ABSTRACT
The current world Covid-19 pandemic has been the most discussed topic in the media and scientific journals. Fear, uncertainty, and lack of knowledge about the disease may be the significant factors that justify such reality. It has been known that the disease presents with a rapidly spreading, it is significantly more severe among the elderly, and it has a substantial global socioeconomic impact. Besides the challenges associated with the unknown, there are other factors, such as the deluge of information. In this regard, the high number of scientific publications, encompassing in vitro, case studies, observational and randomized clinical studies, and even systematic reviews add up to the uncertainty. Such a situation is even worse when considering that most healthcare professionals lack adequate knowledge to critically appraise the scientific method, something that has been previously addressed by some authors. Therefore, it is of utmost importance that expert societies supported by data provided by the World Health Organization and the National Health Department take the lead in spreading trustworthy and reliable information. The Brazilian College of Surgeons suggests in this document various initiatives that may help surgeons, healthcare providers, and patients who will have to face a surgical event under the pandemic.
Keywords:
Pandemics; General Surgery; Preoperative Care; Intraoperative Care; Postoperative Care; Disaster Planning
RESUMO
A atual pandemia do novo coronavírus, Covid-19, tem sido o assunto mais discutido no momento, tanto na mídia como em periódicos científicos. O medo, a incerteza e o desconhecimento sobre o comportamento da doença são os fatores preponderantes que podem justificar essa realidade. Sabe-se de antemão que a enfermidade tem grande disseminação, é mais grave entre idosos e está associada a grande impacto socioeconômico mundial. Além dos desafios em lidar com o desconhecido, há outros relacionados com a sobrecarga de informação e nesse quesito, a grande quantidade de estudos científicos, que englobam pesquisas in vitro, relatos de casos, estudos observacionais e randomizados, além de revisões sistemáticas complementam o panorama de dúvidas. Essa situação é piorada porque o conhecimento sobre o método científico não é dominado pela maioria dos profissionais de saúde, algo que há muito já vem sendo divulgado por vários autores. De sorte que em função desta realidade, torna-se fundamental que sociedades de especialidades apoiadas por dados da Organização Mundial da Saúde e do Ministério da Saúde assumam a liderança da divulgação da informação correta e confiável. O Colégio Brasileiro de Cirurgiões sugere neste documento medidas que podem auxiliar cirurgiões e outros profissionais de saúde, assim como pacientes, em caso de necessidade cirúrgica, a lidar com a atual pandemia.
Descritores:
Pandemias; Cirurgia Geral; Cuidados Pré-Operatórios; Cuidados Intra-Operatórios; Cuidados Pós-Operatórios; Organizações de Planejamento e Atendimento a Desastre
The new coronavirus pandemic, Covid-19, is the current most discussed topic, both by the popular imagery and media, as well as by the scientific world. This situation is due to the fear, uncertainty, and mainly the lack of knowledge regarding the disease. Beforehand, it can be stated that this illness has a geometric capacity of dissemination, a tremendous global socioeconomic impact and high lethality, which, although low considering the world population, it seems to be extremely high among the elderly, in particular, in Italy.
The disease has strongly influenced everyone’s daily routine. Mandatorily social isolation rules, the closing of national borders, and planning for disaster health care initiatives have permeated the current news worldwide. There is no doubt the Covid-19 has become part of everybody’s daily life with unprecedented conditions.
Google search using the words “Covid-19”, “Covid19”, “Covid 19”, “Covid-19 Brazil”, “coronavirus” and “coronavirus Brazil” has provided nine billion results, and five billion when the country is specified. These are astounding numbers that certainly impress any skeptical person who has challenged the veracity of the pandemic while at the same time raises the awareness of those who are well acquainted with its impact on the contemporary global society, mainly those working in the healthcare business. In this context, the doctors are not only responsible for screening, diagnosing, and taking care of the Covid-19 patients, but they are also required to express their opinion about the current situation. The latter demands knowledge about the disease and optimal preparation to face it, something rough under any circumstances, since this is a new disease, emerging at the end of 2019. Despite this situation, in not more than three months, the scientific literature has offered a significant number of publications regarding the disease, covering from in vitro experiments, case studies, potential medication to be prescribed and systematic reviews11 Salehi S, Abedi A, Balakrishnan S, Gholamrezanezhad A. Coronavirus Disease 2019 (COVID-19): A Systematic Review of Imaging Findings in 919 Patients. AJR Am J Roentgenol. 2020:1-7..
