Abstracts
OBJECTIVE: To verify if the use of InGaAIP laser with 685 nm wave length can reduce the xerostomy incidence, the oral mucositis severity and the pain related to mucositis in patients with head and neck cancer submitted to radiotherapy. MATERIALS AND METHODS: Sixty patients presenting head and neck carcinoma were submitted to radiotherapy with daily doses of 1.8 to 2.0 Gy and a final dose of 45 to 72 Gy. The salivary volume was evaluated in the first and fifteenth days, at the end of the treatment and after 15 and 30 days. The oral mucositis was evaluated on a weekly basis. Twenty-nine patients were submitted to radiotherapy without laser and 31 were submitted to radiotherapy and laser with daily doses of 2 joules/cm² in predetermined areas of the oral mucosa and the parotid and submandibular glands. RESULTS: In the group submitted to radiotherapy and laser the incidence of mucositis (p < 0.001) and pain (p < 0.016) was significantly lower and the salivary volume (p < 0.001) was kept higher during and after the treatment. CONCLUSION: The group of patients submitted to radiotherapy and laser had lower incidence of xerostomy, oral mucositis and pain when compared to the group treated with radioteraphy without laser, producing statistically significant results.
Low level laser; Xerostomy; Mucositis; Radiotherapy; Chemotherapy
OBJETIVO: Verificar se o uso do laser de InGaAlP com comprimento de onda de 685 nm pode reduzir a incidência de xerostomia, gravidade da mucosite oral e da dor associada à mucosite em pacientes portadores de câncer de cabeça e pescoço submetidos a radioterapia. MATERIAIS E MÉTODOS: Sessenta pacientes portadores de carcinoma de cabeça e pescoço foram submetidos a radioterapia com dose diária de 1,8 a 2,0 Gy e dose final de 45 a 72 Gy. O volume salivar foi medido nos dias um, 15, ao final do tratamento e após 15 e 30 dias, e a mucosite oral em avaliações semanais. Vinte e nove pacientes se submeteram a radioterapia sem laser e 31 foram submetidos a radioterapia e laser com dose diária de 2 joules/cm² em pontos pré-determinados da mucosa oral e glândulas parótida e submandibular. RESULTADOS: No grupo submetido a radioterapia e laser, a incidência de mucosite (p < 0,001) e dor (p < 0,016) foram significativamente menores e o volume salivar se manteve maior (p < 0,001) durante e após o tratamento. CONCLUSÃO: Os pacientes submetidos à associação de radioterapia e laser tiveram menor incidência de xerostomia, mucosite oral e dor quando comparados ao grupo de radioterapia sem laser, com resultados com significância estatística.
Laser de baixa potência; Xerostomia; Mucosite; Radioterapia; Quimioterapia
ORIGINAL ARTICLE
Low-level laser therapy in the prevention of radiotherapy-induced xerostomia and oral mucositis* * Study developed at the Instituto de Radioterapia do Vale do Paraíba, São José dos Campos, SP, Brazil.
Carlos de Oliveira LopesI; Josepa Rigau I. MasII; Renato Amaro ZângaroIII
IMD Radiotherapist at Instituto de Radioterapia do Vale do Paraíba
IIDoctor-Professor at Unitat Histologia i Neurobiologia, Facultat Medicine i la Ciencies Salut, Universitat Rovira i Virgili, Tarragona, Spain
IIIProfessor at Instituto de Pesquisa e Desenvolvimento da Universidade do Vale do Paraíba
Mailing address Mailing address: Dr. Carlos de Oliveira Lopes Rua Major Antonio Domingues, 494, Centro São José dos Campos, SP, Brasil 12245-750 E-mail: colopes@uol.com.br
ABSTRACT
OBJECTIVE: To verify if the use of InGaAIP laser with 685 nm wave length can reduce the xerostomy incidence, the oral mucositis severity and the pain related to mucositis in patients with head and neck cancer submitted to radiotherapy.
