Abstract
OBJECTIVE: This study analyzed the total symptom score, irritative and obstructive domains of IPSS questions regarding quality of life and the urodynamic diagnosis in 400 men with LUTS. MATERIALS AND METHODS: Four hundred consecutive male patients were prospectively enrolled after being submitted to full urodynamic evaluation and IPSS. Obstructed and non-obstructed patients were compared regarding the symptoms score and quality of life. Results were assessed through Wilcox, ANOVA and Student-t tests. RESULTS: 80.2% were diagnosed as urodynamically obstructed of which 42.4% presented detrusor instability in the filling phase. In obstructed patients there were no statistical difference concerning obstructive or irritative questions from IPSS (p = 0.50). It was not possible either to predict which patients presented detrusor instability based on the questionnaire (p = 0.65). Out of seventy-nine cases unobstructed (19.8%), 65.4% revealed detrusor instability. These cases could not be distinguished from all obstructed men based on the clinical questions measured by IPSS (p = 0.87). Obstructive and irritative questions did not present different indexes than obstructed cases (p = 0.63). Subjective quality of life index did not discriminate obstruction nor it could predict detrusor instability in both groups. CONCLUSION: Clinical symptoms and quality of life index measured by the IPSS as well as its obstructive and irritative domains do not have discriminating power to predict the presence of infravesical obstruction in males with LUTS, demanding objective tools to demonstrate obstruction.
urinary symptoms; urodynamics; bladder outlet obstruction; prostate; prostatism
UROLOGICAL NEUROLOGY
International prostate symptom score IPSS - AUA as discriminat scale in 400 male patients with lower urinary tract symptoms (LUTS)
Paulo Rodrigues; Alex Meller; João C. Campagnari; Daniel Alcântara; Márcio D'Império
Neurourology and Voiding Section, Beneficência Portuguesa Hospital, and Santa Helena Hospital, São Paulo, SP, Brazil
Correspondence Correspondence to Dr. Paulo Rodrigues Clínica de Especialidades Cirúrgicas Rua Maestro Cardim 377 / 7o. andar / cj. 75/76 São Paulo, SP, 01323-002, Brazil Fax: + 55 11 283-1450 E-mail: paulortrodrigues@aol.com
ABSTRACT
OBJECTIVE: This study analyzed the total symptom score, irritative and obstructive domains of IPSS questions regarding quality of life and the urodynamic diagnosis in 400 men with LUTS.
MATERIALS AND METHODS: Four hundred consecutive male patients were prospectively enrolled after being submitted to full urodynamic evaluation and IPSS. Obstructed and non-obstructed patients were compared regarding the symptoms score and quality of life. Results were assessed through Wilcox, ANOVA and Student-t tests.
RESULTS: 80.2% were diagnosed as urodynamically obstructed of which 42.4% presented detrusor instability in the filling phase. In obstructed patients there were no statistical difference concerning obstructive or irritative questions from IPSS (p = 0.50). It was not possible either to predict which patients presented detrusor instability based on the questionnaire (p = 0.65). Out of seventy-nine cases unobstructed (19.8%), 65.4% revealed detrusor instability. These cases could not be distinguished from all obstructed men based on the clinical questions measured by IPSS (p = 0.87). Obstructive and irritative questions did not present different indexes than obstructed cases (p = 0.63). Subjective quality of life index did not discriminate obstruction nor it could predict detrusor instability in both groups.
CONCLUSION: Clinical symptoms and quality of life index measured by the IPSS as well as its obstructive and irritative domains do not have discriminating power to predict the presence of infravesical obstruction in males with LUTS, demanding objective tools to demonstrate obstruction.
Key words: urinary symptoms; urodynamics; bladder outlet obstruction; prostate; prostatism
INTRODUCTION
Benign prostatic hyperplasia is a frequent histological finding in the elderly population. In the meanwhile symptomatic voiding disturbances related to infravesical obstruction are a much less frequent complaint (1). Notably surgical therapy is intended to relief the symptoms and complaints in case there is urodynamically proven urethral obstruction (2).
