ABSTRACT
BACKGROUND:
Prolonged monitoring increased our knowledge on gastroesophageal reflux (GER), and the disease became known as gastroesophageal reflux disease (GERD). Prolonged reflux monitoring permits the diagnosis of GERD when endoscopic findings are not enough to characterize it.
OBJECTIVE:
The objective of this paper is to review the current knowledge on impedance-pH monitoring, taking into account the published literature and the authors experience with 1,200 exams.
METHODS:
The different types of prolonged reflux monitoring, namely: conventional pHmetry, catheter-free pHmetry and impedance-pHmetry will be briefly described. The new possibilities of evaluation with impedance-pHmetry are emphasized, namely: the study of symptomatic patients in use of proton pump inhibitors (PPIs); evaluation of patients with symptoms suggestive of GERD although with normal endoscopy and normal pHmetry, diagnostic elucidation of patients with atypical symptoms or supra-esophageal symptoms, mainly chronic cough, study of patients complaining of belch, differentiating gastric and supra-gastric belching, and the proper work-up before anti-reflux surgery.
RESULTS:
When impedance was associated to pH monitoring, an impressive technological evolution became apparent, when compared to pH monitoring alone. The main advantages of impedance-pHmetry are: the ability to detect all types of reflux: acid, non-acid, liquid, gaseous. In addition, other important measurements can be made: the ability of the esophagus in transporting the bolus, the measurement of basal mucosal impedance and the evaluation of primary peristalsis post reflux.
CONCLUSION:
Impedance-pHmetry is a promising method, with great advantages over conventional pHmetry. The choice between these two types of monitoring should be very judicious. The authors suggest the importance of careful evaluation of each reflux episode by the physician responsible for the examination, necessary for the correct interpretation of the tracings.
HEADINGS:
Gastroesophageal reflux; Esophageal pH monitoring; Electric impedance
RESUMO
CONTEXTO:
A monitorização prolongada ampliou o conhecimento sobre o refluxo gastroesofágico; a afecção decorrente do mesmo, passou a ser designada por doença do refluxo gastroesofágico (DRGE). O estudo prolongado do refluxo viabiliza o diagnóstico da DRGE nos casos sem alterações endoscópicas suficientes para caracterização da afecção.
OBJETIVO:
O objetivo do presente trabalho é apresentar uma revisão sobre a monitorização do refluxo por impedâncio-pHmetria, ponderando-se os dados de literatura com a experiência dos autores com o método em 1.200 exames realizados.
MÉTODOS:
São apresentados detalhes dos diferentes tipos de monitorização prolongada do refluxo; ou seja, a pHmetria convencional, a pHmetria sem cateter e a impedâncio-pHmetria. Salientam-se as novas possibilidades de avaliação que a impedâncio-pHmetria propicia e suas principais indicações: estudo de pacientes que permanecem sintomáticos durante o tratamento do refluxo com antissecretores; análise de pacientes com sintomas sugestivos de DRGE que não apresentem esofagite ao exame endoscópico e que tenham pHmetria normal; esclarecimento diagnóstico de pacientes com sintomas atípicos e supraesofágicos - em especial na tosse crônica; estudo da eructação diferenciando-as em dois grupos: gástricas e supragástricas e no auxílio na indicação do tratamento cirúrgico do refluxo.
RESULTADOS:
A monitorização associando duas modalidades de avaliação: a impedancio-pHmetria representa evolução tecnológica expressiva em relação à modalidade baseada apenas na análise do pH (pHmetria). As principais vantagens da impedâncio-pHmetria são: possibilidade de avaliação de todas modalidades de refluxo; ou seja, ácido, não-ácido, líquido e gasoso e também a possibilidade de estudo de outras variáveis importantes; ou seja: capacidade de transporte do bolus, impedância basal do esôfago e peristalse pós refluxo.
CONCLUSÃO:
A impedancio-pHmetria é um método promissor, com grandes vantagens sobre a pHmetria convencional. A escolha do tipo de monitorização a ser utilizada, deve ser criteriosa. Os autores destacam a importância da análise cuidadosa de cada episódio de refluxo, pelo médico responsável pela execução do exame, para correta interpretação e valorização dos dados obtidos.
DESCRITORES:
Refluxo gastroesofágico; Monitoramento do pH esofágico; Impedância elétrica
INTRODUCTION
Prolonged reflux monitoring, introduced in clinical practice in the mid 70s, enlarged our knowledge on GER. Until then, reflux was recognized only when it provoked inflammation of the esophageal mucosa, identified during endoscopy. The disease caused by reflux, was then designated as reflux esophagitis. With the introduction of prolonged pH monitoring the quantification of reflux in healthy volunteers was established and named physiologic reflux. Reflux above this level was named pathologic reflux and classified according to body position, in three types: upright (the most common type), supine and combined. A large portion of patients with symptomatic pathologic reflux did not have esophagitis identified by endoscopy.
Therefore, the concept of this disease became known as GERD, which can be diagnosed by endoscopic changes suggestive of reflux such as erosive esophagitis and/or pathologic reflux, identified by prolonged reflux monitoring.
The initial monitoring tool in clinical use - esophageal pHmetry- identified only episodes of acid reflux. With the evolution of this method, represented by impedance-pH monitoring, other types of reflux such as non-acid and gaseous reflux were recognized. They can also provoke symptoms and are not shown by conventional pHmetry alone. The purpose of this paper is to review reflux monitoring by impedance-pHmetry, taking into account data of the literature, and the experience of the authors with this method in 1,200 exams.
TYPES OF PROLONGED REFLUX MONITORING
Prolonged reflux monitoring can be done by catheter pHmetry or by catheter-free pH testing, using a telemetric capsule placed by endoscopy in the distal esophagus; when associated with impedance (impedance-pHmetry), it identifies non-acid reflux (pH above 7) and slightly acid (pH between 4 and 7). Impedance-pH monitoring has excellent sensitivity (77%-100%) and specificity (85%-100%) for the diagnosis of pathologic reflux11. Hirano I, Richter JE, Practice Parameters Committee of the American College of Gastroenterology. ACG practice guidelines: esophageal reflux testing. Am J Gastroenterol. 2007;102:668-85.. Therefore, this method is considered the gold standard by many authors22. Lacy BE, Weiser K, Chertoff J, Fass R, Pandolfino JE, Richter JE, et al. The diagnosis of gastroesophageal reflux disease. Am J Med. 2010;123:583-92.,33. Richter JE. Diagnostic tests for gastroesophageal reflux disease. Am J Med Sci. 2003;326:300-8..
