Abstracts
OBJECTIVE: To evaluate the dose distribution in different situations of high dose-rate endobronchial brachytherapy, focusing especially on high-dose volumes, and try to identify better or worse situations in terms of dose distribution to aid as guidance in the clinical practice. MATERIALS AND METHODS: Theoretical study simulating high dose-rate endobronchial brachytherapy utilizing two catheters, varying the loading extent, angle between the catheters, prescription depth, and source step. With a prescription dose of 7.5 Gy, the volumes involved by the 100%, 150% and 200% isodoses (V100, V150 and V200, respectively) and V150/V100 and V200/V100 ratios were calculated. RESULTS: There was a volume enhancement with larger loaded lengths, increase in prescription depth and angles, with a tendency towards a proportionally smaller increase with larger angulations. In general, the V150/V100 and V200/V100 ratios were homogeneous, respectively around 0.50 and 0.30. CONCLUSION: Overall, the dose distribution in the standard situation was appropriate. No specific parameter that could be related to a higher toxicity was identified. The authors recommend a swift evaluation of the treatment quality through the analysis of the V150/V100 and V200/V100 ratios.
Radiotherapy; Endobronchial brachytherapy; Dosimetry
OBJETIVO: Avaliar a distribuição de dose em diferentes situações de braquiterapia endobrônquica de alta taxa de dose, com foco principalmente nos volumes de altas doses, e tentar definir situações de melhor ou pior distribuição de dose que possam servir de guia na prática clínica. MATERIAIS E MÉTODOS: Estudo teórico, simulando braquiterapia endobrônquica de alta taxa de dose utilizando dois cateteres, com variação da extensão de carregamento, angulação entre os cateteres, profundidade de cálculo e o intervalo entre as paradas da fonte. Com prescrição de 7,5 Gy, foram calculados os volumes englobados pelas isodoses correspondentes a 100%, 150% e 200% da dose prescrita (V100, V150 e V200, respectivamente) e as razões V150/V100 e V200/V100. RESULTADOS: Os volumes aumentaram com o aumento da extensão de carregamento dos cateteres, profundidade de cálculo e angulação, com tendência a um aumento proporcionalmente menor para angulações maiores. As relações V150/V100 e V200/V100 foram, em geral, homogêneas, ao redor de 0,50 e 0,30, respectivamente. CONCLUSÃO: A distribuição de dose na situação considerada padrão é em geral adequada. Nenhum parâmetro específico que pudesse ser relacionado à maior toxicidade foi identificado. Recomendamos uma avaliação rápida da qualidade do implante por meio da análise das relações V150/V100 e V200/V100.
Radioterapia; Braquiterapia endobrônquica; Dosimetria
ORIGINAL ARTICLE
High dose-rate endobronchial brachytherapy: a dosimetric sudy*
Regina Maria Godoy LopesI; Laura Natal RodriguesII; Heloisa de Andrade CarvalhoIII
IMaster of Sciences, Physicist at Unit of Radiotherapy - Hospital Santa Rita, São Paulo, SP, Brazil
IIPhD of Physics, Physicist at Unit of Radiotherapy - Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (HC-FMUSP) and Instituto de Pesquisas Energéticas e Nucleares da Universidade de São Paulo (IPEN-USP), São Paulo, SP, Brazil
IIIPhD of Medicine, Physician Assistant at Unit of Radiotherapy - Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (HC-FMUSP), São Paulo, SP, Brazil.
Mailing address
ABSTRACT
OBJECTIVE: To evaluate the dose distribution in different situations of high dose-rate endobronchial brachytherapy, focusing especially on high-dose volumes, and try to identify better or worse situations in terms of dose distribution to aid as guidance in the clinical practice.
MATERIALS AND METHODS: Theoretical study simulating high dose-rate endobronchial brachytherapy utilizing two catheters, varying the loading extent, angle between the catheters, prescription depth, and source step. With a prescription dose of 7.5 Gy, the volumes involved by the 100%, 150% and 200% isodoses (V100, V150 and V200, respectively) and V150/V100 and V200/V100 ratios were calculated.
RESULTS: There was a volume enhancement with larger loaded lengths, increase in prescription depth and angles, with a tendency towards a proportionally smaller increase with larger angulations. In general, the V150/V100 and V200/V100 ratios were homogeneous, respectively around 0.50 and 0.30.
CONCLUSION: Overall, the dose distribution in the standard situation was appropriate. No specific parameter that could be related to a higher toxicity was identified. The authors recommend a swift evaluation of the treatment quality through the analysis of the V150/V100 and V200/V100 ratios.