Clinical questionnaires allow homogeneity and comparable final results after different therapies. They were also historically designed with an initial intent to avoid invasive and costly evaluations justifying the division of urinary symptoms into irritative and obstructive ones (3-6).
Nevertheless in the clinical setting patients present a myriad of urinary complaints all together with no clear division between obstructive and irritative urinary symptoms becoming extremely difficult to diagnose those with infravesical obstruction from those with detrusor instability.
The morphologic evaluation of the prostate based on volume, presence of median lobe, flow rate, bladder residual volume or urinary symptoms seems to be inadequate due to the wide variability and the same clinical prevalence despite the presence or absence of infravesical obstruction (7,8) requiring special attention not to the prostate morphology but to the clinical picture and bothersome symptoms related to voiding difficulties (2).
In the present study the International Prostate Symptoms Score (IPSS) (3) diagnostic specificity was questioned as a valid tool to determine the presence of infravesical obstruction.
PATIENTS AND METHODS
Four hundred consecutive enrolled male patients were prospectively studied with urodynamic evaluation to assess the significance of the IPSS - AUA. All patients filled out the IPSS with no interferences before going to urodynamic evaluation.
The urodynamic study was repeated 3 times, in order to allow reproducibility and smoother curves according to ICS (9) recommendations. It consisted of repeated pressure-flow and cystometry in a standing position with saline infusions at 37°C.
Infravesical obstruction was established on the Abrams-Griffiths' normogram (10) while instability was assigned if > 15 cmH2O (11).
When patients were assigned to the doubtful zone passive urethral resistance relation was calculated and designated as obstructed if > 2 cmH2O/ml/s is obtained.
Obstructed patients were compared to non-obstructed ones.
Total symptoms score and quality of life were compared between the groups.
The sum of questions addressing irritative symptoms (questions 2, 4 and 7) was compared to the sum of questions addressing obstructive complaints (questions 1, 3, 5 and 6) from the IPSS in each group and between the groups.
Quality of life index was also compared to the irritative and obstructive sum in the obstructed and non-obstructed groups.
Wilcox, ANOVA and Student-t test were used as necessary with a 5% statistical significance.
RESULTS
Whole Group
The median age of the whole group was 58.2 years (range: 44 77 years-old).
The average obstructive symptoms was 8.05 ± 3.2 (maximum possible = 20) while the irritative symptoms showed an average 9.26 ± 4.1 (maximum possible = 15) for the studied population. This finding revealed an important contribution of urgency symptoms as a bother perception of the voiding dysfunction in males seeking medical care.
Urodynamic findings
Infravesical obstruction could be documented in 321 cases (80.2%) of which 136 men (42.4%) revealed detrusor instability on filling cystometry. On the other hand 52 (19.8%) of the 79 non-obstructed cases showed detrusor instability (Table-1).
Total symptoms score X Quality of life
There was no statistical correlation between quality of life and total symptoms score in all 400 cases (p = 0.14), although the total score demonstrated a trend to higher interference in the subjective perception of quality of life (Y = 0.0467 + 2.63). Paradoxically some patients (32 cases) showed higher total symptoms score but low perception of bother (Figure-1).
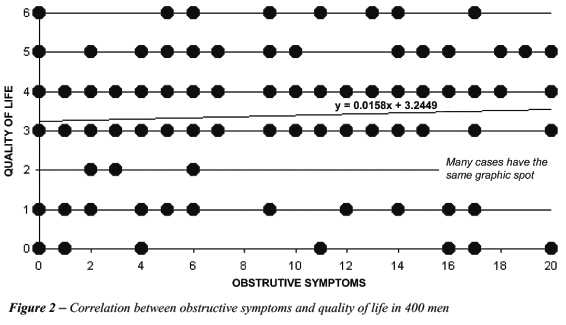
The division of the questions domains into obstructive and irritative questions demonstrated non-significant statistical relationship to the observed quality of life (Figure-2 and 3 ).
Total symptoms score in obstructed and non-obstructed groups
The total symptoms score did not differ between obstructed and non-obstructed cases (p = 0.87) and the same observation was set when only patients with detrusor instability in both groups were compared (p = 0.53). (Table-2)
Irritative symptom score in the obstructed and non-obstructed groups
The irritative symptoms score in obstructed and non-obstructed patients did not show any statistical significance (p = 0.18).