MATERIALS AND METHODS: Sixty patients presenting head and neck carcinoma were submitted to radiotherapy with daily doses of 1.8 to 2.0 Gy and a final dose of 45 to 72 Gy. The salivary volume was evaluated in the first and fifteenth days, at the end of the treatment and after 15 and 30 days. The oral mucositis was evaluated on a weekly basis. Twenty-nine patients were submitted to radiotherapy without laser and 31 were submitted to radiotherapy and laser with daily doses of 2 joules/cm² in predetermined areas of the oral mucosa and the parotid and submandibular glands.
RESULTS: In the group submitted to radiotherapy and laser the incidence of mucositis (p < 0.001) and pain (p < 0.016) was significantly lower and the salivary volume (p < 0.001) was kept higher during and after the treatment.
CONCLUSION: The group of patients submitted to radiotherapy and laser had lower incidence of xerostomy, oral mucositis and pain when compared to the group treated with radioteraphy without laser, producing statistically significant results.
Keywords: Low level laser; Xerostomy; Mucositis; Radiotherapy; Chemotherapy.
INTRODUCTION
The head and neck radiotherapy (RT) is always followed by complications, during or even after treatment especially if associated with chemotherapy , principally in the oral mucosa (mucosistis) and salivary glands (xerostomia)(1).
The oral mucositis is a clinical problem of difficult control that may compromise the deglutition, the food ingestion, the oral hygiene and the patient's communication capability, many times compelling the interruption of RT with an evident impairment to the treatment(25).
The xerostomia appears soon after the beginning of the RT, becoming more evident after 20Gy doses. Initially, the saliva becomes thicker and its elimination rate decreases(6). The changes in salivary flow, volume and viscosity may be related to vascular damages to the salivary glands and may persist for years. The recovery of a normal production of saliva will depend on the characteristics of each patient and the salivary gland irradiated percentage(7). This xerostomia may be irreversible, although there is a tendency of recovering up to 50% of the initial salivary volume, if both the irradiated parotid volume and the final irradiation dose remain in the lowest possible values(812).
Literature describes several techniques for xerostomia and oral mucositis prevention such as the use of amifostine, pilocarpine, Biotene®, sodium bicarbonate mouthwash, use of antibiotics and topic anesthetic, among others, but all of them are limited(1319).
The low level laser (LLL) is a low-energy laser, without photothermal potential, used for biomodulation. The most frequently used lasers are in the red range (632 to 780 nm), with photons of energy below 2.0 electron-volt (eV), therefore lower than the energy of biological molecular binding and DNA, not being able to break chemical bindings and to induce mutations and carcinogenesis(2023).
The LLL irradiation effect is based on the modulation capacity of several metabolic processes, by means of luminous energy conversion through biochemical and photophysical processes which transform the laser light into energy useful for the cell(23). The visible laser causes mitochondrial reactions, an increase in the cell glycosis consumption, in the intracellular calcium concentration and in the number of cellular mitochondria. An increase in the number of mitosis in rats submandibular glands ducts submitted to GaAs laser irradiation also is described(2430).
Publications show the use of neon-helium laser as an agent capable of reducing the intensity of oral mucositis and pain in patients undergoing RT and chemotherapy and in those submitted to autologous bone marrow transplantation(3135).
Published studies show the efficacy of the LLL as a salivary stimulator in patients affected by xerostomia, sialodenitis and Sjögren syndrome(3639).
The objective of this study was to verify if the use of InGaAIP 685 nm wavelength laser can reduce the xerostomy incidence, the oral mucositis severity and the pain associated with mucositis in patients with head and neck cancer submitted to RT.
MATERIALS AND METHODS
Ethics in research with human beings
This study was approved by the Committee of Ethics in Research with Human Beings of the Universidade do Vale do Paraíba, affiliated to the National Council of Research with Human Beings (Conselho Nacional de Pesquisa com Seres Humanos Conep), in compliance with the resolution no. 196/96 of the Health Ministry of Brazil, according to protocol no. L001/2002/CEP. The participating volunteers have signed a consent form including guidance about the project.