Keywords: Radiotherapy; Endobronchial brachytherapy; Dosimetry.
INTRODUCTION
The appropriate assessment of dose distribution in general radiotherapy is of paramount importance for the success of the treatment with a minimum of complications. In brachytherapy in which high doses are administered to restricted volumes, this aspect has an even greater importance. Currently, the three dimensional evaluation, considering the irradiated volumes and their correlations, plays an essential role in endobronchial high-dose rate brachytherapy (EHDRB), supporting the most appropriate possible dose distribution. However, in spite of the fact that the calculations do consider three dimensions, in most of times the planning is based on orthogonal or semi-orthogonal plain radiographs, without radiological image of the lesion and respective anatomical correlations.
In endobronchial brachytherapy, the catheters are placed in positions that produce distinctive geometries at each treatment. The anatomy of the region causes the catheters to become bent (there is an unequal dose distribution in relation to concave and convex surfaces)(1), unparallel, with non perpendicular crossings and not centralized in the bronchial lumen. Additionally, characteristics such as the variation in the extent and diameter of the different bronchial segments, the parallelism of the bronchial tree with its vascularization, the contact of the large vessels at the base of the heart with the main bronchial tree, among others, must be evaluated in order to minimize the risk for complications, particularly fatal hemorrhage.
There are few published studies defining dosimetric parameters of quality for endoluminal brachytherapy, and such studies only consider treatments with a single catheter, in a straight line(2,3). However, in cases requiring crossing or bending catheters, such studies, despite their value as a guidance, are not directly applicable in the evaluation of the quality of this treatment modality.
Based on such studies, the authors have opted to study the implants quality by analysing some volumetric parameters specific for clinical EHDRB dosimetry and maybe, identify situations with higher risk for complications. In a treatment whose main objective is the improvement of patients' quality of life, the technical precautions and patient selection must result in benefits that are greater than the risk to which the patients will be exposed.
The purpose of the present study was to evaluate dose distribution in different EHDRB situations, with emphasis on high-dose volumes, trying to define situations of better and worse dose distribution that may be adopted in the clinical practice.
MATERIALS AND METHODS
This is a theoretical study where simulations of EHDRB plannings were performed with two catheters, with variation of loaded extent, angulation between catheters, calculation depth and source step.
Treatments with two catheters were simulated, utilizing 20°, 30°, 40°, 45°, 60°, 80°, 90°, 100°, 120°, 140°, 160° e 180° angulations (this last one also corresponding to a single catheter). Each one of the catheters was loaded in lenghts ranging from 2 to 10 cm (with 1 cm intervals). The calculations were made for depths of 5 mm, 7 mm and 10 mm from the source axis. Routinely, the source step is not changed in the clinical practice. However an option was made to also evaluate the influence of the source step variation on dosimetry for each analyzed situation, simulating options of not loading at some source dwell positions. The steps utilized were 5 mm, 10 mm, 15 mm and 20 mm. A dose of 750 cGy was prescribed for the volume covered by the 100% isodose (V100).
Volumes covered by the isodoses corresponding to 100%, 150% and 200% of the prescribed dose (V100, V150 and V200, respectively) were calculated in all possible combinations, by means of the dose-volume histograms. The V150/V100 ratio was also calculated, as recommended by Saw et al.(3), as well as the V200/V100 ratio.
The ABACUS (Gammamed-12I) planning system including an option for endobronchial treatment calculation was utilized. This method is based on a linear or quadratic interpolation for optimization of the treatment by means of equal source dwell times (without optimization), geometric distribution or iteractive correction. The linear interpolation with iteractive correction was selected.
The V150/V100 ratio < 0.50(3) was considered as the ideal theoretical situation. However, a value of up to 5% above this ratio was also accepted as a good quality implant, due to variations observed in the clinical practice. (Note: in the absence of a more appropriate term to define endo-luminal brachytherapy, the word "implant" will be utilized herein after to define the procedures).
RESULTS
The combination among volumes calculation variations resulted in 108 data tables with the respective charts. The option was made, therefore, to describe the main results of each studied parameter, illustrating the most frequent situations in the clinical practice, with steps of 5 mm and calculation depth at 10 mm from the source axis.