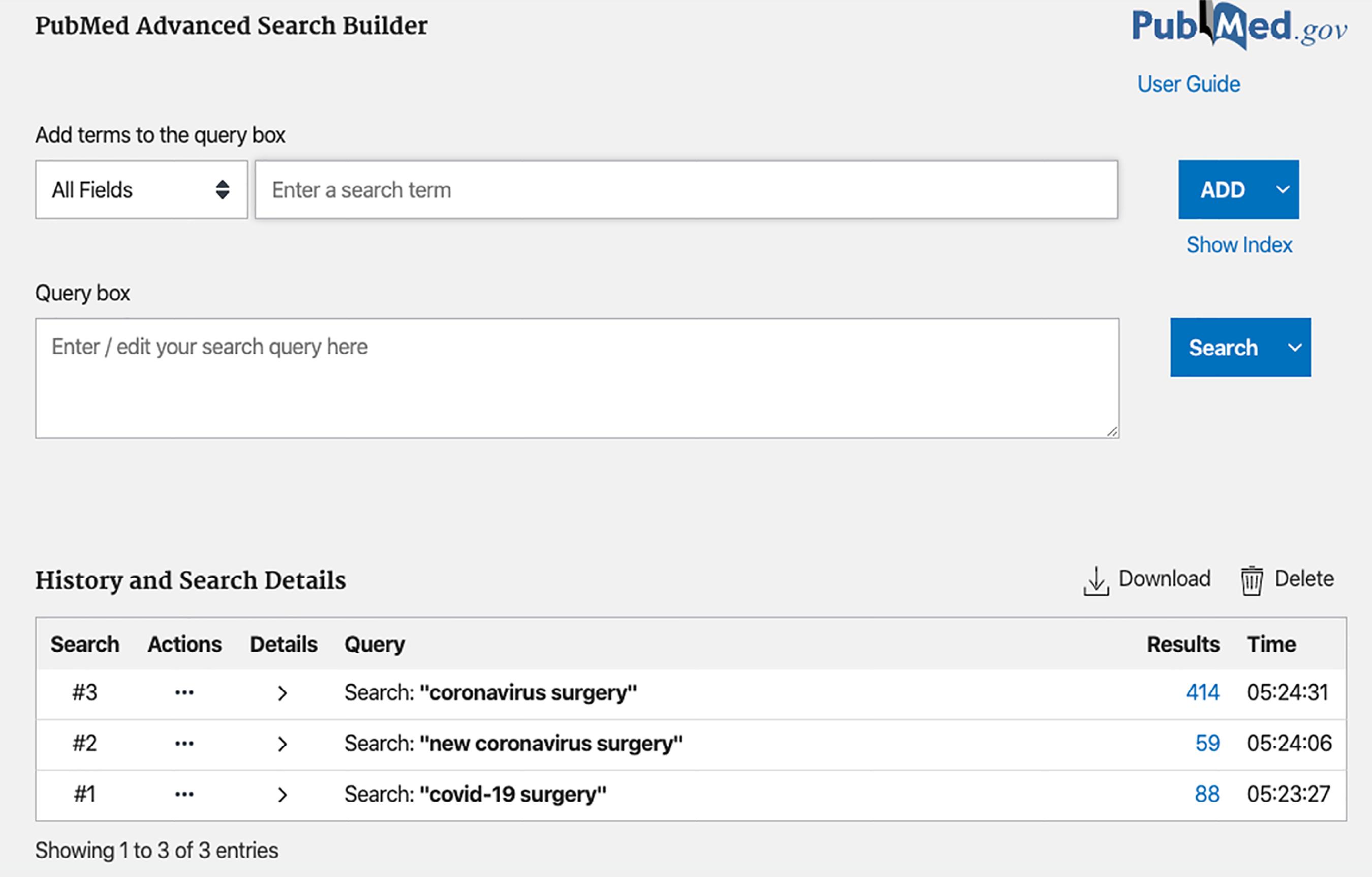
In Pubmed, according to the used keywords, there are between 1300 to 3000 manuscripts, which indicates how relevant the subject is (figure 1)22 Pubmed [Available from: https://pubmed.ncbi.nlm.nih.gov/.