Population and inclusion/exclusion criteria
The study was performed in a group of voluntary patients aged above 21 years, bearing head and neck carcinomas and not submitted to previous RT in the affected region and patients whose the irradiation fields included the salivary glands. The patients with dossiers bearing odd numbers were denominated "control", receiving RT without laser; and the patients with dossiers bearing even numbers were submitted to RT and laser therapy. From March to September 2002, 60 patients were randomized in a group of 29 patients submitted to RT without laser and in another group of 31 patients submitted to concomitant RT and laser therapy.
All the patients were submitted to free initial dental care and to the best clinical support treatment for the whole therapy period.
Laser light application
A 685 nm wavelength InGaAlP laser was used. The application modality was "by contact" on three points of each parotid, one right and left submandibular, two points on the right and left jugal mucosa, one point on each side of the mouth floor, two points on mobile tongue, one point on the right pillar, another on the left pillar and another on the uvula region, all of them with 2.0 joules/cm² energy density per point.
The laser parameters were: 50 mW nominal power and 35 mW real power in a fibre (diameter of 400 µm), 58 s irradiation time, 685 nm wavelength and dose density of 2,0 joules/cm². If the application point was at less than 1 cm from the tumoral area, the LLL application was not made on that site(33).
Radiotherapy
Daily sessions were performed employing a Varian® (Varian Medical Systems) 4 MeV photons linear accelerator. The irradiated areas were delimited according to technical principles included in RT manuals(4043).
The patients were submitted to routine staging examinations, including clinical and endoscopic tests, laboratory tests, tomography studies, biopsies, etc.
The patients were positioned in dorsal decubitus, immobilized with a thermoplastic mask and submitted to control X-rays.
Daily doses ranged between 1.8 and 2.0 Gy, calculated during the planning, and the final doses remained at 4572 Gy, in 25 to 40 days of treatment.
The fields were the right and left cervicofacial, and the supraclavicular fossae.
Chemotherapy
The chemotherapy used in association with RT was cisplatine in weekly doses of 40 mg/m²(44).
Xerostomia evaluation
The xerostomia evaluation was performed according scheme proposed for sialometry by the Radiation Therapy Oncology Group (RTOG) 97-09(45). The initial evaluation was performed on the first day of the RT treatment and worked as an indicator of the salivary production basal level. The non-stimulated production of saliva was evaluated previously to the evaluation of the stimulated production. Initially, the patient was asked to swallow all the saliva in the mouth. Following this, the patient was asked to accumulate the saliva without swallowing it, during 60 seconds. That saliva was accumulated in a 50 ml graded bottle. This procedure was repeated 4 times more, totalling five collections in five minutes. The salivary production stimulation was made with a 2% sodium citrate solution applied on the dorsolateral borders of the tongue, using a cottonete, for five times in a two-minute period. (0, 30, 60, 90 and 120 seconds). Previously to the application of the solution, the mouth was cleaned and any secretion was removed, and afterwards it was cleaned once more for removal of the residual sodium citrate. So, the saliva was collected in the same way adopted for the non-stimulated salivation procedure. These measurements were performed on the days 1, 15, at the end of the treatment and within 15 and 30 post-treatment days.
Oral mucositis evaluation
This evaluation was made on a weekly basis and the mucosistis degree was rated in compliance with the National Cancer Institute (NCI) guidelines, as shown in Table 1(46).
Pain evaluation
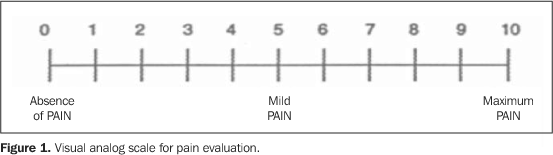
The evaluation was performed according to a numeric analog scale in which the patient was asked to assign a grade for his/her degree of pain in the oral mucosa (Figure 1).