When only the obstructive symptoms were analyzed in patients presenting detrusor instability no statistical difference could be noticed (p = 0.32). (Table-2)
Obstructive symptom score in the obstructed and non-obstructed groups
The irritative symptoms score in the obstructed and non-obstructed patients did not show any statistical significance (p = 0.15).
When only the irritative domain of symptoms was analyzed in patients presenting detrusor instability no statistical difference could be reached (p = 0.23). (Table-2)
Quality of life in obstructed and non-obstructed groups
The quality of life in obstructed and non-obstructed males was not statistically different (p = 0.23). Unstable patients did not differ from the stable ones (p = 0.17) but the unobstructed group showed lower total symptom score (p = 0.07). (Table-2)
Obstructed X Non-obstructed - value of questions domains
The irritative and obstructive questions domains from obstructed and non-obstructed groups were compared to check if the nature of the questions could diagnose the presence of infravesical obstruction.
There was no statistical difference between question domains in both groups or between 2 domains to each individual urodynamic classified group (Table-3).
Quality of life in obstructed and non-obstructed groups related to the urinary questions domains
The obstructed group did not show any statistical correlation between the subjective impression of quality of life and the questions from the obstructive domain (p = 0.77). The same was observed for the questions of the irritative domain (p = 0.67).
Neither obstructive questions (p = 0.75) nor irritative ones (p = 0.88) reached statistical correlation in non-obstructed cases. In none of the groups, when exclusively cases with instability were analyzed, it was possible to reach statistical significance (Table-3).
DISCUSSION
Voiding dysfunction was historically related to prostate enlargement (BPH). Since BPH is highly prevalent in any given male population from the fiftieth decade of life on, it demands high surveillance from health authorities (11).
The gold standard for bladder relief is transurethral resection of the prostate, but this can only be accomplished if obstruction is clearly present (2,12).
The subjective clinical success of prostate relief is directly related to pre-operative evaluation of infravesical obstruction frequently observing poor outcome in those not obstructed improperly diagnosed as infravesical obstruction due to bladder failure or bladder instability comprehending 30 to 42% of males in prospective series (2,12).
The clinical practice of electing patients to surgical treatment based on clinical evaluation was strengthened by the acceptance of standard urological questionnaires allowing homogeneity and objectivity to multiple treatment options (4). This practice was immediately accepted and new questionnaires were conceived and assumed as better than others, some with 24 items (13) demanding understanding from the patients but increasing the difficulty for widespread usage.
The modern approach for the treatment of LUTS highly recommends the subjective perception form the patient as well as the presence of obstruction.
The American Urological Association compiled all the questionnaires and consensually validated its own (3). They added a question concerning the subjective impression from the patient if he had to live forever with that urological picture.
Our series did not show any correlation to the urodynamic findings besides observing scattering pattern of subjective impression from the urological complaints into the same urodynamic group.
Other authors pointed out the lack of specificity of the clinical complaint as well as the questionnaires when they found similar picture in women with urological complaint originating the improper name "female prostatism" (14).
Non-invasive objective parameters such as free-flow rate (15), residual (16) and prostate volume (17) were not accurate.
Critical studies using urodynamic criteria failed to identify obstruction through clinical complaints or the presence of detrusor instability (18).
The division of the AUA symptoms score into irritative (questions 1, 3, 5 and 6) and obstructive (questions 2, 4 and 7) domains failed to identify obstruction or worsening of the quality of life.
We had also demonstrated that the symptoms cannot distinguish obstructed from non-obstructed cases.
Symptoms score is an easy and valuable tool to homogenize and compare clinical studies but it should not be used as a diagnostic instrument for surgical intervention since it does not show discriminative value.
CONCLUSIONS
International Prostate Symptom Score (IPSS) validated by the AUA should not be used to diagnose infravesical obstruction. The symptoms grouped according to the questionnaire did not distinguish obstructed from non-obstructed patients neither allowed previewing the presence of bladder instability on both groups. Obstructive and irritative symptoms should no longer be used since they do not state the existence or absence of infravesical obstruction in males. It was also possible to confirm that the clinical picture has a mild correlation with subjectively measured quality of life.