Standard catheter pHmetry
PHmetry is done through a catheter introduced trans-nasally, with one or more pH sensors. The distal sensor is positioned 5 cm above the upper limit of the lower esophageal sphincter (LES), previously identified by manometry. The catheter is connected to a portable data logger, that register pH data every 4 sec during a 18 to 24 hour period. The patient registers the beginning and end of meals, upright and supine periods, as well as the occurrence of symptoms. Acid reflux is defined as a fall of esophageal pH below 4; the time percentage of pH<4 during the total time is the most reliable measurement for the diagnosis of GERD, considering the upper limit of normal between 4% and 5.5%44. Leme EMO. Parte II - pHmetria Esofágica Prolongada. Nasi A, Michelsohn N, eds. São Paulo: Editora Roca; 2001..
Catheter-free pHmetry
Catheter-free pHmetry is done with a device, the size of a capsule, which is fixed to the esophageal mucosa, usually during endoscopy, 6 cm above the Z line55. Pandolfino JE, Richter JE, Ours T, Guardino JM, Chapman J, Kahrilas PJ. Ambulatory esophageal pH monitoring using a wireless system. Am J Gastroenterol . 2003;98:740-9.. This technique was developed, aiming to reduce patient discomfort, thereby permitting more prolonged monitoring, and increasing the sensitivity of the test, since the patient can go through normal daily activities without the discomfort of the trans-nasal catheter. Nevertheless, a Brazilian study published in 2012, showed that, although catheter-free revealed a larger percentage of time of reflux than conventional pHmetry, both methods were comparable in the diagnosis of pathologic reflux and its correlation with symptoms66. Azzam RS, Sallum RAA, Brandao JF, Navarro-Rodriguez T, Nasi A. Comparative study of two modes of gastroesophageal reflux measuring: conventional esophageal pH monitoring and wireless pH monitoring. Arq Gastroenterol. 2012;49:107-12..
Impedance-pHmetry
Esophageal impedance is a method that allows to follow the ante-grade (bolus transport) and retro-grade movements (reflux) of intraluminal contents77. Silny J. Intraluminal Multiple Electric Impedance Procedure for Measurement of Gastrointestinal Motility. Neurogastroenterol Motil. 1991;3:151-62.. When impedance is associated with pHmetry - esophageal impedance-pHmetry (imp-pH), we can evaluate the retrograde movement of the refluxed material, characterizing its physical and chemical nature. Therefore, we can determine if there is reflux, if it is liquid, gaseous or mixed, acid or non-acid, and mainly, to correlate symptoms with all types of reflux88. Shay S, Tutuian R, Sifrim D, Vela M, Wise J, Balaji N, et al. Twenty-four hour ambulatory simultaneous impedance and pH monitoring: A multicenter report of normal values from 60 healthy volunteers. Am J Gastroenterol . 2004;99:1037-43.,99. Sifrim D, Castell D, Dent J, Kahrilas PJ. Gastro-oesophageal reflux monitoring: review and consensus report on detection and definitions of acid, non-acid, and gas reflux. Gut. 2004;53:1024-31.. Since the method identifies reflux regardless of its pH, it can be done while on anti-secretory drugs.
The imp-pH catheter has the same diameter of the conventional pHmetry catheter (2 mm), with one or two pH sensors and six pairs of metallic electrodes, allowing several configurations. The catheter is connected to a portable data-logger, and this data is kept in a memory card. At the end of the examination, the data is transferred to a computer to be analyzed by a dedicated software.
The method is based on the measurement of alterations in the resistance to alternating electric current (measured in Ohms), which occur between pairs of metallic electrodes, distributed along the catheter, positioned inside the esophagus. The electric conductance is directly related to the concentration of ions inside the esophageal lumen. When the content has a high concentration of ions (food, saliva, gastric contents), the electrical conductivity is high, and therefore, the impedance is low. When the intraluminal contents have a low ionic concentration (absence of bolus or presence of air), the electrical conductivity is low and, therefore, the impedance is high. Observing the impedance changes along the catheter, we can verify if the direction of the bolus is ante-grade, such as during food ingestion, or retrograde, as occurs during reflux. When a pH sensor is attached to this catheter, we can identify the acid or non-acid nature of the refluxed material1010. Bredenoord AJ, Smout AJPM. Advances in motility testing--current and novel approaches. Nat Rev Gastroenterol Hepatol. 2013;10:463-72.. (Figure 1).
On the left, an intra-esophageal catheter is depicted; on the right, there is a graphic representation of a reflux episode mainly liquid (shown by the decrease in impedance), acid (demonstrated by the fall of pH in the lower tracing), with proximal extension up to the pharynx. It is also shown that this reflux episode is cleared by primary peristalsis, seen by the descending movement of liquid content.
MAIN INDICATIONS FOR IMPEDANCE-PHMETRY
Impedance-pHmetry is the method with the best sensitivity to detect all reflux episodes, as well as its distribution in the esophagus and pharynx, composition and clearance1111. Sifrim D, Holloway R, Silny J, Tack J, Lerut A, Janssens J. Composition of the postprandial refluxate in patients with gastroesophageal reflux disease. Am J Gastroenterol . 2001;96:647-55.
12. Shay SS, Bomeli S, Richter J. Multichannel intraluminal impedance accurately detects fasting, recumbent reflux events and their clearing. Am J Physiol Gastrointest Liver Physiol. 2002;283:G376-83.-1313. Sifrim D, Silny J, Holloway RH, Janssens JJ. Patterns of gas and liquid reflux during transient lower oesophageal sphincter relaxation: a study using intraluminal electrical impedance. Gut. 1999;44:47-54.. It was validated in the detection of acid reflux, identifying 97% to 98% of acid refluxes detected by pHmetry, not only in patients with GERD, but also in healthy controls, and in the identification of non-acid refluxes, detecting more than 93% of non-acid refluxes and in superimposed refluxes (“re-reflux”). This method, nevertheless, does not allow detection of very small volume refluxes (<1mL); but such episodes are less frequent in clinical practice. Next are the main indications and advantages of the method.
Assessment of non-acid reflux
As already mentioned, esophageal pHmetry evaluates properly acid GER, but is not so with non-acid reflux. About 30% of patients continue having symptoms, in spite of anti-secretory drugs, have their symptoms due to non-acid reflux, not detected by conventional pHmetry. The term non-acid reflux is not very precise, since the majority of these refluxes have pH between 4 and 7. This aspect was discussed in an international consensus on the definition of reflux, and it was suggested that the term non-acid reflux should be used when pH is above 7, and refluxes with pH between 4 and 7 should be called slightly acidic refluxes99. Sifrim D, Castell D, Dent J, Kahrilas PJ. Gastro-oesophageal reflux monitoring: review and consensus report on detection and definitions of acid, non-acid, and gas reflux. Gut. 2004;53:1024-31.. Nonetheless, in clinical practice the term non-acid is used whenever a reflux has pH>4, all of them not detected by conventional pHmetry.