Statistical analysis
A statistical analysis was part of the comparison between the two groups and included a calculation of central tendency measures (mean) and dispersion (standard deviation) for quantitative variables as well as frequency distributions (%) for qualitative variables. In Tables 2 x 2, where at least one of the expected frequencies was <5, the Fisher's exact test was applied. For the quantitative variables measures comparison (age and irradiation doses) between the studied groups, the Student's test was applied for independent samples. When the assumption of the variables normal distribution was not confirmed, the Mann-Whitney's test (non-parametric) was applied. For the repeated measures analysis of variance (ANOVA), the time was the repeated measure, and group was the independent variable. When the variances between groups were not homogeneous, the Friedman's test was applied, as a non-parametric equivalent. In the presence of statistically significant differences, the ANOVA was supplemented by the Tukey-HSD multiple comparisons test.
RESULTS
Results of 60 patients were analyzed 29 submitted to RT without laser therapy and 31 submitted to RT and laser therapy. Most of them were men (83.3%). The age ranged between 28 and 88 years (average 57.4 ± 13.9 years).
The most frequent sites of primary tumors were: larynx (18.3%), amygdale (10.0%) and tongue (8.3%). The spinocellular carcinoma was the predominant histological type (85.0%).
The majority of the patients presented advanced tumors (clinical stage IV) (76.7%). Thirty-four patients (56.7%) were not submitted to surgery and 31 were not given chemotherapy (51.7%) (Table 2).
Doses in the salivary glands: Statistically significant differences were not observed between the total dose averages in the right (p = 0.081) and left (p = 0.090) parotid glands; right (p = 0.081) and left (p = 0.090) submandibular glands; right (p = 0.081) and left (p = 0.090) sublingual glands in the groups treated with or without laser (Table 3).
Stimulated salivary flow: A statistically significant difference between the groups was observed (p < 0,001) (Table 4).
Non-stimulated salivary flow: There was a statistically significant difference between the groups (p < 0,001) (Table 5).
Mucositis NCI score: Statistically significant differences were observed between moments (p < 0,001) and between groups (p < 0,001). A statistically significant interaction was observed between moment and group (p < 0,001), i.e., the variation between the moments is different in both studied groups (Table 6).
Pain analog scale: There was a statistically significant difference between the studied groups (p < 0,001) (Table 7).
DISCUSSION
Univariate analysis of data collected showed no statistically significant difference between the groups regarding sex, age, base-disease, staging, irradiation doses in salivary glands, association with surgery or chemotherapy, histological type and primary tumor site.
Evaluation of data regarding oral mucositis incidence, pain and xerostomia, showed that patients submitted to RT and laser therapy had significantly lower indexes of these events when compared to the RT without laser therapy group. Bensadoun et al.(33) developed a randomized study with 30 patients, using helium-neon laser, with positive results in the reduction of the radio-induced mucositis and pain severity in patients submitted to neck and head RT. In our study, besides including a higher number of cases (a total of 60), we have also equalized all patients initial oral hygiene conditions as well as the better support of dental care during the treatment.
The patients submitted to RT and laser therapy evolved with a lower incidence of mucositis and pain due to the treatment. Our data are in compliance with those of Cowen et al.(32), who have compared the oral mucositis evolution in 30 patients who had undergone autologous bone marrow transplant and RT in the period from 1993 to 1995, with a significant reduction of mucositis, and considering the prophylactic laser application as an advantageous method in relation to the curative method.
In our study, the application was performed since the beginning of the RT and was extended for the whole treatment period.