Variation of catheter loading length and angulation
The volumes presented a linear behavior in relation to the catheters loading length, with a tendency to a proportionally smaller increase for larger angles (Figure 1) particularly from 8 cm loadings. With extreme catheters angulation (20° or close to or equal to 180°), the dose distribution is similar to that of a single catheter, as expected, with some advantages with smaller angles, in which the high dose volumes are distributed between both catheters. Figure 2 shows the behavior of the V150/V100 and V200/V100 ratios in this situation, considered as standard. It is possible to observe that the V150/V100 ratio is in general homogeneous, however, with smaller angulations, it tends to increase. From the 5 cm loading, the homogeneity increases. On the other hand, the V200/V100 ratio that is also homogeneous, tends to stabilize with 6 cm loadings or more, and decreases with angles < 90° as the loading lenght increases.
Variation of the calculation depth
Figures 3 and 4 show the volumes behavior when the 5 mm standard step is maintained for a treatment with a fixed 5 cm loading lenght, and the prescription depth varying for the different studied angulations. Likewise, in Figure 3 one can observe that all volumes increase as the angles increase and tend to remain stable starting at 90°. For a same situation, when the calculation depth decreases, both V100 and the high-dose volume obviously also decrease, at a rate of approximately 50% at every 2 or 3 mm of variation. For example, the V100 of a calculation at 5 mm is similar to V200 for the same calculation at a depth of 10 mm. On Figure 4, one can notice that the prescription at 10 mm presents a homogeneous behavior of the V150/V100 and V200/V100 ratios, independently of the catheters angulation. As the depth is changed, prescriptions at 5 mm present the lowest values; however, calculations at a depth of 7 mm present the highest values for V150/V100, with angles > 60°, decreasing when the catheter becomes a straight line (180°). Paradoxically, both the 7 mm and 5 mm calculation depths have V200/V100 values lower than at the depth of 10 mm.
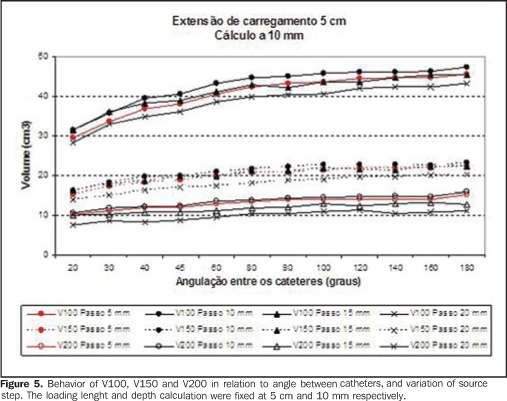
Variation of the source step
Figures 5 and 6 show what happens with the volumes when the source step is varied. The increase in source step decreases the high-dose volumes, particularly V200, as well as the step equivalent to twice the prescription depth (for example, the prescription at 10 mm presented smaller V150/V100 with a 20 mm step). However, the treatment volume (V100) decreases with the step increase, mainly due to the volume decrease at the implants extremities.
For the standard situation, with a 5 mm step and 10 mm depth calculation, the V150/V100 ratio presented the mean value of 49.2% (45.6% to 54.7%), but ranged from 28.4% to 60.8% considering all the analyzed situations. It was possible to observe that angles > 60°, loading lengths < 4 cm, and calculation depth at 7 mm presented the highest V150/V100 (above 0.52) values. The V200/V100 ratio presented a mean value of 23.9% (19.6 to 36.1%) for the standard situation and presented a global variation from 16% to 40%, being greater for the smaller lenghts. Table 1 presents the mean V150/V100 and V200/V100 values for the different calculation depths that were analyzed.
DISCUSSION
According to the brachytherapy optimization rules, the 100% isodose must be as regular and homogeneous as possible, minimizing the high-dose volumes(4). The American Brachytherapy Society(5) recommends that in endobronchial brachytherapy, the dose at the depth of 10 mm be reported. However, innumerable treatment possibilities were analysed in order to evaluate the variations of dose distribution. Even situations considered as unusual, such as the case of source step variation, were studied in order to evaluate advantages and shortcomings of the different combinations.
The main accomplishment of such an exercise in dosimetry was observing that, the predefined standards for source step, dwell and calculation depth, presented a satisfactory dose distribution independently of the calculation depth and catheters angulation. In other words, even with a geometry not defined by the optimization rules, such standards can be applied to endobronchial brachytherapy with regards to dose distribution.