Several studies in adults and children, indicate that impedance-pHmetry is the gold standard for the diagnosis of GER. Tutuian R and Castell DO, in a review on this subject1414. Tutuian R, Castell DO. Use of multichannel intraluminal impedance to document proximal esophageal and pharyngeal nonacidic reflux episodes. Am J Med. 2003; Suppl 3A:119S-123S., claim that the presence and proximal extension of non-acid reflux (which occur mainly in the post-prandial period when gastric acidity can be neutralized by food, and during treatment with anti-secretory drugs), can now be adequately studied. The possibility of correlating clinical symptoms and non-acid reflux is of great value, especially in patients who remain symptomatic while in use of anti-secretory drugs.
Other methods for the detection of non-acid reflux (scintigraphy and bilimetry) have several limitations. Scintigraphy involves radiation and can only be done over short periods of time, allowing a momentaneous analysis of reflux. Bilimetry does not correlate well with intra-gastric pH, and does not detect reflux without bilirubin, which amounts to more than 90% of non-acid refluxes1515. Just RJ, Leite LP, Castell DO. Changes in overnight fasting intragastric pH show poor correlation with duodenogastric bile reflux in normal subjects. Am J Gastroenterol . 1996;8:1567-70.. Pace F et al.1616. Pace F, Sangaletti O, Pallotta S, Molteni P, Porro GB. Biliary reflux and non-acid reflux are two distinct phenomena: A comparison between 24-hour multichannel intraesophageal impedance and bilirubin monitoring. Scand J Gastroenterol. 2007;42:1031-9., evaluating bilimetry together with impedance-pH, noted that there is no significant relation between bile reflux and non-acid reflux. The majority of bile reflux are associated with acid reflux.
Assessment of proximal extension and composition of reflux
Regarding proximal extension, refluxes are limited to the distal esophagus, or ascend proximally to the upper esophagus. Neither pHmetry, nor impedance-pHmetry can measure volume. The measurement of proximal extension is a surrogate for volume, since larger volume of reflux, occupying more space, extends proximally. This measurement of proximal extension (by impedance) is important, since there are symptoms that are not due to its acidity, but to the volume of refluxed material, such as regurgitation, chest pain and cough. Moreover, the increased proximal extension of reflux can be the reason of refractory symptoms in patients with hypersensitive esophagus1717. Rohof WO, Bennink RJ, de Jonge H, Boeckxstaens GE. Increased Proximal Reflux in a Hypersensitive Esophagus Might Explain Symptoms Resistant to Proton Pump Inhibitors in Patients With Gastroesophageal Reflux Disease. Clin Gastroenterol Hepatol. 2014;12:1647-55..
Regarding the composition of reflux, we observe a similar proportion of liquid (51%) and mixed refluxes (49%). Regarding esophageal clearance, it is noted that the necessary time to pH to return to a level above 4, is twice longer than the time to impedance to return to previous level. There are some publications on normal values for imp-pH; among them we emphasize: Zerbib F et al., with 68 asymptomatic controls1818. Zerbib F, des Varannes SB, Roman S, Pouderoux P, Artigue F, Chaput U, et al. Normal values and day-to-day variability of 24-h ambulatory oesophageal impedance-pH monitoring in a Belgian-French cohort of healthy subjects. Aliment Pharmacol Ther. 2005;22:1011-21. and Zentilin P et al., with 25 controls1919. Zentilin P, Iiritano E, Dulbecco P, Bilardi C, Savarino E, De Conca S, et al. Normal values of 24-h ambulatory intraluminal impedance combined with pH-metry in subjects eating a Mediterranean diet. Dig Liver Dis. 2006;38:226-32..
It is important to stress that symptoms often do not depend on the chemical composition of the reflux, but on its physical composition (liquid, gaseous or mixed content). In these cases, symptoms are not due to stimulation of chemoreceptors, but on mechanoreceptors. The association of symptoms with gaseous distention, can only be detected by impedance-pHmetry. It is worth mentioning that gaseous content of reflux is an important factor in the proximal extension and development of extra-esophageal complaints.
Imp-pH also permits the diagnosis of “re-reflux” (superimposed acid reflux). It represents a new episode of reflux that occurs while the pH is still below 4. Conventional pHmetry can not distinguish a “re-reflux” from a prolonged reflux episode2020. Shay SS, Johnson LF, Richter JE. Acid rereflux: A review, emphasizing detection by impedance, manometry, and scintigraphy, and the impact on acid clearing pathophysiology as well as interpreting the pH record. Dig Dis Sci. 2003;48:1-9.. Acid reflux is twice more frequent than non-acid reflux, and superimposed reflux (“re-reflux”) occurs in an even smaller frequency.
Assessment of patients with refractory symptoms in spite of anti-secretory drugs
When imp-pH is indicated in the evaluation of patients not responding well to the use of anti-secretory drugs, the exam should be preferably done during treatment to establish if symptoms are due to acid reflux not adequately blocked, if symptoms are due to non-acid reflux, or not due to reflux at all. In a classic study with imp-pH in symptomatic patients in spite of anti-secretory drugs, it was shown that 11% of them had their symptoms due to acid reflux not adequately neutralized by anti-secretory drugs (these cases could be identified by conventional pHmetry). Nevertheless, 37% of patients had symptoms related to non-acid reflux (detectable only by impedance-pH). In the remaining 52% of the patients, symptoms were not related to reflux2121. Mainie I, Tutuian R, Shay S, Vela M, Zhang X, Sifrim D, Castell DO. Acid and non-acid reflux in patients with persistent symptoms despite acid suppressive therapy: A multicentre study using combined ambulatory impedance-pH monitoring. Gut. 2006;55:1398-402..
When imp-pH is indicated for the diagnosis of GERD, it is preferable to withhold medication for at least one week. By doing so, we can assess the total number of refluxes and their distribution in acid or non-acid. We can determine the percentage of time of acid exposure, which is considered pathologic when greater than 6%. Another reason is that with a tendency for an increase in the number of symptoms when off medication, there is a greater chance for symptom correlation with reflux.
When evaluating asymptomatic controls without anti-secretory drugs, it is noted that 2/3 of reflux is acid and 1/3 is non-acid. When patients are taking anti-secretory drugs, we do not notice a significant reduction in the total number of reflux episodes, but there is a significant change in the distribution, and non-acid refluxes predominate.
Vela et al., in a classic publication on this subject2222. Vela MF, Camacho-Lobato L, Srinivasan R, Tutuian R, Katz PO, Castell DO. Simultaneous intraesophageal impedance and pH measurement of acid and nonacid gastroesophageal reflux: Effect of omeprazole. Gastroenterology. 2001;120:1599-606., evaluated the effect of omeprazole in 12 patients, submitted to impedance-pHmetry, before and during the use of this drug. They observed that before treatment, 55% of the refluxes were non-acid and 45% were acid. During the use of omeprazole, the total number of reflux was the same, but there was a great change in the distribution; 97% of the refluxes became non-acid, and 3% remained acid.
