Abstracts
INTRODUCTION: Head trauma is an important consequence of child abuse. Specific pathophysiological mechanisms in child abuse are responsible for the ''whiplash shaken-baby syndrome'', which would favour the occurrence of intracranial hemorrhages. CASE REPORT: We report the case of a child who developed epidural hematoma following minor-intensity head trauma. Initial diagnosis of child abuse was made, but subsequent investigation led to the diagnosis of hemophilia A. CONCLUSION: Even though epidural hematoma is not closely associated with child abuse, this aethiology must always be considered when the reported trauma mechanism is out of proportion to the magnitude of the encountered lesions.
hemophilia A; child abuse; epidural hematoma
INTRODUÇÃO: Traumatismo crânio-encefálico é importante conseqüência de abuso infantil. Mecanismos fisiopatológicos específicos do abuso infantil são responsáveis pela ''whiplash shaken-baby syndrome'', o que favoreceria o aparecimento de hemorragias intracranianas. RELATO DE CASO: Relatamos o caso de uma criança que desenvolveu hematoma extradural após trauma de pequena intensidade. Foi feito diagnóstico inicial de abuso infantil, mas investigações subseqüentes levaram ao diagnóstico de hemofilia A. CONCLUSÃO: Embora o hematoma extradural não esteja intimamente relacionado com abuso infantil, esta etiologia deve ser sempre considerada quando o mecanismo de trauma relatado estiver fora de proporção com as lesões encontradas.
hemofilia A; abuso infantil; hematoma extradural
Hemophilia and child abuse as possible causes of epidural hematoma: case report
Hemofilia e abuso infantil como possíveis causas de hematoma extradural: relato de caso
Fernando Campos Gomes PintoI; Fabrizio Frutos PorroI; Liliana SuganumaII; Ricardo Bragança de Vasconcellos FontesII; Almir Ferreira de AndradeIII; Raul Marino JrIV
Neurosurgery Division, Neurology and Neurosurgery Department, University of São Paulo Medical School, São Paulo SP, Brazil (USP)
IM.D., Resident, USP
IIM.D., Liga de Neurocirurgia, USP
IIIM.D., Ph.D., Head of the Neurosurgery Emergency Section, USP
IVM.D., Ph.D., Head of the Neurosurgery Division, USP
ABSTRACT
INTRODUCTION: Head trauma is an important consequence of child abuse. Specific pathophysiological mechanisms in child abuse are responsible for the ''whiplash shaken-baby syndrome'', which would favour the occurrence of intracranial hemorrhages.
CASE REPORT: We report the case of a child who developed epidural hematoma following minor-intensity head trauma. Initial diagnosis of child abuse was made, but subsequent investigation led to the diagnosis of hemophilia A.
CONCLUSION: Even though epidural hematoma is not closely associated with child abuse, this aethiology must always be considered when the reported trauma mechanism is out of proportion to the magnitude of the encountered lesions.
Key words: hemophilia A, child abuse, epidural hematoma.
RESUMO
INTRODUÇÃO: Traumatismo crânio-encefálico é importante conseqüência de abuso infantil. Mecanismos fisiopatológicos específicos do abuso infantil são responsáveis pela ''whiplash shaken-baby syndrome'', o que favoreceria o aparecimento de hemorragias intracranianas.
RELATO DE CASO: Relatamos o caso de uma criança que desenvolveu hematoma extradural após trauma de pequena intensidade. Foi feito diagnóstico inicial de abuso infantil, mas investigações subseqüentes levaram ao diagnóstico de hemofilia A.
CONCLUSÃO: Embora o hematoma extradural não esteja intimamente relacionado com abuso infantil, esta etiologia deve ser sempre considerada quando o mecanismo de trauma relatado estiver fora de proporção com as lesões encontradas.
Palavras-chave: hemofilia A, abuso infantil, hematoma extradural.