The analysis of treatment volumes was intended to provide a three-dimensional view of the dose distribution, besides allowing the evaluation of implants with non-classical geometries. The V150/V100 ratio concept introduced by Saw et al.(3) proved to be useful in the evaluation of the volume receiving at least 50% more than the dose (V150), and in general that volume was around 50% of the treatment volume (V100). Furthermore, the volume that receives twice the prescription dose (V200) and its relation with the treatment volume (V200/V100) were also evaluated. Such ratio presented values ranging between 25% and 30%, a useful information in the evaluation of high-dose volumes. No references to this type of analysis were found in literature. The authors believe that, after the treatment calculation, the analysis of the high-dose volumes and their relation with V100 is valuable in the rapid assessment of the implant quality/homogeneity, providing more safety to the treatment.
The treatment volume can be, among others, a risk factor for complications(6). A general conclusion in the present study is that smaller implants present a more "concentrated" dose distribution, given the characteristics of brachytherapy. In spite of the fact that the high-dose volumes are proportionally greater, there is a compensation by the smallest treatment volume (V100) and, consequently, smallest absolute volumes in general.
The angle between the catheters had an influence on the irradiated volumes. The lower the angle, the more concentrated the volumes tend to be, as if there were only one catheter. With the catheters in close proximity, the dwell times may be eliminated or decreased in some points, generating greater homogeneity in the high-dose region. Such fact may be utilized as a tool to support the treatment optimization. The dose distribution between two catheters instead of a single one, producing the same treatment volume, for example, decreases the dose on the surface of each catheter, which may preserve the mucosa in contact with them. The greater the angle between the catheters, the more the isodose distribution approaches that of a straight catheter, as described by Ezzel(7).
A brief comment with regards to alterations in the source step deserves to be made. The lowest ratios between high dose volumes and V100 were observed with the 2 cm step and calculation at a depth of 1 cm, representing a better dose distribution considering the hot spots. Although in practice the source step in not increased further than 5 mm, it is possible not to load certain positions, leading to dwell intervals different from step length. However, it was possible to observe that such a strategy, in spite of theoretically presenting advantages as compared with high-dose volumes, it leads to a reduction of V100, which might cause an underdose of the tumor. As the standard situation is homogeneous, no advantages were identified in changing the source step, or in intentionally excluding some dwell positions.
The concern in relation to high-dose volumes is mainly due to the possibility of direct contact of the catheter with the normal bronchial mucosa. A Dutch group has evaluated the doses in the healthy bronchial mucosa utilizing computed tomography (CT)(8,9). The authors have suggested the use of a dose-wall histogram and a dose-surface histogram, considering a 3 mm-wall thickness. Some aspects have also been takent into consideration: the method is limited, as only the trachea and the main bronchi are visible at CT and likely to be outlined in the planning system; most of the catheters are positioned on the medial or posterior wall of the bronchus at the level of the carina; the prescription can be made in accordance with the bronchus diameter; in most of the cases, prescriptions at 10 mm depth cover the whole tumor volume, but may cause an overdose in the mucosa; and, finally, the increase in total procedure time does not justify its use in palliative cases. They suggest the use of catheters with centering devices, and that a prescription at a depth of 2 mm from the bronchial wall may be a good alternative. They also recommend the utilization of the method, particularly for curative cases, because of the higher cost and time spent in the procedure. Also, it is important to highlight that only treatment situations with a single catheter were analyzed, because of the practical difficulties of evaluating treatments with two catheters or two targets.
In the present study, treatments with one or two catheters were simulated with dose calculations at depths compatible with the clinical practice. The loading lenghts, angles between catheters and source step were varied. Generally, the prescriptions at 5 mm depth presented the best dose distribution in all situations in agreement with the Dutch study. However there is the risk of underdosing of the target volume. Generally this is the prescribed depth for the treatment of segmental or subsegmental bronchi, attempting to adjust the dose to the bronchus diameter.
Concerning the target volume, the same authors(8,9) have observed that the best dose distribution was obtained with prescriptions at the depth of 10 mm. Therefore, in this situation, the high-dose volumes evaluation is mandatory. In the present study, such situation presented a good dose distribution in all instances, considering the analyzed volumes.
Ezzel(10) has attempted to establish an algorithm in order to predefine the source dwell times in treatments with two catheters. Two baseline geometries were considered, "Y" and "V". In the "V" geometry, the catheters were not loaded in their proximal segments. A theoretical study was developed, with the angle between catheters ranging from 30° to 90°, and the separation between their parallel portions ranged from 0.3 to 1.5 mm ("Y" geometry). "Weights" were established for the source dwell times from the proximal portion, on to the angle to the distal portion. A table was built with these weights, which could eventually facilitate the treatment calculation. Comparing the calculations obtained with the use of such table with actual situations, the author observed a variation of plus or minus 5% of the prescribed dose at a 10 mm depth. Such variation corresponds to a difference of 1 mm in the prescribed depth. It is important to note that, when the author fixed the distance between the catheters in their "parallel" portion, he has not considered the variations of such distance along the lenght and positioning of the catheters that is minimized next to their crossing point.