Received: August 10, 2003
Accepted after revision: March 1, 2004
- 1. Lytton B, Emer JM, Harvard BM: Incidence of benign prostatic obstruction, J Urol. 1968; 99: 639-45.
- 2. Rodrigues P, Lucon AM, Freire GC, Arap S: Urodynamic pressure-flow studies can predict the clinical outcome after transurethral prostatic resection. J Urol. 2001; 165: 499502.
- 3. Barry MJ, Fowler FJ Jr, O'Leary MP, Bruskewitz RC, Holtgrewe HL, Mebust WK, et al.: The American Urological Association symptom index for benign prostatic hyperplasia. J Urol. 1992; 148: 154953.
- 4. Boyarsky S, Jones G, Paulson DF, Prout GR Jr: A new look at bladder neck obstruction by the Food and Drug Administration regulatros: Guidelines for investigation of benign prostatic hypertrophy, Trans Amer Genito-Urin Surg. 1977; 68: 29-33.
- 5. Madsen PO, Iversen P: A point system for selecting operative candidates In Benign Prostatic Hypertrophy, New York, Heidelberg, Berlin:Springer-Verlag. 1983; pp.763-5.
- 6. Brasso K, Stigsby B, Pilsgard B, Nordling J: Precision of a patient-weighted symptom score in prostatism. Scand J Urol Nephrol. 1994; 28: 71-5.
- 7. Neal DE, Styles RA, Powell PH, Ramsden PD: Relationship between detrusor function and residual urine in men undergoing prostatectomy. J Urol. 1987; 60: 560-4.
- 8. Meyhoff HH, Ingelmann L, Nordling J, Hald T: Accuracy in preoperative estimation of prostatic size. Scand J Urol Nehrol. 1981; 15: 45-51.
- 9. Abrams P, Donovan JL, de la Rossette JJMC, Schafer W, the ICS-Study group: International Continence Society "Benign Prostatic Hyperplasia" Study: Background, Aims and Methodology. Neurourol Urodynam. 1997; 16: 7991.
- 10. Abrams PH, Griffiths DJ: The assessment of prostatic obstruction from urodynamic measurements and from residual urine. Br J Urol. 1979; 51: 129-34.
- 11. Garraway WM, Collins GN, Lee RJ: High prevalence of benign prostatic hypertrophy in the community. Lancet. 1991; 338: 469-71.
- 12. Javlé P, Jenkins AS, Machin DG, Parsons KF: Grading of benign prostatic obstruction can predict the outcome of transurethral prostatectomy. J Urol. 1998; 160: 1713-5.
- 13. Meyhoff HH, Hald T, Nordling J, Andersen JT, Bilde T, Walter S: A new patient weighted symptom score system (DAN-PSS-1). Scand J Urol Nephrol. 1993; 27: 493-6.
- 14. Lepor H, Machi G: Comparison of AUA symptom index in unselected males and females between fifty-five and seventy-nine years of age. Urology. 1993; 42: 36-9.
- 15. Gerstenberg TC, Andersen JT, Klarskov P, Ramirez D, Hald T: High flow infravesical obstruction in men: Symptomatology, urodynamics and the results of surgery. Scand J Urol Nephrol. 1982; 127: 943-5.
- 16. Griffiths CJ, Murray A, Ramsden PD: Accuracy and repeatability of bladder volume measurement using ultrasonic imaging. J Urol. 1986; 136: 808-12.
- 17. Meyhoff HH, Ingelmann L, Nordling J, Hald T: Accuracy in preoperative estimation of prostatic size. Scand J Urol Nephrol. 1981; 15: 45-51.
- 18. Chal TC, Belville WD, Mcguire EJ, Nyquist L: Specificity of the American Urological Association voiding symptom index: comparison of unselected and selected samples of both sexes. J Urol. 1993; 150: 1710-3.
Publication Dates
-
Publication in this collection
02 June 2004 -
Date of issue
Apr 2004
History
-
Accepted
01 Mar 2004 -
Received
10 Aug 2003