Abstract
Os autores analisaram 13 doentes com ferimentos hepático transfixante tratados com a colocação de balão hidrostático no trajeto do ferimento. Cinco doentes apresentavam ferimento abdominal exclusivo, enquanto 8 eram toraco-abdominais. Em todos os casos houve acometimento do lobo direito e em três o acometimento foi bilobar. O tempo médio de permanência do balão insuflado foi de 9 dias. Dois doentes necessitavam reoperação para a retirada do balão em virtude de existência de aderências que impediam sua mobilização. Não foram observados casos de sangramento após a retirada do balão. A permanência hospitalar variou de 5 a 36 dias. São discutidas as indicações e as vantagens da colocação desse tipo de dispositivo em doentes com ferimentos hepáticos profundos, transfixantes e com sangramento abundante.
Trauma; Abdominal trauma; hepatic trauma; intrahepatic Balloon
ORIGINAL ARTICLE
Treatment of transfixing hepatic lesions with a hydrostatic balloon
Sérgio San Gregorio Fávero; Paulo Roberto Corsi; Raul Sérgio Martins Coimbra; Samir Rasslan
Emergency Service, Department of Surgery, Faculty of Medical Sciences of "Santa Casa de São Paulo" - Brazil
Address for correspondence Address for correspondence: Dr. Sérgio San Gregorio Fávero Rua Coelho Lisboa, 41 - São Paulo - SP - Brasil CEP 03323-040
Uniterms: Trauma, Abdominal trauma, hepatic trauma, intrahepatic Balloon.
RESUMO
Os autores analisaram 13 doentes com ferimentos hepático transfixante tratados com a colocação de balão hidrostático no trajeto do ferimento. Cinco doentes apresentavam ferimento abdominal exclusivo, enquanto 8 eram toraco-abdominais. Em todos os casos houve acometimento do lobo direito e em três o acometimento foi bilobar.
O tempo médio de permanência do balão insuflado foi de 9 dias. Dois doentes necessitavam reoperação para a retirada do balão em virtude de existência de aderências que impediam sua mobilização. Não foram observados casos de sangramento após a retirada do balão. A permanência hospitalar variou de 5 a 36 dias.
São discutidas as indicações e as vantagens da colocação desse tipo de dispositivo em doentes com ferimentos hepáticos profundos, transfixantes e com sangramento abundante.
INTRODUCTION
Because of its size, the liver is particularly vulnerable to damage in contusions and penetrating wounds of the abdomen. The incidence of liver damage ranges from 15 to 45% in abdominal contusions, but rises to 30 to 40% after penetrating firearm or knife wounds. In essence, any projectile or any other perforating instrument that penetrates the abdomen can cause liver damage (7).
Because the liver is a well irrigated parenchymatous organ, the challenge posed by complex hepatic lesions is the control of bleeding. Among these types of lesions are transfixing hepatic wounds caused by bullets, wich are often highly difficult to resolve surgically (16,17).
In view of the impossibility of suturing and control-ling hemorrhage in deep lesions of the liver parenchyma, the surgeon is forced to use more agressive types of treatment. However, a simpler therapeutic action which may be quite effective is to produce tamponade of the path of the wound with a balloon or tube in order to stop bleeding by compression. This procedure was created in 1906 by Schroeder (apud 17), who introduced and insufflated a rubber balloon along the path of the wound, controlling hemorrhage after a frustated attempt to do so with sponges.
This maneuver was not disseminated and was eventually forgotten until recently when Branco et al. used it successfully in nine patients with complex penetrating wounds (2). Because of its simplicity and effectiveness, the procedure deserves to be disseminated, even though we are aware that various services in Brazil already use it, but with no reports on their results.
Thus, the objective of the present report was to present a small series of patients with transfixing wounds of the liver treated by tamponade with a hydrostatic balloon.
CASES
The study was conducted on 13 patients (12 males and 1 female) with transfixing wounds of the liver admitted to the Emergency Service of the Department of Surgery, Faculty of Medical Sciences of "Santa Casa de São Paulo", from June 1987 to April 1992. Patient age ranged from 17 to 43 years, with a mean of 28.6 years. All had been wounded by firearm bullets. Thoraco-abdominal wounds were present in eight patients, and only abdominal wounds were present in the remaining five. Four patients were hemodynamically unstable upon admission, with a systolic pressure of 90 mmHg or less. The trauma score ranged from 11 to 16 (Table 1).
The right lobe was damaged in all cases. In one patient there was also involvement of the caudate lobe, and in two others the left lobe was also involved.