In the present study, the "Y" geometry was not evaluated; however there were angle variations above 90°, simulating single curved catheters, or specific treatments such as the irradiation of the upper and lower lobe bronchi. Also, the symmetrical loading of both catheters was the standard procedure. In the clinical practice, this symmetry is not always necessary, and an asymmetrical loading may constitute an alternative to change the treatment volumes.
Finally, it should be pointed out that the analysis of dosimetric parameters must always be performed together with the clinical evaluation. Factors such as volume, tumor site and previous treatments among others, must be considered in the treatment indication and analysis of the risk for complication.
CONCLUSIONS
With this dosimetric exercise, it was possible to observe that the dose distribution in the situation considered as standard is in general appropriate. No specific parameter possibly related to a higher toxicity could be identified.
Shoter lenghts with smaller angles lead to a higher concentration of high-dose volumes, compensated by the smaller treatment volume (V100). The individual evaluation of each treatment, however, is critical because of the high variations observed, particularly in the ratios between high-dose volumes and V100.
With prescriptions at 5mm, the nominal dose can eventually be higher, in the case of bronchi with a larger caliber. Prescriptions at 7 mm depths, with loading lengths < 6 cm and angles > 60° must be individually analyzed.
Therefore, the standard treatment is recommended, with special attention to a catheter angulation around 90°. In sites where overdosing should be avoided (proximity with large vessels, for example), a better dose distribution can be obtained by using two catheters, as demonstrated in situations with smaller angles. The elimination or reduction of margins in relation to the catheter loading versus lesion extent can be evaluated to reduce V100.
Also, a rapid evaluation of the implant quality by means of the analysis of the V150/V100 ratio (which should be maintained at approximately 50%) and the V200/V100 ratio (around 25% to 30%) is suggested in order to consider eventual changes in the calculation.
REFERENCES
- 1. Carvalho HA, Aisen S, Pedreira Júnior WL, et al. Braquiterapia endobrônquica de alta taxa de dose: técnica de tratamento. Rev Imagem. 1998;20: 151-6.
- 2. Marinello G, Pierquin B, Grimard L, et al. Dosimetry of intraluminal brachytherapy. Radiother Oncol. 1992;23:213-6.
- 3. Saw CB, Korb LJ, Pawlicki T, et al. Dose volume assessment of high dose rate 192Ir endobronchial implants. Int J Radiat Oncol Biol Phys. 1996;34: 917-22.
- 4. Williamson JF, Brenner DJ. Physics and biology of brachytherapy. In: Perez CA, Brady LW, Halperin EC, et al., editors. Principles and practice of radiation oncology. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2004. p. 472-537.
- 5. Nag S, Abitbol AA, Anderson LL, et al. Consensus guidelines for high dose rate remote brachytherapy in cervical, endometrial, and endobronchial tumors. Clinical Research Committee, American Endocurietherapy Society. Int J Radiat Oncol Biol Phys. 1993;27:1241-4.
- 6. Carvalho HA, Gonçalves SLV, Pedreira W Jr, et al. Irradiated volume and the risk of fatal hemoptysis in patients submitted to high dose-rate endobronchial brachytherapy. Lung Cancer. 2007;55:319-27.
- 7. Ezzell GA. Limitations of the straight-line assumption for endobronchial HDR brachytherapy treatments. Med Phys. 2000;27:151-3.
- 8. Senan S, Lagerwaard FJ, de Pan C, et al. A CT-assisted method of dosimetry in brachytherapy of lung cancer. Rotterdam Oncological Thoracic Study Group. Radiother Oncol. 2000;55:75-80.
- 9. Lagerwaard FJ, Murrer LH, de Pan C, et al. Mucosal dose prescription in endobronchial brachytherapy: a study based on CT-dosimetry. Int J Radiat Oncol Biol Phys. 2000;46:1051-9.
- 10. Ezzell GA. A manual algorithm for computing dwell times for two-catheter endobronchial treatments using HDR brachytherapy. Med Phys. 2000;27:1030-3.
Publication Dates
-
Publication in this collection
09 Mar 2010 -
Date of issue
Feb 2010
History
-
Received
25 July 2009 -
Accepted
30 Nov 2009