Head trauma is the most frequent cause of morbidity and mortality in children who have suffered abuse. Billmire and Myers1 report that, excluding uncomplicated skull fractures, 95% of serious intracranial injuries and 64% of all skull injuries in children under 1 year of age are consequences of child abuse. Besides that, 80% of all deaths due to head trauma in children under 2 years are provoked by the same trauma mechanism2. The diagnosis of child abuse must be remebered when evaluating head injuries in children under 2 years of age, especially when the reported trauma mechanism is out of proportion to the magnitude of signs encountered during physical examination or when there are evidences of violence in other regions of the body, such as multiple fractures, contusions and/or ecchymosis. Caffey and other authors3-6 propose a specific pathophysiological mechanism for head injury due to child abuse, named 'whiplash shaken-baby syndrome'. According to this theory, infants possess certain predisposing factors for head injury, such as relatively bigger skull size and weight, cervical musculature flaccidity, nervous system vasculature fragility, weaker skull and vulnerability of the bridging veins due to larger subarachnoideal spaces. The combination of these predisposing factors, when the child is shaken while being held by the limbs or trunk, would favour the occurrence of subarachnoideal, subdural and retinal hemorrhages, diffuse axonal injury and cerebral edema. This pathophysiological mechanism should be suspected especially in the absence of evidences of external trauma. On the other hand, the most serious forms of this syndrome are related to direct impact as the precipitating factor of sudden deceleration7. The symptoms of shaken baby syndrome are non-specific and comprise irritability, lethargy, vomiting, nausea, fever and respiratory alterations, which render clinical diagnosis difficult8.
We report the case of an infant who developed intracranial hemorrhage (epidural hematoma) following minor-intensity head trauma. Initial diagnosis was made of child abuse. However, subsequent clinical investigation revealed the diagnosis of classic hemophilia. The differential diagnosis between these two clinical entities is discussed.
CASE
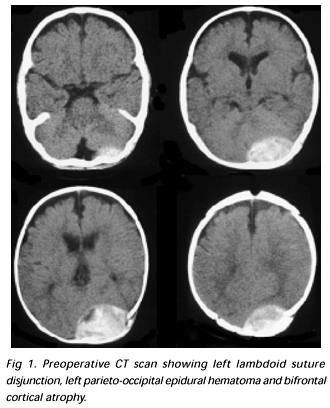
A, white, male, seven months old infant, born and resident in the city of São Paulo, was admitted to the Neurosurgery Emergency Section of the Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo (HC-FMUSP) on December 31, 2000. According to his mother, a divorced housemaid, his aunt looked after him during the day while she was on her job. However, during one of these periods two weeks before admission, the child had hit his head against the wall after falling from his cradle. A large subgaleal hematoma progressively formed on the left parieto-occipital region. The child subsequently became somnolent one day before admission and had two episodes of vomiting. Physical examination revealed a hipoactive and reactive child, spontaneously moving all four limbs, normotense bregmatic fontanelle, large subgaleal hematoma on the left parieto-occipital region and disjunction of the left lambdoid suture. Cranial perimeter was considered normal at 46 cm. Computed tomography (CT) scan of the skull confirmed the diagnosis of disjunction of the left lambdoid suture, showed a left parieto-occipital epidural hematoma and suggested bifrontal cortical atrophy (Fig 1). The child underwent a left parieto-occipital craniotomy. During surgery, a left occipital fracture was found and a large epidural hematoma drained. Hemostasis of diffuse bleeding points was performed and no other incidents occurred during the surgery. Postoperative control CT scans revealed good surgical results and complete removal of the hematoma (Fig 2). Due to the confusing clinical story reported by the mother, the diagnosis of child abuse was suspected and the Hospital das Clínicas Social Services Department was notified during the immediate postoperative period. Radiographs of long bones were performed but did not reveal any signs of fractures. Ophthalmological evaluation was normal. Abnormal blood laboratory findings were hemoglobin 7.6 g/dL, hematocrit 24.1% and a platelet count 513,000. The child was discharged on the eighth postoperative day after a court order was obtained. Physical examination revealed an active and reactive child, normotense bregmatic fontanelle and no other abnormalities.
On January 14, 2001 the patient was brought once again to the HC-FMUSP. He had developed a dehiscence of the surgical wound because of a large subgaleal hematoma. He underwent a new operation. After this new procedure, while the child was still on the wards, another subgaleal hematoma formed at the same site. Hematological investigation was performed and coagulation laboratory results revealed a partial activated thromboplastin time of 63.7 seconds (R=2.55), and factor VIII activity was measured at 2%. The diagnosis of classical hemophilia A was thus established and child abuse excluded.
DISCUSSION
Several studies dissociate epidural hematoma from child abuse, but relate this pathophysiological mechanism to interhemispheric subdural hematoma, subarachnoideal hemorrhage, bilateral chronic subdural hematoma and retinian hemorrhage. This last finding is pathognomonic when child abuse is suspected9. Epidural hematoma in the pediatric population is related to direct head impact such as accidental falls. In these cases, the impact generates linear acceleration, leading to the laceration of meningeal blood vessels located in the virtual space between the dura mater and the skull due to excessive acute traction. Eventually, skull fractures and diploe or venous sinuses bleedings may be the cause of epidural hematomas. Therefore the degree of suspicion of child abuse must be much higher in cases of subdural hematomas, despite the fact that subdural hematomas can also form secondary to accidental head trauma10, 11.