Due to social or personal reasons, some patients have not followed such a rigid conduct and have failed to attend treatment sessions, sometimes for up to five consecutive days. As an example, there was a patient bearing rhinopharynx carcinoma and undergoing RT + chemotherapy + laser therapy, who decided not to attend the laser sessions during a whole week due to the excess of saliva. The mucositis worsening brought him back to the initial therapeutic plan right after a few days of laser applications. This has led us to review the daily necessity of laser applications so, in the future, we plan to study a group with three weekly sessions, comparing the results.
During the study, we have observed that, in the RT + laser therapy group, all the patients completed the planned treatment, while in the RT without laser therapy group, four patients of a total of 29 (13.8%) had their treatment suspended due to mucositis. This observation is compatible with the study of Balakirev et al.(35) about the employment of laser for oral mucositis prevention. This study concluded that the treatment interruption time necessary for handling the complications resulting from RT and chemotherapy side effects in pediatric patients decreased in up to 1.5-2 times in the group concomitantly submitted to laser therapy. We have not found in the literature any study aiming at showing the usefulness of the laser for xerostomia prevention during the RT period. However, there are several studies on the laser effectiveness as salivary glands stimulator. Among them, we can mention Katz(38,39), about the employment of helium-neon laser in sialodenitis; Fructuoso & Moset(36) and Takeda(24), using GaAs 904 nm wavelength laser, and Nagasawa(37), using GaAlAs 820 nm wavelength laser in patients affected by Sjögren syndrome, resulting in an improvement of the salivary flow produced by the parotid gland after laser-light stimulation.
Our data are in compliance with the literature and have shown that in the group of patients submitted to concomitant RT and laser therapy there was a lower decrease in the salivary volume than in the group submitted to RT not associated to laser therapy where all the patients showed a progressive volume decrease of the stimulated and non-stimulated saliva with a tendency to volumes lower than 1.0 ml. In the group of patients submitted to RT associated with laser therapy, there were some cases of increase in the salivary volume during the RT % a fact that at no time we have observed during years of work in this specialty, even making use of sodium bicarbonate mouthwashes, Biotene®, artificial saliva and other support clinical treatments of the routine medical practice.
Although with no statistical value, our re-evaluations have shown that the salivary volume in patients submitted to RT + laser therapy has been kept at higher levels than in patients undergoing RT without laser therapy (Figure 2). It is our first impression that this benefit tends to be prolonged and the patients should be followed-up for the next months or years. Successive re-evaluations of their salivary volume will be useful for showing if this initial benefit will persist.
CONCLUSIONS
The xerostomia incidence was significantly lower in patients submitted to RT and laser therapy.
The utilization of laser in association with RT reduced the oral mucositis severity.
The pain associated with oral mucositis also is significantly reduced in patients submitted to RT and laser therapy.
REFERENCES
Received April 11, 2005.
Accepted after revision July 5, 2005.
- 1. Trotti A. Toxicity in head and neck cancer: a review of trends and issues. Int J Radiat Oncol Biol Phys 2000;47:112.
- 2. Bonassa EMA. Enfermagem em quimioterapia. São Paulo: Atheneu, 1998;238.
- 3. Fontelonga A. Mucosite. A saúde na internet. São Paulo; 2001 [acessado em 5 nov 2001]. Disponível em: http://www.saudenainternet-rede MNI.htm
- 4. Carl W, Havens J. The cancer patient with severe mucositis. Curr Rev Pain 2000;3:197202.
- 5. Devita VT Jr. Oral complications. In: Cancer: principles and practice of oncology. 6th ed. Philadelphia, PA: Lippincott Williams & Wilkins, 2001; 28812888.
- 6. Semba SE, Mealey BL, Hallmon WW. The head and neck radiotherapy patient: Part 1 oral manifestations of radiation therapy. Compend Contin Educ Dent 1994;15:252260.
- 7. Fajardo LF, Bertrong M, Anderson RE. Salivary glands In: Fajardo LF, Bertrong M, Anderson RE, editors. Radiation pathology. Minnesota: Oxford University Press, 2001;265270.
