2014). Physical activity and depressive symptoms in older adults. Geriatric Nursing, 35, 37-41.
- Lucas, M., Mekary, R., Pan, A., Mirzaei, F., O'Reilly, E.J., Willett. W.C.,... Ascherio A. (2011). Relation Between Clinical Depression Risk and Physical Activity and Time Spent Watching Television in Older Women: A 10-Year Prospective Follow-up Study. American journal of epidemiology, 174, 1017-1027.
- Maki, Y., Ura, C., Yamaguchi, T., Murai, T., Isahai, M., Kaiho, A., ... Yamaguchi, H. (2012). Effects of Intervention Using a Community-Based Walking Program for Prevention of Mental Decline: A Randomized Controlled Trial. Journal of American Geriatrics Society, 60, 505-10.
- Mann, W.C., Kimble, C., Justiss, M.D., Casson, E., Tomita, M., & Wu, S.S. (2005). Problems with dressing in the frail elderly. The American journal of occupational therapy, 59, 398-408.
- Martins, R., Coelho, E.S.M., Pindus, D., Cumming, S., Teixeira, A., & Verissimo, M. (2011). Effects of strength and aerobic-based training on functional fitness, mood and the relationship between fatness and mood in older adults. The Journal of sports medicine and physical fitness, 51, 489-496.
- Mendes de Leon, C.F., Glass, T.A., Beckett, L.A., Seeman, T.E., Evans, D. A., & Berkman, L.F. (1999). Social networks and disability transitions across eight intervals of yearly data in the New Haven EPESE. Journals of gerontology. Series B, Psychological sciences and social sciences, 54, S162-172.
- Mendes de Leon, C.F., Gold, D.T., Glass, T.A., Kaplan, L., & George, L.K. (2001). Disability as a function of social networks and support in elderly African Americans and Whites: the Duke EPESE 1986--1992. Journals of gerontology. Series B, Psychological sciences and social sciences, 56, S179-190.
- Montorio, I., & Izal, M. (1996). The Geriatric Depression Scale: a review of its development and utility. International Psychogeriatrics, 8, 103-112.
- Murphy, S.L., Williams, C.S., & Gill, T.M. (2002). Characteristics associated with fear of falling and activity restriction in community-living older persons. Journal of American Geriatrics Society, 50, 516-520.
- Nascimento, C.M.C., Gobbi, S., Hirayama, M.S. & Brazão, M.C. (2008). Nível de atividade física e as principais barreiras percebidas por idosos de Rio Claro. Revista de Educação Física/UEM, 19, 109-118.
- National Center for Health Statistics (2004). Health, United States, 2004, with Cartbook on Trends in the Health of Americans. Hyattville, MD: U.S. Department of Health and Human Services, Center for Disease Control and Prevention.
- Nyberg, L., Gustafson, Y., Berggren, D., Brannstrom, B., & Bucht, G. (1996). Falls leading to femoral neck fractures in lucid older people. Journal of American Geriatrics Society, 44, 156-160.
- Pavol, M.J., Owings, T.M., Foley, K.T., & Grabiner, M.D. (2001). Mechanisms leading to a fall from an induced trip in healthy older adults. Journals of gerontology. Series A, Biological sciences and medical sciences, 56, M428-437.
- Podsiadlo, D., & Richardson, S. (1991). The timed "Up & Go:" A test of basic functional mobility for frail elderly persons. Journal of American Geriatrics Society, 39, 142-148.
- Rowe, J.W., & Kahn, R.L. (1997). Successful aging. The Gerontologist, 37, 433-440.
- Saczynski, J.S., Pfeifer, L.A., Masaki, K., Korf, E.S., Laurin, D., White, L., & Launer, L.J. (2006). The effect of social engagement on incident dementia: the Honolulu-Asia Aging Study. American Journal of Epidemiology, 163, 433-440.
- Sai, A.J., Gallagher, J.C., Smith, L.M., & Logsdon, S. (2010). Fall predictors in the community dwelling elderly: a cross sectional and prospective cohort study. Journal of musculoskeletal and neuronal interactions, 10, 142-150.