As to associated lesions, involvement of the right kidney was present in five patients, and lesion of the inferior vena cava occurred in only one.
Lesions of other organs were present and are listed in Table 2 according to the Penetrating Abdominal Trauma Index (PATI).
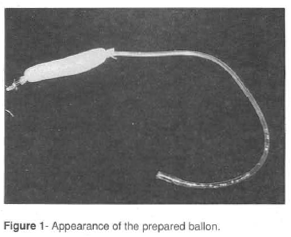
The option to introduce a balloon was chosen in the presence of a transfixing wound of the liver of difficult approach and with active bleeding. The balloon consists of two drains arranged coaxially, an internal tubular one made of plastic (no 14 or 16 Levine tube), and an external, laminar one of the Penrose type. The laminar drain is firmly tied to the tubular one at the ends and the latter is occluded with a ligature at its distal end (Fig. 1).
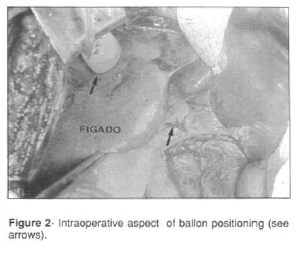
The tubular drain should contain three to four orifices so as to permit the introduction of fluid inside the laminar drain, transforming it into a balloon. The balloon should extend 4 to 6 cm beyond the path of the wound. The capacity of the balloon is verified with contrast fluid, so as to maintain it distened. When it is insufflated, with its ends located aproximately 2 to 3 cm outside the path at both ends of the wound, it should take on the shape of dumbells perfectly anchored to the liver parenchyma (Figs. 2 and 3).
After the occurrence of hemostasis was verified and the associated visceral lesions were corrected, the cavity was drained with a tubular-laminar drain exteriorized through the right flank, with the balloon coming out through a counter-opening in an incision separate from that of the abdominal drain.
The common hepatic artery was ligated in one case at the beginning of surgery and the balloon was introduced because of persistent bleeding. No additional hemostasis procedures were used in the remaining patients.The mean volume of crystalloid solution infused intraoperatively was 4.15 liters, and blood replacement ranged from 2 to 17 U of red cell concentrate (Table 3).
RESULTS
After passage of the balloon, hemorrhage stopped in all patients. The balloon was kept insufflated for a period of time varying from 3 to 23 days, with a mean of 9 days. The definitive removal of the balloon occurred between the 6th and 24th postoperative day (Table 4). Six patients were discharged from the hospital with no local or systemic complications.
Two patients required a new surgical intervention for removal of the balloon because of the presence of epiploon adherences to the tube which prevented its removal. Both patients had a good course.
Two patients had fever and, after complementary imaging tests, were diagnosed to have subhepatic collections. Treatment with antibiotics was started and no additional surgical procedures were required for resolution. As mentioned earlier, one patient was submitted to hepatic artery ligation but no complications related to the procedure were observed.
One patient presented upper digestive hemorrhage on the lith postoperative day secondary to a duodenal ulcer when the balloon had already been removed. He was submitted to partial gastrectomy and discharged from the hospital without complications. In this second intervention, the path of the wound was evaluated and no evidence of bleeding or of a biliary fistula wasfound.
Two patients died, one due to acute hemorrhagic duodenal ulcer who was not operated upon and who developed bronchopneumonia and pleural empyema, and the other due to shock lung and acute renal failure caused by the initial severity of trauma.
Except for the two patients who developed complications and died (cases 2 and 12), the time of hospitalization ranged from 5 to 36 days, with a mean of 14,7 days.
DISCUSSION
The incidence of traumatic liver injury has increased over the last three decades (3,12,13). Several reports suggest that aproximately 80% of all traumatic liver injuries in civilian life can be treated by simple techniques such as suture, drainage or local compression and that only a reduced number of hepatic lesions require major procedures such as resection or cannulation of the inferior vena cava (1,5,8,9,22).
In view of the diversity of existing classifications with respect to traumatic injury to the liver, the American Association for the Surgery of Trauma has created a committee responsible for the classification of the various degrees of hepatic damage so as to standardize the information and permit comparison of data obtained by different groups (14). However, an interesting fact is that some transfixing wounds, although listed in the classification as grade II and III, behave similarly to hepatic lesions of more elevated grades due to the difficulty faced by the surgeon in approaching the wound and controlling hemorrhage in an efficient, rapid, and adequate manner.