Evaluation of atypical symptoms
Ambulatory impedance-pH monitoring has become a great diagnostic tool in the evaluation of atypical GERD symptoms like chronic cough and belching.
According to a systematic review and meta-analysis of randomised controlled trials 21% to 41% of chronic cough without an underlying respiratory disease is associated with gastro-oesophageal reflux2323. Chang AB, Lasserson TJ, Kiljander TO, Connor FL, Gaffney JT, Garske LA. Systematic review and meta-analysis of randomised controlled trials of gastro-oesophageal reflux interventions for chronic cough associated with gastro-oesophageal reflux. BMJ. 2005;332:11-17.. Sifrim et al.2424. Sifrim D, Dupont L, Blondeau K, Zhang X, Tack J, Janssens J. Weakly acidic reflux in patients with chronic unexplained cough during 24 hour pressure, pH, and impedance monitoring. Gut. 2005;54:449-54. analyzing 22 patients suffering from chronic cough has observed that 22.7% had chronic cough related to acid reflux, 13.6% related to weakly acid reflux and 9% related to both. In this study, the ability in determination of temporal association between cough and reflux was observed in 31.5% for pH-monitoring alone and in 45.5% for impedance-pH. Besides, a subgroup of patients with chronic cough clearly associated with weakly acidic reflux was identified. In another case series, the same author analyzed a total of 100 patients with chronic cough. It was demonstrated that acid reflux could be a potential mechanism for cough in 45 patients, weakly acidic reflux could be a potential mechanism for cough in 24 patients and reflux could not be identified as a potential mechanism for cough in 31 patients2525. Blondeau K, Dupont LJ, Mertens V, Tack J, Sifrim D. Improved diagnosis of gastro-oesophageal reflux in patients with unexplained chronic cough. Aliment Pharmacol Ther . 2007;25:723-32..
One of the mechanisms that have been proposed to explain unexplained chronic cough refractory to PPI is the occurrence of esophageal distension by weakly acidic reflux2121. Mainie I, Tutuian R, Shay S, Vela M, Zhang X, Sifrim D, Castell DO. Acid and non-acid reflux in patients with persistent symptoms despite acid suppressive therapy: A multicentre study using combined ambulatory impedance-pH monitoring. Gut. 2006;55:1398-402.. Impedance-pH-monitoring identified patients in whom cough can be related to reflux that would have been disregarded using the standard diagnostic criteria for acid reflux.
In patients with excessive belching, impedance-pH can differentiate patients who present belching from the gas content of the stomach through the esophagus, those who expulse swallowed air and those who expulse air stored in the esophagus itself. Such differentiation is important in therapeutic management.
Belching (eructation) is classically defined as a physiological mechanism that prevents the accumulation of gas in the stomach due to the venting of the accumulated intragastric air into the esophagus followed by oral expulsion2626. Wyman JB, Dent J, Heddle R, Dodds WJ, Toouli J, Downton J. Control of belching by the lower oesophageal sphincter. Gut. 1990;31:639-46.. However, with the use of esophageal impedance monitoring, supragastric belching has been identified. During this type of belch, air is rapidly brought into the esophagus and immediately followed by a rapid expulsion. Impedance tracers demonstrate an increase in impedance level starting in the proximal channel and progressing to the most distal channel. The air is then cleared from the esophagus in oral direction that is seen as a return to the baseline impedance level, starting in the most distal channel and progressing to the proximal channel. On the other hand, gastric belch is characterized by an increase in impedance level starting in the distal channel and progressing to the most proximal channel accompanied by lower esophageal sphincter relaxation2727. Kessing BF, Bredenoord AJ, Smout AJPM. The pathophysiology, diagnosis and treatment of excessive belching symptoms. Am J Gastroenterol . 2014;10(8)..
Differential diagnosis of functional disorders
Symptomatic reflux, abnormal acid exposure, and mucosal acid sensitivity are separate, though related, aspects of GERD. It is known that 10%-40% of patients presenting heartburn do not respond to proton pump inhibitor (PPI) use and that a proportion of those patients have normal esophageal acid exposure and no correlation between reflux events and symptoms2828. Fass R, Sifrim D. Management of heartburn not responding to proton pump inhibitors. Gut. 2009;58:295-309.. This group is named “functional heartburn”2929. Hachem C, Shaheen NJ. Diagnosis and Management of Functional Heartburn. Am J Gastroenterol . 2016;111:53-61..
According to Rome IV criteria, diagnosis of functional heartburn must include all of the following: burning retrosternal discomfort or pain; no symptom relief despite optimal antisecretory therapy; absence of evidence that gastroesophageal reflux or EoE is the cause of symptoms and absence of major esophageal motor disorders3030. Aziz Q, Fass R, Gyawali CP, Miwa H, Pandolfino JE, Zerbib F. Esophageal disorders. Gastroenterology. 2016;150:1368-79..
In other hand, reflux hypersensitivity refers to patients with esophageal symptoms (heartburn or chest pain) triggered by physiologic reflux3030. Aziz Q, Fass R, Gyawali CP, Miwa H, Pandolfino JE, Zerbib F. Esophageal disorders. Gastroenterology. 2016;150:1368-79..
Thus, it is observed that imp-pH is essential for the diagnosis of functional heartburn and hypersensitivity to reflux3030. Aziz Q, Fass R, Gyawali CP, Miwa H, Pandolfino JE, Zerbib F. Esophageal disorders. Gastroenterology. 2016;150:1368-79.. Classifying patients with symptomatic nonacid reflux as having a hypersensitive esophagus decreases the number of patients with functional heartburn3131. Savarino E, Zentilin P, Tutuian R, Pohl D, Casa DD, Frazzoni M, et al. The role of nonacid reflux in NERD: Lessons learned from impedance-pH monitoring in 150 patients off therapy. Am J Gastroenterol . 2008;103:2685-93.. This characterization is important considering that patients with functional heartburn may not respond to anti-secretory drugs2929. Hachem C, Shaheen NJ. Diagnosis and Management of Functional Heartburn. Am J Gastroenterol . 2016;111:53-61..
Identification of candidates for surgical treatment
It is well established that GERD is a disease of acid escape and not acid production and that transient lower esophageal sphincter relaxation (TLESR) is one of the main mechanism of gastroesophageal reflux disease. Although TLESRs number are not consistently increased in GERD patients compared to controls, it is known that TLESRs are more frequently associated with reflux episodes in GERD patients3232. Iwakiri K, Hayashi Y, Kotoyori M, Tanaka Y, Kawakami A, Sakamoto C, Holloway RH. Transient lower esophageal sphincter relaxations (TLESRs) are the major mechanism of gastroesophageal reflux but are not the cause of reflux disease. Dig Dis Sci . 2005;50:1072-7.,3333. Trudgill NJ, Riley SA. Transient lower esophageal sphincter relaxations are no more frequent in patients with gastroesophageal reflux disease than in asymptomatic volunteers. Am J Gastroenterol . 2001;96(Suppl.9):2569-2574..