- Scott, V., Votova, K., Scanlan, A., & Close, J. (2007). Multifactorial and functional mobility assessment tools for fall risk among older adults in community, home-support, long-term and acute care settings. Age and Ageing, 36, 130-139.
- Sebastião, E., Chodzko-Zajko, W., Schwingel, A., Gobbi, L.T.B., Papini, C.B., Nakamura,... Gobbi, S. (2013). Perceived barriers to leisure time physical activity: What Brazilians have to say? Open Journal of Preventive Medicine, 3, 491-499.
- Seghers, J., Spaepen, A., Delecluse, C., & Colman, V. (2003). Habitual level of physical activity and muscle fatigue of the elbow flexor muscles in older men. European Journal of Applied Physiology, 89, 427-434.
- Shigematsu, R., & Okura, T. (2006). A novel exercise for improving lower-extremity functional fitness in the elderly. Aging Clinical and Experimental Research, 18, 242-248.
- Shigematsu, R., Okura, T., Nakagaichi, M., Tanaka, K., Sakai, T., Kitazumi, S., & Rantanen, T. (2008). Square-stepping exercise and fall risk factors in older adults: a single-blind, randomized controlled trial. Journal of Gerontology. Series A Biological Sciences and Medical Sciences, 63, 76-82.
- Shigematsu, R., Okura, T., Sakai, T., & Rantanen, T. (2008). Square-stepping exercise versus strength and balance training for fall risk factors. Aging Clinical and Experimental Research, 20, 19-24.
- Shumway-Cook, A., Baldwin, M., Polissar, N.L., & Gruber, W. (1997). Predicting the probability for falls in community-dwelling older adults. Physiotherapy, 77, 812-819.
- Shumway-Cook, A., Brauer, S., & Woollacott, M. (2000). Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Physiotherapy, 80, 896-903.
- Tennstedt, S., Howland, J., Lachman, M., Peterson, E., Kasten, L., & Jette, A. (1998). A randomized, controlled trial of a group intervention to reduce fear of falling and associated activity restriction in older adults. Journals of gerontology. Series B, Psychological sciences and social sciences, 53, P384-392.
- Teixeira, C.V.L., Gobbi, S., Pereira, J.R., Ueno, D.T., Shigematsu, R., Gobbi, L.T.B. (2013). Effect of square-stepping exercise and basic exercises on functional fitness of older adults. Geriatrics and Gerontology International, 13, 842-8
- Teri, L., Gibbons, L.E., McCurry, S.M., Logsdon, R.G., Buchner, D.M., Barlow, W.E., ... Larson, E.B. (2003). Exercise plus behavioral management in patients with Alzheimer disease: a randomized controlled trial. Journal of the American Medical Association, 290, 2015-2022.
- Tsang, W.W., & Hui-Chan, C.W. (2004). Effect of 4-and 8-wk intensive Tai Chi training on balance control in the elderly. Medicine and science in sports and exercise, 36, 648-657.
- Tu, W., Stump, T.E., Damush, T.M., & Clark, D.O. (2004). The effects of health and environment on exercise-class participation in older, urban women. Journal of Aging and Physical Activity, 12, 480-496.
- Unger, J.B., Johnson, C.A., & Marks, G. (1997). Functional decline in the elderly: evidence for direct and stress-buffering protective effects of social interactions and physical activity. Annals of Behavioral Medicine, 19, 152-160.
- Viccaro, L.J., Perera, S., & Studenski, S.A. (2011). Is timed up and go better than gait speed in predicting health, function, and falls in older adults? Journal of American Geriatric Society, 59, 887-892.
- Voorrips, L.E., Ravelli, A.C., Dongelmans, P.C., Deurenberg, P., & Van Staveren, W.A. (1991). A physical activity questionnaire for the elderly. Medicine and Science in Sports and Exercise, 23, 974-979.
-
Acknowledgments We would like to thank the Mie University (Japan), CPNq, Rio Claro City Hall, Prof. Dr. José Luiz Riani Costa and the Centro Dia do Idoso "Padre Casagrande.
Publication Dates
-
Publication in this collection
Oct-Dec 2014
History
-
Received
29 Mar 2013 -
Accepted
11 Sept 2014