- 8. Chao KS, Deasy JO, Markmon J, et al A prospective study of salivary function sparing in patients with head-and-neck cancers receiving intensity-modulated or three-dimensional radiation therapy: initial results. Int J Radiat Oncol Biol Phys 2001; 49:907916.
- 9. Burlage FR, Coppes RP, Meertens H, et al. Parotid and submandibular/sublingual salivary flow during high dose radiotherapy. Radiother Oncol 2001;61: 271274.
- 10. Roesink JM, Moerland MA, Battermann JJ, et al. Quantitative dose-volume response analysis of changes in parotid gland function after radiotherapy in the head-and-neck region. Int J Radiat Oncol Biol Phys 2001;51:938946.
- 11. Maes A, Weltens C, Flamen P, et al. Preservation of parotid function with uncomplicated conformal radiotherapy. Radiother Oncol 2002;63:203211.
- 12. Cheng VST, Downs J, Herbert D, Aramany M. The function of the parotid gland following radiation therapy for head and neck cancer. Int J Radiat Oncol Biol Phys1981;7:253258.
- 13. Johnson JT, Ferreti GA, Nethery WJ, et al. Oral pilocarpine for post-irradiation xerostomia in patients with head and neck cancer. N Engl J Med 1993;329:390395.
- 14. Rieke JW, Hafermann MD, Johnson JT, et al. Oral pilocarpine for radiation-induced xerostomia: integrated efficacy and safety results from two prospective randomized clinical trials. Int J Radiat Oncol Biol Phys 1995;31:661669.
- 15. Schuchter LM, Hensley ML, Meropal NJ, et al. 2002 Update of recommendations for the use of chemotherapy and radiotherapy protectants: clinical practice guidelines of the American Society of Clinical Oncology. J Clin Oncol 2002;20:28952903.
- 16. Warde P, Krall B, O'Sullivan B, et al. A phase II study of Biotene in the treatment of postradiation xerostomia in patients with head and neck cancer. Support Care Cancer 2000;8:203208.
- 17. Antonadou D, Pepelassi M, Synodinou M, Puglisi M, Throuvalas N. Prophylactic use of amifostine to prevent radiochemotherapy-induced mucositis and xerostomia in head-and-neck cancer. Int J Radiat Oncol Biol Phys 2002;52:739747.
- 18. Epstein JB, Schubert MM. Synergistic effect of sialagogues in management of xerostomia after radiation therapy. Oral Surg Oral Med Oral Pathol 1987;64:179182.
- 19. Schubert MM, Franquini JC, Niccoli-Filho F, et al. Effects of low-energy laser on oral mucositis: a phase I/II pilot study. Cancer Res Weekly 1994;7:14.
- 20. Brugnera Jr A, Pinheiro ALB. Lasers na odontologia moderna. São Paulo, SP: Pancast, 1998.
- 21. Tunér J, Hode L. Low level laser therapy. Graengesberg, Sweden: Prima Books, 1999;403.
- 22. Maldonado EP. Mecanismos de interação laser-tecido [apostila do curso de mestrado profissionalizante de lasers em odontologia do Ipen]. São Paulo, SP: Ipen, 2000.
- 23. Cisneros JLV. Láser y fuentes de luz pulsada intensa em dermatología y dermocosmética. Madrid: Aula Médica Ediciones, 2000.
- 24. Takeda Y. Irradiation effect of low-energy laser on rat submandibular salivary gland. J Oral Pathol 1988;17:9194.
- 25. Bortolleto R. Efeito da radiação do laser de baixa potência no potencial de membrana de mitocôndrias em células in-vitro. (Dissertação de Mestrado). São José dos Campos, SP: Universidade do Vale do Paraíba, 2000.
- 26. Rigau J. Acción de la luz láser a baja densidad en la modulación de la función celular. (Tesis de Doctorado). Reus-Tarragona, Espanha: Universidad Rovira y Virgili, 1996.