Fundoplication results in significant decrease in TLESR frequency compared to GERD and normal patients, and less TLESRs associated with reflux events3434. Kessing BF, Bredenoord AJ, Schijven MP, van der Peet DL, van Berge Henegouwen MI, Smout AJPM. Long-term effects of anti-reflux surgery on the physiology of the esophagogastric junction. Surg Endosc Other Interv Tech. 2015;29:3726-32.. Moreover, fundoplication can restore the disrupted anatomy of esophagogastric junction (EGJ) in case of hiatus hernia. However, because of the invasive nature of the operation, it is not considered as first-line therapy to GERD patients. Thus, patient selection is the key role for surgery success. The best candidates are those with typical symptoms who respond to PPI therapy3535. Campos GM, Peters JH, DeMeester TR, Oberg S, Crookes PF, Tan S, et al. Multivariate analysis of factors predicting outcome after laparoscopic Nissen fundoplication. J Gastrointest Surg. 1999;3:292-300.. However, non-responders can also be candidates when they have positive correlation between symptoms and acid or weakly acid reflux. In a study of 200 patients with persistent symptoms despite PPIs twice daily, 18 patients with positive correlation of symptoms with reflux underwent laparoscopic Nissen fundoplication. Seven of these patients complaining of chronic cough had their symptoms related to non-acid reflux, and all of them remained asymptomatic at 14 months follow-up3636. Mainie I, Tutuian R, Agrawal A, Adams D, Castell DO. Combined multichannel intraluminal impedance-pH monitoring to select patients with persistent gastro-oesophageal reflux for laparoscopic Nissen fundoplication. Br J Surg. 2006;93:1483-7.. This indicates that, unlike the treatment with antisecretor3636. Mainie I, Tutuian R, Agrawal A, Adams D, Castell DO. Combined multichannel intraluminal impedance-pH monitoring to select patients with persistent gastro-oesophageal reflux for laparoscopic Nissen fundoplication. Br J Surg. 2006;93:1483-7.,3737. Tutuian R, Mainie I, Agrawal A, Adams D, Castell DO. Nonacid reflux in patients with chronic cough on acid-suppressive therapy. Chest. 2006;130:386-91., surgical management can also treat non-acid reflux.
Imp-pH could also demonstrate that the drugs used to reduce transient relaxation of the esophageal lower sphincter, especially baclofen, reduce the total number of reflux episodes and not only change their chemical composition, as do the antisecretor3838. Vela MF, Tutuian R, Katz PO, Castell DO. Baclofen decreases acid and non-acid post-prandial gastro-oesophageal reflux measured by combined multichannel intraluminal impedance and pH. Aliment Pharmacol Ther . 2003;17:243-51.. However, their important side effects may limit their clinical use.
AUTHORS’ EXPERIENCE WITH THE METHOD
We have started the use of imp-pH in 2005 carrying out 1,200 procedures. We advocate that the main indication of the method is the study of symptoms refractory to the clinical treatment of GERD. Analyzing a series of 20 consecutive patients, with predominant typical complaints, we observed that 19 (95%) had symptoms during the examination; (31.6%) with no reflux, 6 (31.6%) related to non-acid reflux, 6 (31.6%) related to non-acid reflux and 2 (10.5%) related with both. Roughly, we can say that among patients with refractory GERD, 1/3 has symptoms due to acid reflux, 1/3 due to non-acid reflux and in 1/3 it is not possible to relate persistent symptoms to any reflux modality.
In our series, the main indications of the method were: antisecretors symptom refractory patients, atypical or extraesophageal complaints and patients with clinical suspicion of GERD not confirmed by endoscopy or by conventional pHmetry. Kline MM et al.3939. Kline MM, Ewing M, Simpson N, Laine L. The Utility of Intraluminal Impedance in Patients With Gastroesophageal Reflux Disease-Like Symptoms But Normal Endoscopy and 24-Hour pH Testing. Clin Gastroenterol Hepatol . 2008;6:880-85. evaluating 37 patients with typical GERD symptoms with normal endoscopy and pHmetry, have found that 10 (27%) presented acid reflux and 14 (38%) acid reflux and non-acid reflux symptoms demonstrating incremental value of imp-pH over conventional pHmetry in diagnostic performance.
Additional advantages of impedance-pH versus pHmetry
A recently published consensus on the diagnosis of GERD, Lyon consensus4040. Gyawali CP, Kahrilas PJ, Savarino E, Zerbib F, Mion F, Smout AJPM, et al. Modern diagnosis of GERD: the Lyon Consensus. Gut. 2018:67:1351-62., interesting statements are set regarding the monitoring of GERD. The authors advocated that the most relevant parameter in monitoring by pHmetry is the percentage of total reflux time; percentages above 6 should be considered pathological, less than 4 physiological and between 4 and 6 inconclusive. Regarding imp-pH monitoring, the number of episodes of reflux has been highlighted; pathological over 80, physiological below 40 and inconclusive between 40 and 80. The authors have emphasized that imp-pH, considering all reflux modalities, has a greater chance of relating clinical symptoms with reflux than conventional pH monitoring. Three additional advantages of imp-pH monitoring in relation to conventional pHmetry are pointed out: analysis of bolus transport, basal esophageal impedance and post reflux peristalsis. We have evaluated the transport of the bolus since the beginning of our experience; and, in the last three years, we added the analysis of baseline impedance and peristalsis post reflux in all performed procedures. The importance of these three measurements is demonstrated as follows.
Analysis of the bolus transport
At the beginning of recording, with the patient in recumbent position, 10 oral instillations of 5 ml of saline are made, 30 seconds interval between them. The following day, after removal of the equipment, it is verified, by impedance, if there is complete transport of the bolus. Adequate transport of at least eight (80.0%) of the swallows studied is considered normal4141. Hila A, Chowdhury N, Hajar N, Castell DO. Swallow evaluation during multichannel intraluminal impedance and pH: An alternate method to assess esophageal transit. J Clin Gastroenterol. 2011;45:862-6.. Figure 2 shows an adequate transport record of the ingested bolus. This information is important in the preoperative evaluation, since complete bolus transport is indicative of the efficacy of the contractile activity of the esophagus, even if there is hypocontractility of the esophageal body on manometric study.
In our experience, retrospectively reviewing the last 1,000 cases, we found abnormal bolus transport (<80%) in 31 (3.1%) cases. There were several causes for impairment of bolus transport; among them: relevant motor disorders of the esophagus, dysphagia after fundoplication and large gastric herniations. In 12 (1.2%) cases the analysis of the bolus transport was impaired by very low baseline impedance in the esophageal body. The most common causes for the difficulty of bolus transport analysis due to low baseline impedance were: long Barrett’s esophagus, esophageal involvement due to collagen disease and megaesophagus. In our view, the study of bolus transport by impedance-pHmetry provides important reference information; however, it does not represent a specific and sensitive method for definitive characterization of esophageal transport function. For a more specific analysis of this question, a radiological contrast study is recommended. A radiological contrast study of the esophagus can be performed in two ways: conventional and dynamic. The dynamic study, with film of the passage of contrast material through the esophagus, has a higher diagnostic sensitivity than the conventional study.