https://pubmed.ncbi.nlm.nih.gov/...
. On the other hand, it is challenging to have the capacity to read, assess and conclude about the best strategy or treatment applied to each one’s reality. It is also important to consider the required amount of time to read all the articles. Furthermore, the lack of knowledge to critically appraise the scientific method, makes it even more difficult to get to conclusions. Ever since long ago, Jonh Ioannidis has been challenging how science has been carried out, in particular, regarding the used methods and the lack of critical appraise by the healthcare professionals33 Ioannidis JPA. Randomized controlled trials: Often flawed, mostly useless, clearly indispensable: A commentary on Deaton and Cartwright. Soc Sci Med. 2018.
4 Ioannidis JPA. Hijacked evidence-based medicine: stay the course and throw the pirates overboard. J Clin Epidemiol. 2017;84:11-3.
5 Ioannidis JP. Evidence-based medicine has been hijacked: a report to David Sackett. J Clin Epidemiol. 2016;73:82-6.-66 Ioannidis JP. Why most published research findings are false. PLoS Med. 2005;2(8):e124.. In a recent provocative text, Ioannidis shoots his “methodological machine gun” against the data regarding the Covid-1977 Ioannidis JPA. A fiasco in the making? As the coronavirus pandemic takes hold, we are making decisions without reliable data Statnew: Boston Globe; 2020 [Available from: https://www.statnews.com/2020/03/17/a-fiasco-in-the-making-as-the-coronavirus-pandemic-takes-hold-we-are-making-decisions-without-reliable-data/?fbclid=IwAR0r5W-fu7C4Qi19bUdiW_ekgbTu6HpP98xx5BBaZjL1bZn5QjIvaVbm3yc.
https://www.statnews.com/2020/03/17/a-fi...
. All these uncertainties increase the responsibility of those who, perhaps, can better inform the general population and also the physicians: the World Health Organization, the National Health Department, and the medical societies. Nonetheless, this is not an easy task and may be marked by controversies, once what today may seem logical, tomorrow might be challenged. Afterward, transitory truths have been Medicine’s trademark.
The experienced and wise Professor Saul Goldenberg, some years ago, questioned, “As a scientific journal editor, I always ask myself: how to be convinced about the veracity of one manuscript? How to differentiate the true from the fake”88 Goldenberg S. [Reflections on the truth]. Acta Cir Bras. 2007;22(6):420-1.. Ioannidis, on the other hand, states that the majority of scientific articles are fake66 Ioannidis JP. Why most published research findings are false. PLoS Med. 2005;2(8):e124.. In regard to this situation, many professionals believe that the best way to solve the deluge of scientific information99 C A. The End of Theory: The Data Deluge Makes the Scientific Method Obsolete https://www.wired.com/2008/06/pb-theory/2008 [
https://www.wired.com/2008/06/pb-theory/...
is to read systematic reviews, metanalysis, and guidelines, mainly from trustworthy sources such as Cochrane, which also requires a critical appraisal. The latter are not spared of controversies, and their scientific impartiality has been challenged33 Ioannidis JPA. Randomized controlled trials: Often flawed, mostly useless, clearly indispensable: A commentary on Deaton and Cartwright. Soc Sci Med. 2018.,44 Ioannidis JPA. Hijacked evidence-based medicine: stay the course and throw the pirates overboard. J Clin Epidemiol. 2017;84:11-3.,1010 Askheim C, Sandset T, Engebretsen E. Who cares? The lost legacy of Archie Cochrane. Med Humanit. 2017;43(1):41-6.