- 27. Karu TI. Photobiological fundamentals of low-power laser therapy. J Quantum Electronics Moscow 1987;QE-23(10):17031717.
- 28. Mester AF, Mester A. Wound healing. Laser Therapy 1989;1:715.
- 29. Hashieh IA, Tardieu C, Franquin JC. Helium-neon laser irradiation is not a stressful treatment: a study on heat-shock protein (HSP70) level. Lasers Surg Med 1997;4 :451460.
- 30. Genovese WJ. Laser de baixa intensidade: aplicações terapêuticas em odontologia. São Paulo, SP: Lovise, 2000.
- 31. Barasch A, Peterson DE, Tanzer JM, et al. Helium-neon laser effects on conditioning induced oral mucositis in bone marrow transplantation patients. Cancer 1995;76:25502556.
- 32. Cowen D, Tardieu C, Schubert M, et al Low energy helium-neon laser in the prevention of oral mucositis in patients undergoing bone marrow transplant: results of a double blind randomized trial. Int J Radiat Oncol Biol Phys 1997;38:697703.
- 33. Bensadoun RJ, Franquin JC, Ciais G. Low-energy He/Ne laser in the prevention of radiation-induced mucositis. A multicenter phase III randomized study in patients with head and neck cancer. Support Care Cancer 1999;7:244252.
- 34. Plevová P. Prevention and treatment of chemotherapy and radiotherapy induced oral mucositis: a review. Oral Oncol 1999;5:453470.
- 35. Balakirev SA, Gusev LI, Kasanova MB, et al Low-intensity laser therapy in pediatric oncology. Vopr Onkol 2000;46:459461.
- 36. Fructuoso FJG, Moset J M. Randomized double blind study on biostimulatory effect of laser irradiation of the parotid gland in patients suffering of Sjögren syndrome. Invest y Clinica Laser 1987;1: 1825.
- 37. Nagasawa A. Application of LLLT in dentistry. In: Ohshiro T, editor. Low-reactive laser therapy. Practical applications. London: John Wiley & Sons, 1991;76.
- 38. Kats AG. Low-energy laser radiation in the combined treatment of salivary gland inflammation. Stomatologia (Mosk) 1993;4:3236.
- 39. Kats AG, Belastotskaia IM, Malamud ZP, et al. Remote results of the complex treatment of chronic sialadenitis using the helium-neon laser. Vestnik Khirurgii Imeni I-I Grekova 1985;135:3942.
- 40. Hall EJ. Radiobiology for the radiologist. 4th ed. Philadelphia, PA: JB Lippincott, 1994;113.
- 41. Bentel GC. Radiation therapy planning. 2nd ed. New York, NY: McGraw-Hill, 1996;268330.
- 42. Perez CA, Brady LW. Principles and practice of radiation oncology. 3rd ed. Philadelphia, PA: Lippincott-Raven, 1998;9811002.
- 43. Leibel SA, Phillips TL. Textbook of radiation oncology. Philadelphia, PA: WB Saunders, 1998; 412526.
- 44. Gomes R. Oncologia básica. Rio de Janeiro, RJ: Revinter, 1997.
-
4545. Radiation Therapy Oncology Group. A phase III study to test the efficacy of the prophylatic use of oral pilocarpine to reduce hyposalivation and mucositis associated with curative radiation therapy in head and neck cancer patients. RTOG97-09. Philadelphia, PA: Radiation Therapy Oncology Group, 1999.
- 46. Trotti A, Byhardt R, Stetz J, et al. Common toxicity criteria: version 2.0. An improved reference for grading the effects of cancer treatment: impact on radiotherapy. Int J Radiat Biol Oncol Phys 2000; 47:1347.
Publication Dates
-
Publication in this collection
25 May 2006 -
Date of issue
Apr 2006
History
-
Accepted
05 July 2005 -
Received
11 Apr 2005