Basal impedance
When the esophagus is empty, the intraluminal impedance recorded corresponds to that of the esophageal mucosa. In the presence of active inflammation of the same, Barrett’s esophagus and esophageal involvement in collagenosis, the basal impedance is very much reduced. Therefore, by the analysis of the basal impedance (BI) one can infer about the integrity of the mucosa. In the presence of liquid-alimentary residue in the esophagus, the baseline impedance is also reduced, impeding adequate evaluation of reflux4242. Kandulski A, Weigt J, Caro C, Jechorek D, Wex T, Malfertheiner P. Esophageal Intraluminal Baseline Impedance Differentiates Gastroesophageal Reflux Disease From Functional Heartburn. Clin Gastroenterol Hepatol . 2015;13:1075-81.. Figure 3 shows a record of both low and normal BI in the lower esophagus. The BI should be evaluated during sleep, when the impedance is more stable, as there are fewer refluxes and deglutition. This is calculated as an average of three periods of 10 minutes.
In our experience, it has been noted that low baseline impedance makes it difficult to interpret reflux episodes; however, we have observed a relationship between the percentage of exposure time to acid and baseline impedance and also that the reduced BI tends to normalize with anti-secretory use. Baseline impedance has been considered a good marker of esophageal mucosal lesion4343. Kessing BF, Bredenoord AJ, Weijenborg PW, Hemmink GJM, Loots CM, Smout AJPM. Esophageal acid exposure decreases intraluminal baseline impedance levels. Am J Gastroenterol . 2011;106:2093-7..
Mucosal integrity and BI are longitudinal evidences, that is, over time, reflects exposure to acid. Reduced BI, in the absence of stasis, indicates impairment of esophageal mucosal integrity. Obviously, mucosal integrity can also be assessed by upper digestive endoscopy; however, it must be emphasized that there may be involvement of the mucosa without visible endoscopic alterations. When biopsies are performed to identify microscopic esophagitis, mucosal integrity can be assessed in greater detail. However, macroscopic esophagitis may be present in up to 15% of healthy individuals4444. Vaezi MF, Sifrim D. Assessing Old and New Diagnostic Tests for Gastroesophageal Reflux Disease. Gastroenterology. 2018;154:289-301..
Peristalse post reflux
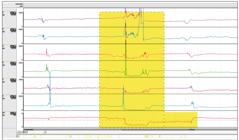
Here we stop worrying only about the reflux and we begin to worry about what happens after the reflux, that is, with its clearance. It is known that acid reflux triggers esophageal-salivary reflex4545. Woodley FW, Fernandez S, Mousa H. Diurnal Variation in the Chemical Clearance of Acid Gastroesophageal Reflux in Infants. Clin Gastroenterol Hepatol . 2007;5:37-43.. After an episode of reflux, one can identify, by impedance-pH, whether there is esophageal peristalsis. By analyzing the reflux episodes individually, we observed how many elicited esophageal peristalsis in the 30 seconds following reflux. With this, one can analyze the percentage of refluxes that trigger peristalsis after reflux; that is, the so-called post reflux peristalsis index (PRPI). Initial publications on the subject have pointed out that this index reflects the capacity of clearance of the esophagus. Normal indices (greater than or equal to 61%) suggest good capacity of esophageal clearance of the refluxed material. Relating this index to the degree of mucosal lesion, lower rates of erosive GERD, intermediate non-erosive and normal asymptomatic controls have been noted4646. Frazzoni M, Savarino E, de Bortoli N, Martinucci I, Furnari M, Frazzoni L, et al. Analyses of the Post-reflux Swallow-induced Peristaltic Wave Index and Nocturnal Baseline Impedance Parameters Increase the Diagnostic Yield of Impedance-pH Monitoring of Patients With Reflux Disease. Clin Gastroenterol Hepatol . 2016;14:40-6.. Figure 4 shows post-reflux peristalsis promoting acidity clearance of reflux.
It has been noted that the rate of peristalsis post reflux is more reduced in patients with Barrett’s esophagus with dysplasia4747. Frazzoni M, Bertani H, Conigliaro R, Frazzoni L, Losi L, Melotti G. Neoplastic progression in short-segment Barrett’s oesophagus is associated with impairment of chemical clearance, but not inadequate acid suppression by proton pump inhibitor therapy. Aliment Pharmacol Ther . 2014;40:835-42.. Barrett’s neoplastic degeneration seems to relate more to low PRPI than to inadequate response to antisecretors. Quantifying reflux may be dispensable in Barrett because the diagnosis is already established; however, the evaluation of PRPI may justify the achievement of impedance-pH in these cases. The evaluation of PRPI is also important in patients who undergo lung transplantation; the risk of rejection is greater when there is reduced PRPI4848. Tangaroonsanti A, Jones DR, Lee AS, Vela MF, DeVault KR, Houghton LA. 534 Post-Reflux Swallow-Induced Peristaltic Wave (PSPW) Index, a Measure of Esophageal Chemical Clearance Is a Predicator of Allograph Failure After Lung Transplantation. Gastroenterology. 2016;150:S111-S112. Doi: https://doi.org/10.1016/S0016-5085(16)30480-2.
https://doi.org/https://doi.org/10.1016/...
. The measurement of the PRPI has not yet been incorporated into the software; therefore, careful visual analysis of all acid or mildly acid reflux episodes is necessary. Episodes of gas reflux are not considered in the calculation of PRPI because they do not trigger esophageal-salivary reflux.
INDICATIONS OF IMPEDANCE-PHMETRY
-
Study of patients who remain symptomatic during the treatment of reflux with anti-secretory drugs. In these cases, the test should be performed during the period on medication.
-
Patients with symptoms suggestive of GERD who do not present esophagitis at endoscopic examination and who have normal pHmetry. In these cases, the test should be performed without the use of anti-secretory agents.
-
Diagnostic clarification of patients with atypical symptoms and supra-esophageal symptoms, not explained by other causes. Principally: coughing and belching.
-
Assistance in the indication of surgical treatment of reflux.
CONCLUSION
Prolonged monitoring increased knowledge about gastroesophageal reflux; the condition resulting from it, has been renamed Gastroesophageal reflux disease. Monitoring allows the diagnosis of GERD in cases without sufficient endoscopic alterations to characterize the condition.
The choice of the type of monitoring to be used should be judicious. The main advantages of impedance-pHmetry to pH-monitoring alone are: the possibility of evaluating all reflux modalities; i.e. acid, non-acid, liquid and gaseous and also the possibility of studying other important variables; i.e., bolus transport capacity, basal impedance of the esophagus and peristalsis post reflux.