11 Noone KJ. Beware the impact factor. Ambio. 2016;45(5):513-5.-1212 Correia M. Are we capable of separating the wheat from the chaff when assessing meta-analyses? Clin Nutr. 2020;39(3):705-7.. Furthermore, under the current situation, it is challenging to publish material with a high level of evidence. However, the principles of Evidence-Based Medicine, by definition require “the conscious, explicit and judicious use of the best available evidence to help decide for patient care”1212 Correia M. Are we capable of separating the wheat from the chaff when assessing meta-analyses? Clin Nutr. 2020;39(3):705-7.. If what it has been published, until now, is of low evidence, including clinical off-label treatment trials, this is what it is available to face the current pandemic. Therefore, the scientific community must critically appraise the studies and be careful while analyzing the data. As members of scientific expert societies, we face crucial dilemma to provide adequate information and clarify about facts and truths, despite the meek evidence that may be prone to change in the future. In this regard, the Brazilian College of Surgeons, with its nonagenarian maturity, utilizing its scientific journal, herein, suggests quality and safety initiatives, supported by the available current surgical literature aiming to help surgeons and patients face this critical moment1313 Brindle M, Gawande A. Managing COVID-19 in Surgical Systems. Ann Surg. 2020;accepted(on line).
14 Surgeons TcotQpotACo. Maintaining trauma Center Acess and Care during the Covid-19 Pandemic: Guidance Document for Trauma Medical Directors 2020 [Available from: https://www.facs.org/quality-programs/trauma/maintaining-access.
https://www.facs.org/quality-programs/tr...
15 Surgeons ACo. Covid-19 Recommendations for Management of Elective Surgical Procedures [Available from: https://www.facs.org/about-acs/covid-19/information-for-surgeons.
https://www.facs.org/about-acs/covid-19/...
16 Aminian A, Safari S, Razeghian_Jahromi A, Ghorbani M, Delaney CP. Covid-19 Outbreak and Surgical Practice: Unexpected Fatality in Perioperative Period. Ann Surg. 2020;on line.-1717 Zheng MH, boni L, Fingerhut A. MInimally invasive surgery and the novel coronavirus outbreak: lessons learned in China and Italy. Ann Surg. 2020;on line.. The Brazilian Healthcare Department guidelines1818 Saúde Md. 2020 [cited 2020 March, 22nd 2020]. Available from: https://saude.gov.br/.
https://saude.gov.br/...
, under the steady leadership of its Secretary Dr. Luiz Henrique Mandetta, himself an orthopedic surgeon, and the information provided by the World Health Organization1919 Organization WH. Rolling updates on coronavirus disease (COVID-19). 2020. also support these recommendations.
The truth is that the healthcare services must be prepared for the current emergency that rapidly spreads, and changes exponentially at any time. In reality, the healthcare services should have permanent quality and safe strategies/guidelines2020 Saúde Md. Cirurgias seguras salvam vidas Rio de Janeiro: Organização Pan-Americana da Saúde ; Ministério da Saúde ; Agência Nacional de Vigilância Sanitária; 2009 [Available from: http://bvsms.saude.gov.br/bvs/publicacoes/seguranca_paciente_cirurgias_seguras_guia.pdf.
http://bvsms.saude.gov.br/bvs/publicacoe...
, which should also encompass nature disasters, war, and pandemic topics, that are crucial under the current situation1313 Brindle M, Gawande A. Managing COVID-19 in Surgical Systems. Ann Surg. 2020;accepted(on line).. Therefore:
-
• Elective surgical procedures should be postponed to a more appropriate time.