The mortality rate for isolated hepatic lesions is approximately 5%, but when other organs are involved these rates exceed 50% (1,3,5,10,11,15,23). This fact was con-firmed in Brazil by Coimbra (4) who, using multivariate analysis, demonstrated that associated lesions interfere with delayed morbidity and with mortality. The same author also demonstrated that variables such as blood replacement, advanced age, abdominal complications and PATI of more than 20 are factors directly related to mortality rates.
In this patient series it was not possible to establish a direct correlation between haemodynamic conditions, trauma score, blood replacement and PATI, and morbidity and mortality because of the limited number of cases analyzed. Thus, the patient with a PATI of 52 did not present postoperative complications despite the replacement of 16 U of red cell concentrate, where as the patient with a PATI of 8 died on the 36th postoperative day. However, the patient that was admitted in shock with a trauma score of 11, who received 17 U of red cell concentrate and who had a PATI of 60, died on the 5th postoperative day. Fifty percent of the patients with a PATI of more than 23, excluding patient no 12, were hospitalized for 19 days, compared to 9.5 days for the remaining patients.
If the hepatic lesion is small or bleeding is minimal, haemostasis is obtained by simple procedures, but in more complex lesions the surgeon should start repair before establishing the haemodynamic conditions, only performing manual compression and the Pringle maneuver (7,11,19,20,23). As an alternative to the use of mass sutures that provoke ischaemia of the tissue portion involved, Patchier et al. in 1983 (18) proposed that haemostasis in the presence of deep wounds could be obtained by widening the path of the wound manually and by direct haemostasis of bleeding points. This technique permits definitive treatment and intrahepatic ligation of small vessels (18). Simple suture of the entrance and exit orifices or superficial tamponed of the wound may create conditions favorable to the appearance of intrahepatic collections, abscess formation or hemobilia (2,6). Furthermore, the path of the wound may deeply involve both lobes when crossing the caudate lobe, a fact that would hamper the approach based on direct exploration of the path.
In view of the above considerations, Morimoto et al. in 1987 (17) proposed the placement of a balloon through-out the path of the wound. The balloon should be made of nelation tubing and a Penrose drain arranged coaxially and filled with a mixture of saline and iodated contrast (17).
In our opinion, the advantages of using a tamponing balloon is the easy preparation of the device and the efficiency in obtaining hemostasis, with no need for major or more agressive surgical procedures that would excessively prolong operative time.
In this patient series, mean time of permanence of the insufflated balloon was 9 days, except for patients 2 and 12, in whom the balloon was maintained for 23 and 12 days, respectively. This was due to the extensive liver damage present, which in the first case involved the right and caudate lobes, and in the second the right and left lobes. Analysis of the present data and the acquired experience permit us to establish a period of 7 to 10 days as ideal for balloon permanence as long there is no recurrent bleeding.
It should be emphasized that drainage of the cavity should be maintained for at least 24 hours after balloon removal in order to detect possible bleeding or excess bile drainage. In addition to providing immediate hemostasis, the device represents a true transhepatic drainage by permiting the outflow of secretions and bile originating from the damaged hepatic ducts, thus avoiding or mini- mizing the occurrence and gravity of an eventual biliary fistula (2). If bleeding through the abdominal drain should occur after baloon deflation, an event never oserved by us, the balloon could be insufflated again and the patient would have the opportunity of being submitted to reoperation, if necessary, under stable hemodynamic conditions and with a surgical field free from bleeding.
As to blood volume replacement, we observed that the patients who received large amounts of blood (cases 5 and 12) had multiple associated lesions that represented potential bleeding points in addition to the hepatic lesion. The mean amount of red cell concentrate tranfused was 5 units and the mean amount of crystalloid solution was 4 150 ml. These data also confirm the need to use alternative methods, such as the intrahepatic balloon, for the treatment of complex hepatic lesions so that blood volume losses will be smaller and the surgeon will have the possibility of adequately treating other bleeding points.
Thus, on the basis of the present results, we believe that the intrahepatic balloon represents a valuable alternative for the treatment of transfixing lesions of the liver presenting abundant hemorrhage, representing a rapid and simple method for obtaining hemostasis.
- 01. ALDRETE, J.S.; HALPERN, N.B.; WARD, S. & WRIGHT, J.O. - Factors determining the mortality and morbidity in hepatic injuries. Ann Surg, 198:466-74, 1979.
- 02. BRANCO, P.D.; POGGETTI, R.; BERNINI, C.O. & BIROLINI, D. - Balão de tamponamento em ferimentos transfixantes do figado: resultados imediatos. Rev Hosp Clin Fac Med Sao Paulo, 43(1):20-5, 1988.