The main indications of impediment-pH monitoring in clinical practice are: the study of symptoms refractory to the clinical treatment of GERD, the study of atypical reflux manifestations; among them, in particular, the chronic cough and the study of the eructations differentiating them in gastric and supragastrics.
Our experience with the method is encouraging. It should be noted, however, that the method is much more labor intensive than conventional pHmetry. The automatic reflux analysis by the computer program often misinterprets impedance traces, considering as reflux what in reality is an anterograde flow (deglutition). Therefore, one should analyze all episodes referred to as reflux for correct interpretation; only the retrograde propagation pattern is indicative of reflux. The characterization of the reflux should not be left on account of the computer program. Finally, it is emphasized that the study of the bolus transport capacity, the measurement of the nocturnal basal impedance and the post reflux peristalsis have become important components of the prolonged monitoring of impedance-pH monitoring4949. Smits MJ, Loots CM, van Wijk MP, Bredenoord AJ, Benninga MA, Smout AJPM. An expert panel-based study on recognition of gastro-esophageal reflux in difficult esophageal pH-impedance tracings. Neurogastroenterol Motil . 2015;27:637-45..
REFERENCES
-
1Hirano I, Richter JE, Practice Parameters Committee of the American College of Gastroenterology. ACG practice guidelines: esophageal reflux testing. Am J Gastroenterol. 2007;102:668-85.
-
2Lacy BE, Weiser K, Chertoff J, Fass R, Pandolfino JE, Richter JE, et al. The diagnosis of gastroesophageal reflux disease. Am J Med. 2010;123:583-92.
-
3Richter JE. Diagnostic tests for gastroesophageal reflux disease. Am J Med Sci. 2003;326:300-8.
-
4Leme EMO. Parte II - pHmetria Esofágica Prolongada. Nasi A, Michelsohn N, eds. São Paulo: Editora Roca; 2001.
-
5Pandolfino JE, Richter JE, Ours T, Guardino JM, Chapman J, Kahrilas PJ. Ambulatory esophageal pH monitoring using a wireless system. Am J Gastroenterol . 2003;98:740-9.
-
6Azzam RS, Sallum RAA, Brandao JF, Navarro-Rodriguez T, Nasi A. Comparative study of two modes of gastroesophageal reflux measuring: conventional esophageal pH monitoring and wireless pH monitoring. Arq Gastroenterol. 2012;49:107-12.
-
7Silny J. Intraluminal Multiple Electric Impedance Procedure for Measurement of Gastrointestinal Motility. Neurogastroenterol Motil. 1991;3:151-62.
-
8Shay S, Tutuian R, Sifrim D, Vela M, Wise J, Balaji N, et al. Twenty-four hour ambulatory simultaneous impedance and pH monitoring: A multicenter report of normal values from 60 healthy volunteers. Am J Gastroenterol . 2004;99:1037-43.
-
9Sifrim D, Castell D, Dent J, Kahrilas PJ. Gastro-oesophageal reflux monitoring: review and consensus report on detection and definitions of acid, non-acid, and gas reflux. Gut. 2004;53:1024-31.
-
10Bredenoord AJ, Smout AJPM. Advances in motility testing--current and novel approaches. Nat Rev Gastroenterol Hepatol. 2013;10:463-72.
-
11Sifrim D, Holloway R, Silny J, Tack J, Lerut A, Janssens J. Composition of the postprandial refluxate in patients with gastroesophageal reflux disease. Am J Gastroenterol . 2001;96:647-55.
-
12Shay SS, Bomeli S, Richter J. Multichannel intraluminal impedance accurately detects fasting, recumbent reflux events and their clearing. Am J Physiol Gastrointest Liver Physiol. 2002;283:G376-83.
-
13Sifrim D, Silny J, Holloway RH, Janssens JJ. Patterns of gas and liquid reflux during transient lower oesophageal sphincter relaxation: a study using intraluminal electrical impedance. Gut. 1999;44:47-54.
-
14Tutuian R, Castell DO. Use of multichannel intraluminal impedance to document proximal esophageal and pharyngeal nonacidic reflux episodes. Am J Med. 2003; Suppl 3A:119S-123S.
-
15Just RJ, Leite LP, Castell DO. Changes in overnight fasting intragastric pH show poor correlation with duodenogastric bile reflux in normal subjects. Am J Gastroenterol . 1996;8:1567-70.
-
16Pace F, Sangaletti O, Pallotta S, Molteni P, Porro GB. Biliary reflux and non-acid reflux are two distinct phenomena: A comparison between 24-hour multichannel intraesophageal impedance and bilirubin monitoring. Scand J Gastroenterol. 2007;42:1031-9.
-
17Rohof WO, Bennink RJ, de Jonge H, Boeckxstaens GE. Increased Proximal Reflux in a Hypersensitive Esophagus Might Explain Symptoms Resistant to Proton Pump Inhibitors in Patients With Gastroesophageal Reflux Disease. Clin Gastroenterol Hepatol. 2014;12:1647-55.
-
18Zerbib F, des Varannes SB, Roman S, Pouderoux P, Artigue F, Chaput U, et al. Normal values and day-to-day variability of 24-h ambulatory oesophageal impedance-pH monitoring in a Belgian-French cohort of healthy subjects. Aliment Pharmacol Ther. 2005;22:1011-21.
-
19Zentilin P, Iiritano E, Dulbecco P, Bilardi C, Savarino E, De Conca S, et al. Normal values of 24-h ambulatory intraluminal impedance combined with pH-metry in subjects eating a Mediterranean diet. Dig Liver Dis. 2006;38:226-32.
-
20Shay SS, Johnson LF, Richter JE. Acid rereflux: A review, emphasizing detection by impedance, manometry, and scintigraphy, and the impact on acid clearing pathophysiology as well as interpreting the pH record. Dig Dis Sci. 2003;48:1-9.
-
21Mainie I, Tutuian R, Shay S, Vela M, Zhang X, Sifrim D, Castell DO. Acid and non-acid reflux in patients with persistent symptoms despite acid suppressive therapy: A multicentre study using combined ambulatory impedance-pH monitoring. Gut. 2006;55:1398-402.
-
22Vela MF, Camacho-Lobato L, Srinivasan R, Tutuian R, Katz PO, Castell DO. Simultaneous intraesophageal impedance and pH measurement of acid and nonacid gastroesophageal reflux: Effect of omeprazole. Gastroenterology. 2001;120:1599-606.
-
23Chang AB, Lasserson TJ, Kiljander TO, Connor FL, Gaffney JT, Garske LA. Systematic review and meta-analysis of randomised controlled trials of gastro-oesophageal reflux interventions for chronic cough associated with gastro-oesophageal reflux. BMJ. 2005;332:11-17.