-
○ Rational: 1) the need for available room/spaces to host more patients; 2) to make available more mechanical ventilators in case of increased demand1313 Brindle M, Gawande A. Managing COVID-19 in Surgical Systems. Ann Surg. 2020;accepted(on line).; 3) to prevent adverse events in patients undergoing expected low morbimortality procedures but that became fatal because of Covid-19 infection in asymptomatic individuals1616 Aminian A, Safari S, Razeghian_Jahromi A, Ghorbani M, Delaney CP. Covid-19 Outbreak and Surgical Practice: Unexpected Fatality in Perioperative Period. Ann Surg. 2020;on line..
-
-
• To ensure planning strategies to carry out urgent/emergency operations during the pandemic
-
○ Rational: 1) to ensure an adequate treatment for trauma patients, those with digestive bleeding or severe infection, for example, who require immediate surgery; 2) to prepare and guide all the healthcare professionals on how to act, adequately protecting themselves with individual protection equipment (IPE); 3) to allow the minimum required people in the surgical room, thus preventing the risk of contamination of other individuals. In this regard, this is a mandatory percept of quality and safety initiatives not only for disasters and pandemics1313 Brindle M, Gawande A. Managing COVID-19 in Surgical Systems. Ann Surg. 2020;accepted(on line)..
-
-
• To define, when possible, and taking into consideration the type of hospital and the assisting trajectory, specific operating rooms for urgent/emergent procedures with guiding information posters visible to all the professionals.
-
○ Rational: 1) to minimize the number of personnel and material; 2) to expose patients’ to less potential disease disseminators2121 Zheng MH, Boni L, Fingerhut F. Rolling updates on coronavirus disease (COVID-19) 2020 [Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen.
https://www.who.int/emergencies/diseases... .
-
-
• To be extremely careful during laparoscopic and open procedures with aspiration, cauterization, and insufflation devices. The pneumoperitoneal pressure should be as low as to offer excellent and safe anatomic exposure of the operating field. The power settings of the electrocautery should be as low as possible to avoid spillage of blood and tissues.
-
○ Rational: to minimize contaminating particle dispersions1717 Zheng MH, boni L, Fingerhut A. MInimally invasive surgery and the novel coronavirus outbreak: lessons learned in China and Italy. Ann Surg. 2020;on line..
-
-
• To carry out rigorous sterilization of the room and materials according to the local health rules1818 Saúde Md. 2020 [cited 2020 March, 22nd 2020]. Available from: https://saude.gov.br/.
https://saude.gov.br/... .-
○ Rational: 1) to guarantee the next patient’s safety and also of the attending team.
-
-
• To control the number of patients’ visitors, mainly those in the intensive care units (if necessary, consider, canceling all of them).
-
○ Rational: 1) to minimize the traffic of people and materials; 2) to guarantee decreased patients’ exposure to other individuals who may be asymptomatic carriers1515 Surgeons ACo. Covid-19 Recommendations for Management of Elective Surgical Procedures [Available from: https://www.facs.org/about-acs/covid-19/information-for-surgeons.
https://www.facs.org/about-acs/covid-19/... .
-
-
• To ensure, in trauma scenarios, that the whole healthcare team (at the different stages of assistance, since the screening process to the on-site aid, the transport and the hospital admission) provides the adequate assistance and protects themselves by using appropriate IPEs1414 Surgeons TcotQpotACo. Maintaining trauma Center Acess and Care during the Covid-19 Pandemic: Guidance Document for Trauma Medical Directors 2020 [Available from: https://www.facs.org/quality-programs/trauma/maintaining-access.
https://www.facs.org/quality-programs/tr... .-
○ Rational: 1) to minimize virus dissemination among healthcare professionals, in particular, those exposed to body secretions and blood, while considering every patient as a potential virus disseminator; 2) to decrease the risk of patient exposure to asymptomatic healthcare professionals; 3) to reorganize the schedules and the shifts of the teams, foreseeing the potential risk of work overload and concomitant ill states, which would impact the quality of assistance, and the availability of more professionals if required.