Shugerman et al. report that only 6% of their 93 patients between 0 and 3 years of age that suffered child abuse presented with epidural hematoma. On the other hand, 47% of these patients possessed subdural hematoma. Even though our case included an epidural hematoma and the child did not present fractures or other hemorrhages, the diagnosis of child abuse was suspected because of the recurrence of intracranial hemorrhage and the absence of any compatible trauma mechanism related during clinical interview with the mother, which is a common characteristic of child abuse cases10.
Especially in cases which the physician suspects of child abuse with no external evidences of trauma, radiological findings may be valuable for the diagnosis. Radiographs may reveal multiple fractures in typical sites such as ribs and the metaphyses of long bones. These fractures may also show different healing phases. CT and magnetic resonance imaging (MRI) scans of the the brain may reveal contusions, subarachnoideal hemorrhage, cerebral edema, infarct areas or signs of previous brain lesions, such as cortical atrophy, ex vacuo hydrocephalus and bilateral chronic subdural hematoma11-13.
The incongruence between clinical history and physical findings in child abuse cases defies even the most skilled clinicians. This case reminds us that even though very frequent in our society, child abuse is not the sole cause of incongruence between history and physical exam. Neurosurgeons should thus always bear in mind the differential diagnosis of this clinical entity.
Received 17 January 2003, received in final form 23 May 2003. Accepted 23 June 2003
Dr. Ricardo B. V. Fontes - Rua Jandiro Joaquim Pereira 389 - 05658-000 São Paulo SP - Brasil. E-mail: rbvfontes@yahoo.com.br
- 1. Billmire ME, Myers PA. Serious head injury in infants: accident or abuse? Pediatrics 1985;75:340-342.
- 2. Bruce DA, Zimmerman RA. Shaken impact syndrome. Pediatr Ann 1989;18482-494.
- 3. Caffey J. Multiple fractures in the long bones of infants suffering from subdural hematomas. AJR 1946;56:163-173.
- 4. Caffey J. On the theory and practice of shaking infants: its potential residual effects of permanent brain damage and mental retardation. Am J Dis Child 1972;124:161-169.
- 5. Caffey J. The whiplash shaken infant syndrome: manual shaking by the extremities with whiplash-induced intracranial and intraocular bleedings, linked with residual permanent brain damage and mental retardation. Pediatrics 1974;54:396-403.
- 6. Guthkelch NA. Infantile subdural hematoma and its relationship to whiplash injury. Br Med J 1971;2:430-431.
- 7. Duhaime AC, Genarelli TA, Thibault LE, Bruce DA, Margulies SS, Wiser R. The shaken baby syndrome: a clinical, pathological and biomechanical study. J Neurosurg 1987;66:409-415.
- 8. Comittee on Child Abuse and Neglect. Shaken baby syndrome: inflicted cerebral trauma. Del Med J 1997;69:365-370.
- 9. Eisemberg AB. Retinal hemorrhage in the battered child. Childs Brain 1979;5:40-44.
- 10. Shugerman RP, Paez A, Grossman DC, Feldman KW, Grady S. Epidural hemorrhage: is it abuse? Pediatrics 1996;97:664-668.
- 11. Ewing-Cobbs L, Kramer L, Prasad M, et al. Neuroimaging, physical and developmental findings after inflicted and noninflicted traumatic brain injury in young children. Pediatrics 1998;102:300-307.
- 12. Bach KP, Schouten-van Meeteren AY, Smit LM, Veenhuizen L, Gemke RJ. Intracranial hemorrhages in infants: child abuse or a congenital coagulation disorder? Ned Tijdschr Geneeskd 2001;145:809-813.
- 13. Bray GL, Luban NLC. Hemophilia presenting with intracranial hemorrhage: an approach to the infant with intracranial bleeding and coagulopathy. Am J Dis Child 1987;141:1215-1217.
Publication Dates
-
Publication in this collection
06 Jan 2004 -
Date of issue
Dec 2003
History
-
Received
17 Jan 2003 -
Reviewed
23 May 2003 -
Accepted
23 June 2003