- 03. CARMONA, R.H.; LIM, R.C.Jr. & CLARK, C.G. - Morbidity and mortality in hepatic trauma. A 5 year study. Am J Surg, 144:88-94, 1982.
- 04. COIMBRA, R.S.M. - Ferimentos hepáticos penetrantes: estudo dos fatores relacionados a morbidade e mortalidade operatórias. Tese de Mestrado. Faculdade de Ciências Médicas da Santa Casa de São Paulo, 1992.
- 05. DEFORE, W.W.Jr.; MATTOX, K.L.; JORDAN, G. L. & BEALL, A.C.Jr. - Management of 1590 consecutive cases of liver trauma. Arch Surg, 111:493-7, 1976.
- 06. FELICIANO, D.V. - Cirurgia para traumatismo hepático. Clin. Cir Am N, 2:293-307, 1989.
- 07. FELICIANO, D.V. & PACHTER, H.L. - Hepatic trauma revisited. Curr Probl Surg, 26(7):457-524, 1989.
- 08. FREIRE, E. - Trauma do figado. Rev Col Bras Cir, 7:123- 42, 1980.
- 09. KLUG, W.A.; UCHOA, R.A.; PEREIRA, V. & RAHAL, F. - Ferimentos do fígado: Etiologia, diagnóstico e tratamento cirúrgico. Análise de 103 casos. An Paul Med Cir, 107(1): 13- 30, 1980.
- 10. LEVIN, A.; GOVER, P. & NANCE, F.C. - Surgical restraint in the management of hepatic injury. J Trauma, 18:399-404, 1978.
- 11. LUCAS, C.E. & LEDGERWOOD, A.M. - Prospective evaluation of hemostatic techniques for liver injuries. J Trauma, 16:422-5 1, 1976.
- 12. MAYS, E.T. - Complex penetrating hepatic wounds. Ann Surg, 173:421-8, 1971.
- 13. McCLELAND, R.N. & SHIRES, T. - Management of liver trauma in 259 consecutive patients. Ann Surg, 161:248-57, 1965.
- 14. MOORE, E.E. - Organ injury Scaling Committee. American Association for the Surgery of Trauma. December, 1988. In FELICIANO, D.V. & PACHTER, H.L. - Hepatic Trauma revisited. Curr Probl Surg, 26(7):475, 1989.
- 15. MOORE, E.E.; DUNN, E.L.; MOORE, J.B. & THOMPSON, J.S. - Penetrating abdominal trauma index. J Trauma, 21 :439- 45, 1981.
- 16. MOORE, F.A.; MOORE, E.E. & SEAGRAVES, A. - Nonresectional management of major hepatic trauma. Am J Surg, l50:725-9, 1985.
- 17. MORIMOTO, R.Y.; BIROLINI, D.; JUNQUEIRA, Jr., A.R.; POGGETTI, R. & HORITA, L.T. - Balloon tamponade for transfixing lesions of the liver. Surg Ginecol Obstet, 164:87- 8, 1987.
- 18. PACHTER, H.L.; SPENCER, F.C.; HOFSTETTER, S.R. & COPPA, G.F. - Experience with the finger fracture technique to achieve intra-hepatic hemostasis in 75 patients with severe injuries of the liver. Ann Surg, 197:771-8, 1983.
- 19. PACHTER, H.L.; SPENCER, F.C.; HOFSTETTER, S.R.; LIANG, H.C. & COPPA, G.F. - The management of juxta hepatic venous injuries without an atrio caval shunt: preliminary clinical observations. Surgery, 99:566-75, 1986.
- 20. PRINGLE, J.H. -Notes on the arrest of hepatic hemorrhage due to trauma. Ann Surg, 48:541-8, 1908.
- 21. STAIN, S.C.; YELLIN, A.E. & DONOVAN, A.J. - Hepatic trauma. Arch Surg, 123: 125 1-5, 1988.
- 22. TRUNKEY, D.D.; SHTRES, G.T. & McCLELLAND, R. - Management of liver trauma in 8 1 1 consecutive patients. Ann Surg, 179:722-8, 1974.
- 23. WALT, J.W. - The mithology of hepatic trauma - of Babel revisited. Am J Surg, 135: 12-8, 1978.Figure IegendsFig. 1 - Appearance of the prepared balloon.Fig. 2 - Intraoperative aspect of balloon positioning (see arrows).Fig. 3 - Radiologic aspect of balloon positioning (postoperative view).
Publication Dates
-
Publication in this collection
03 July 2009 -
Date of issue
Dec 1994