-
24Sifrim D, Dupont L, Blondeau K, Zhang X, Tack J, Janssens J. Weakly acidic reflux in patients with chronic unexplained cough during 24 hour pressure, pH, and impedance monitoring. Gut. 2005;54:449-54.
-
25Blondeau K, Dupont LJ, Mertens V, Tack J, Sifrim D. Improved diagnosis of gastro-oesophageal reflux in patients with unexplained chronic cough. Aliment Pharmacol Ther . 2007;25:723-32.
-
26Wyman JB, Dent J, Heddle R, Dodds WJ, Toouli J, Downton J. Control of belching by the lower oesophageal sphincter. Gut. 1990;31:639-46.
-
27Kessing BF, Bredenoord AJ, Smout AJPM. The pathophysiology, diagnosis and treatment of excessive belching symptoms. Am J Gastroenterol . 2014;10(8).
-
28Fass R, Sifrim D. Management of heartburn not responding to proton pump inhibitors. Gut. 2009;58:295-309.
-
29Hachem C, Shaheen NJ. Diagnosis and Management of Functional Heartburn. Am J Gastroenterol . 2016;111:53-61.
-
30Aziz Q, Fass R, Gyawali CP, Miwa H, Pandolfino JE, Zerbib F. Esophageal disorders. Gastroenterology. 2016;150:1368-79.
-
31Savarino E, Zentilin P, Tutuian R, Pohl D, Casa DD, Frazzoni M, et al. The role of nonacid reflux in NERD: Lessons learned from impedance-pH monitoring in 150 patients off therapy. Am J Gastroenterol . 2008;103:2685-93.
-
32Iwakiri K, Hayashi Y, Kotoyori M, Tanaka Y, Kawakami A, Sakamoto C, Holloway RH. Transient lower esophageal sphincter relaxations (TLESRs) are the major mechanism of gastroesophageal reflux but are not the cause of reflux disease. Dig Dis Sci . 2005;50:1072-7.
-
33Trudgill NJ, Riley SA. Transient lower esophageal sphincter relaxations are no more frequent in patients with gastroesophageal reflux disease than in asymptomatic volunteers. Am J Gastroenterol . 2001;96(Suppl.9):2569-2574.
-
34Kessing BF, Bredenoord AJ, Schijven MP, van der Peet DL, van Berge Henegouwen MI, Smout AJPM. Long-term effects of anti-reflux surgery on the physiology of the esophagogastric junction. Surg Endosc Other Interv Tech. 2015;29:3726-32.
-
35Campos GM, Peters JH, DeMeester TR, Oberg S, Crookes PF, Tan S, et al. Multivariate analysis of factors predicting outcome after laparoscopic Nissen fundoplication. J Gastrointest Surg. 1999;3:292-300.
-
36Mainie I, Tutuian R, Agrawal A, Adams D, Castell DO. Combined multichannel intraluminal impedance-pH monitoring to select patients with persistent gastro-oesophageal reflux for laparoscopic Nissen fundoplication. Br J Surg. 2006;93:1483-7.
-
37Tutuian R, Mainie I, Agrawal A, Adams D, Castell DO. Nonacid reflux in patients with chronic cough on acid-suppressive therapy. Chest. 2006;130:386-91.
-
38Vela MF, Tutuian R, Katz PO, Castell DO. Baclofen decreases acid and non-acid post-prandial gastro-oesophageal reflux measured by combined multichannel intraluminal impedance and pH. Aliment Pharmacol Ther . 2003;17:243-51.
-
39Kline MM, Ewing M, Simpson N, Laine L. The Utility of Intraluminal Impedance in Patients With Gastroesophageal Reflux Disease-Like Symptoms But Normal Endoscopy and 24-Hour pH Testing. Clin Gastroenterol Hepatol . 2008;6:880-85.
-
40Gyawali CP, Kahrilas PJ, Savarino E, Zerbib F, Mion F, Smout AJPM, et al. Modern diagnosis of GERD: the Lyon Consensus. Gut. 2018:67:1351-62.
-
41Hila A, Chowdhury N, Hajar N, Castell DO. Swallow evaluation during multichannel intraluminal impedance and pH: An alternate method to assess esophageal transit. J Clin Gastroenterol. 2011;45:862-6.
-
42Kandulski A, Weigt J, Caro C, Jechorek D, Wex T, Malfertheiner P. Esophageal Intraluminal Baseline Impedance Differentiates Gastroesophageal Reflux Disease From Functional Heartburn. Clin Gastroenterol Hepatol . 2015;13:1075-81.
-
43Kessing BF, Bredenoord AJ, Weijenborg PW, Hemmink GJM, Loots CM, Smout AJPM. Esophageal acid exposure decreases intraluminal baseline impedance levels. Am J Gastroenterol . 2011;106:2093-7.
-
44Vaezi MF, Sifrim D. Assessing Old and New Diagnostic Tests for Gastroesophageal Reflux Disease. Gastroenterology. 2018;154:289-301.
-
45Woodley FW, Fernandez S, Mousa H. Diurnal Variation in the Chemical Clearance of Acid Gastroesophageal Reflux in Infants. Clin Gastroenterol Hepatol . 2007;5:37-43.
-
46Frazzoni M, Savarino E, de Bortoli N, Martinucci I, Furnari M, Frazzoni L, et al. Analyses of the Post-reflux Swallow-induced Peristaltic Wave Index and Nocturnal Baseline Impedance Parameters Increase the Diagnostic Yield of Impedance-pH Monitoring of Patients With Reflux Disease. Clin Gastroenterol Hepatol . 2016;14:40-6.
-
47Frazzoni M, Bertani H, Conigliaro R, Frazzoni L, Losi L, Melotti G. Neoplastic progression in short-segment Barrett’s oesophagus is associated with impairment of chemical clearance, but not inadequate acid suppression by proton pump inhibitor therapy. Aliment Pharmacol Ther . 2014;40:835-42.
-
48Tangaroonsanti A, Jones DR, Lee AS, Vela MF, DeVault KR, Houghton LA. 534 Post-Reflux Swallow-Induced Peristaltic Wave (PSPW) Index, a Measure of Esophageal Chemical Clearance Is a Predicator of Allograph Failure After Lung Transplantation. Gastroenterology. 2016;150:S111-S112. Doi: https://doi.org/10.1016/S0016-5085(16)30480-2.
» https://doi.org/https://doi.org/10.1016/S0016-5085(16)30480-2. -
49Smits MJ, Loots CM, van Wijk MP, Bredenoord AJ, Benninga MA, Smout AJPM. An expert panel-based study on recognition of gastro-esophageal reflux in difficult esophageal pH-impedance tracings. Neurogastroenterol Motil . 2015;27:637-45.
-
Disclosure of funding: no funding received
Publication Dates
-
Publication in this collection
Nov 2018
History
-
Received
23 May 2018 -
Accepted
11 June 2018