-
-
• To develop support strategies to healthcare professionals, mainly those with young children, and offer them better psychologic conditions to ensure they can provide good quality care
-
○ Rational: 1) schools have been locked down; 2) potential caretakers, like grandparents, are at higher risk of Covid-19 and also at higher risk of complications. Therefore they should not be taking care of children1919 Organization WH. Rolling updates on coronavirus disease (COVID-19). 2020..
-
-
• To support, under this critical situation, the recommendation by the Conselho Federal de Medicina n. 1756/20202222 OFÍCIO CFM Nº 1756/2020 - COJUR - Telemedicina, (2020). on teleorientation, telemonitoring, and teleinterconsultation.
-
○ Rational: 1) the need to remotely help patients under isolation; 2) to support medical orientation and supervision of various disease and healthy parameters; to allow medical information exchange and opinions to help doctors in diagnosis and therapies.
-
-
• To re-book operations only when suggested and allowed by the official healthcare entities1818 Saúde Md. 2020 [cited 2020 March, 22nd 2020]. Available from: https://saude.gov.br/.
https://saude.gov.br/... .
The Brazilian College of Surgeons is well aware that there is a great amount of information, but the scientific evidence is weak. Therefore it essentially suggests quality and safety initiatives to help the patients and the healthcare professionals face this challenging situation. Healthcare professionals should not be seen as heroes2222 OFÍCIO CFM Nº 1756/2020 - COJUR - Telemedicina, (2020)., but rather as human beings who have chosen a profession to take care of others. They were taught to do so, but unfortunately not routinely trained to face disaster situations and even less scientific prepared to critically appraise the deluge of published manuscripts1212 Correia M. Are we capable of separating the wheat from the chaff when assessing meta-analyses? Clin Nutr. 2020;39(3):705-7.,2323 Herós em guerra. Veja. 2020 March, 25th, 2020.
24 Grech V, Rizk DEE. Increasing importance of research metrics: Journal Impact Factor and h-index. Int Urogynecol J. 2018;29(5):619-20.-2525 Karabulut N. Inaccurate Citations in Biomedical Journalism: Effect on the Impact Factor of the American Journal of Roentgenology. AJR Am J Roentgenol. 2017;208(3):472-4..
-
Source of funding: none.
REFERÊNCIAS
-
1Salehi S, Abedi A, Balakrishnan S, Gholamrezanezhad A. Coronavirus Disease 2019 (COVID-19): A Systematic Review of Imaging Findings in 919 Patients. AJR Am J Roentgenol. 2020:1-7.
-
2Pubmed [Available from: https://pubmed.ncbi.nlm.nih.gov/
» https://pubmed.ncbi.nlm.nih.gov/ -
3Ioannidis JPA. Randomized controlled trials: Often flawed, mostly useless, clearly indispensable: A commentary on Deaton and Cartwright. Soc Sci Med. 2018.
-
4Ioannidis JPA. Hijacked evidence-based medicine: stay the course and throw the pirates overboard. J Clin Epidemiol. 2017;84:11-3.
-
5Ioannidis JP. Evidence-based medicine has been hijacked: a report to David Sackett. J Clin Epidemiol. 2016;73:82-6.
-
6Ioannidis JP. Why most published research findings are false. PLoS Med. 2005;2(8):e124.
-
7Ioannidis JPA. A fiasco in the making? As the coronavirus pandemic takes hold, we are making decisions without reliable data Statnew: Boston Globe; 2020 [Available from: https://www.statnews.com/2020/03/17/a-fiasco-in-the-making-as-the-coronavirus-pandemic-takes-hold-we-are-making-decisions-without-reliable-data/?fbclid=IwAR0r5W-fu7C4Qi19bUdiW_ekgbTu6HpP98xx5BBaZjL1bZn5QjIvaVbm3yc
» https://www.statnews.com/2020/03/17/a-fiasco-in-the-making-as-the-coronavirus-pandemic-takes-hold-we-are-making-decisions-without-reliable-data/?fbclid=IwAR0r5W-fu7C4Qi19bUdiW_ekgbTu6HpP98xx5BBaZjL1bZn5QjIvaVbm3yc -
8Goldenberg S. [Reflections on the truth]. Acta Cir Bras. 2007;22(6):420-1.
-
9C A. The End of Theory: The Data Deluge Makes the Scientific Method Obsolete https://www.wired.com/2008/06/pb-theory/2008 [
» https://www.wired.com/2008/06/pb-theory/2008 -
10Askheim C, Sandset T, Engebretsen E. Who cares? The lost legacy of Archie Cochrane. Med Humanit. 2017;43(1):41-6.
-
11Noone KJ. Beware the impact factor. Ambio. 2016;45(5):513-5.
-
12Correia M. Are we capable of separating the wheat from the chaff when assessing meta-analyses? Clin Nutr. 2020;39(3):705-7.
-
13Brindle M, Gawande A. Managing COVID-19 in Surgical Systems. Ann Surg. 2020;accepted(on line).
-
14Surgeons TcotQpotACo. Maintaining trauma Center Acess and Care during the Covid-19 Pandemic: Guidance Document for Trauma Medical Directors 2020 [Available from: https://www.facs.org/quality-programs/trauma/maintaining-access
» https://www.facs.org/quality-programs/trauma/maintaining-access -
15Surgeons ACo. Covid-19 Recommendations for Management of Elective Surgical Procedures [Available from: https://www.facs.org/about-acs/covid-19/information-for-surgeons
» https://www.facs.org/about-acs/covid-19/information-for-surgeons -
16Aminian A, Safari S, Razeghian_Jahromi A, Ghorbani M, Delaney CP. Covid-19 Outbreak and Surgical Practice: Unexpected Fatality in Perioperative Period. Ann Surg. 2020;on line.
-
17Zheng MH, boni L, Fingerhut A. MInimally invasive surgery and the novel coronavirus outbreak: lessons learned in China and Italy. Ann Surg. 2020;on line.
-
18Saúde Md. 2020 [cited 2020 March, 22nd 2020]. Available from: https://saude.gov.br/
» https://saude.gov.br/ -
19Organization WH. Rolling updates on coronavirus disease (COVID-19). 2020.
-
20Saúde Md. Cirurgias seguras salvam vidas Rio de Janeiro: Organização Pan-Americana da Saúde ; Ministério da Saúde ; Agência Nacional de Vigilância Sanitária; 2009 [Available from: http://bvsms.saude.gov.br/bvs/publicacoes/seguranca_paciente_cirurgias_seguras_guia.pdf
» http://bvsms.saude.gov.br/bvs/publicacoes/seguranca_paciente_cirurgias_seguras_guia.pdf -
21Zheng MH, Boni L, Fingerhut F. Rolling updates on coronavirus disease (COVID-19) 2020 [Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen
» https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen -
22OFÍCIO CFM Nº 1756/2020 - COJUR - Telemedicina, (2020).
-
23Herós em guerra. Veja. 2020 March, 25th, 2020.
-
24Grech V, Rizk DEE. Increasing importance of research metrics: Journal Impact Factor and h-index. Int Urogynecol J. 2018;29(5):619-20.
-
25Karabulut N. Inaccurate Citations in Biomedical Journalism: Effect on the Impact Factor of the American Journal of Roentgenology. AJR Am J Roentgenol. 2017;208(3):472-4.
-
26Ioannidis JP. The Mass Production of Redundant, Misleading, and Conflicted Systematic Reviews and Meta-analyses. Milbank Q. 2016;94(3):485-514.
-
27"Coronavirus surgery" [Pubmed]. 2020 [Available from: https://pubmed.ncbi.nlm.nih.gov/?term=%22coronavirus+surgery%22
» https://pubmed.ncbi.nlm.nih.gov/?term=%22coronavirus+surgery%22
Publication Dates
-
Publication in this collection
30 Mar 2020 -
Date of issue
2020
History
-
Received
23 Mar 2020 -
Accepted
23 Mar 2020