Abstracts
PURPOSE: To describe the anatomical variations of superficial inferior epigastric artery (SIEA) flap as a muscle-sparing flap. METHODS: A series of 40 dissections were performed on 20 preserved or fresh male cadavers. The site origin and drainage of vessels, caliber, length, and correlation between diameter and length of pedicle were identified. RESULTS: The SIEA and SIEV were identified at inguinal ligament level in 38 (95%) and 40 (100%) dissections, respectively. The SIEA originated directly from a common femoral artery 22 (57.9%) or a common trunk with other arteries. The SIEA was found within 1 cm of the midpoint of the inguinal ligament in 33 of 38 cases. The meanSD length of SIEA was 3.041.73 (0.5-7) cm. The meanSD caliber of SIEA was 1.450.35 (0.7-2.1) mm. The length of SIEV ranged from 2.2 to 12 cm with a meanSD of 5.452.08 cm. The caliber of SIEV ranged from 1.6 to 4 mm with a meanSD of 2.140.45 mm. The length of SIEA correlated with caliber of arterial pedicle (p<0.001 and correlation coefficient = 0.517). CONCLUSION: The inferior epigastric artery flap can be applied to microsurgical flap transfer, potentially in breast reconstruction, hemifacial atrophy, phalloplasty, or when extremely large amounts of skin coverage are required.
Epigastric Arteries; Surgical Flaps; Anatomy
OBJETIVO: Descrever as variações anatômicas do retalho muscular com artéria epigástrica superficial. MÉTODOS: Foram realizadas uma série de 40 dissecções em cadáveres do gênero masculino, preservados ou recentes, Foram identificados o local de origem e drenagem dos vasos: calibre, comprimento e correlação entre diâmetro e comprimento do pedículo. RESULTADOS: As artérias e veias epigástricas superficiais foram identificadas no nível do ligamento inguinal respectivamente em 38 (95%) e 40 (100%) das dissecções. A artéria epigástrica superficial originava diretamente da artéria femoral em 22 (57,9%) ou de um tronco comum com outras artérias. A artéria foi encontrada em um cm do ponto médio do ligamento inguinal em 33 de 38 casos. A média do comprimento da artéria epigástrica superficial foi de 3.04 1.73 (0,5-7) cm. A média do calibre da artéria foi 1.45 0.35 (0.7-2.1). O comprimento da veia epigástrica superficial foi de 2.2 a 12 cm com média de 5.452.08 cm. O calibre da veia era de 1.6 a 4 mm com média de 2.140.45 mm. O comprimento da artéria epigástrica superficial foi correlacionado com o calibre do pedículo arterial. CONCLUSÃO: O retalho com a artéria epigástrica superficial pode ser aplicado em microcirurgia de retalhos, potencialmente em reconstrução mamária, atrofia hemifacial, faloplastia ou quando se faz necessário aplicar em perdas acentuadas de pele.
Artérias Epigástricas; Retalhos Cirúrgicos; Anatomia
7 - ORIGINAL ARTICLE
PLASTIC SURGERY
The anatomy of superficial inferior epigastric artery flap1 Correspondence: Ebrahim Hatamipour North Kargar St. Tehran Heart Center, Tehran, Iran PO Box: 1411713138 Phone: (98 21) 2241-5543 Fax: (98 21) 8802-9256 ehatamipour@yahoo.com aliiabbasi@yahoo.com
Anatomia do retalho com a artéria epigástrica superficial
Mahdi FathiI; Ebrahim HatamipourI; Hamid Reza FathiI; Ali AbbasiII
IDepartment of Plastic and Reconstruction Surgery, Medical Sciences, Tehran University, Imam Khomeini Hospital, Tehran, Iran
IIDepartment of Clinical Research, Tehran Heart Center, Medical Sciences, Tehran University, Tehran, Iran
Correspondence Correspondence: Ebrahim Hatamipour North Kargar St. Tehran Heart Center, Tehran, Iran PO Box: 1411713138 Phone: (98 21) 2241-5543 Fax: (98 21) 8802-9256 ehatamipour@yahoo.com aliiabbasi@yahoo.com
ABSTRACT
PURPOSE: To describe the anatomical variations of superficial inferior epigastric artery (SIEA) flap as a muscle-sparing flap.
METHODS: A series of 40 dissections were performed on 20 preserved or fresh male cadavers. The site origin and drainage of vessels, caliber, length, and correlation between diameter and length of pedicle were identified.
RESULTS: The SIEA and SIEV were identified at inguinal ligament level in 38 (95%) and 40 (100%) dissections, respectively. The SIEA originated directly from a common femoral artery 22 (57.9%) or a common trunk with other arteries. The SIEA was found within 1 cm of the midpoint of the inguinal ligament in 33 of 38 cases. The mean+/-SD length of SIEA was 3.04+/-1.73 (0.5-7) cm. The mean+/-SD caliber of SIEA was 1.45+/-0.35 (0.7-2.1) mm. The length of SIEV ranged from 2.2 to 12 cm with a mean+/-SD of 5.45+/-2.08 cm. The caliber of SIEV ranged from 1.6 to 4 mm with a mean+/-SD of 2.14+/-0.45 mm. The length of SIEA correlated with caliber of arterial pedicle (p<0.001 and correlation coefficient = 0.517).
CONCLUSION: The inferior epigastric artery flap can be applied to microsurgical flap transfer, potentially in breast reconstruction, hemifacial atrophy, phalloplasty, or when extremely large amounts of skin coverage are required.
Key words: Epigastric Arteries. Surgical Flaps. Anatomy.
RESUMO
OBJETIVO: Descrever as variações anatômicas do retalho muscular com artéria epigástrica superficial.
MÉTODOS: Foram realizadas uma série de 40 dissecções em cadáveres do gênero masculino, preservados ou recentes, Foram identificados o local de origem e drenagem dos vasos: calibre, comprimento e correlação entre diâmetro e comprimento do pedículo.
RESULTADOS: As artérias e veias epigástricas superficiais foram identificadas no nível do ligamento inguinal respectivamente em 38 (95%) e 40 (100%) das dissecções. A artéria epigástrica superficial originava diretamente da artéria femoral em 22 (57,9%) ou de um tronco comum com outras artérias. A artéria foi encontrada em um cm do ponto médio do ligamento inguinal em 33 de 38 casos. A média do comprimento da artéria epigástrica superficial foi de 3.04 +/- 1.73 (0,5-7) cm. A média do calibre da artéria foi 1.45 +/-0.35 (0.7-2.1). O comprimento da veia epigástrica superficial foi de 2.2 a 12 cm com média de 5.45+/-2.08 cm. O calibre da veia era de 1.6 a 4 mm com média de 2.14+/-0.45 mm. O comprimento da artéria epigástrica superficial foi correlacionado com o calibre do pedículo arterial.
CONCLUSÃO: O retalho com a artéria epigástrica superficial pode ser aplicado em microcirurgia de retalhos, potencialmente em reconstrução mamária, atrofia hemifacial, faloplastia ou quando se faz necessário aplicar em perdas acentuadas de pele.
Descritores: Artérias Epigástricas. Retalhos Cirúrgicos. Anatomia.
Introduction
Since Wood first described the superficial inferior epigastric artery (SIEA) flap as an axial pattern for reconstructing forearm defect in 1863, several studies have reported its use as a pedicled or free flap for reconstructing upper and lower extremities, head and neck, breast and genital organs1-6. Early in the 1990s, the free SIEA flap was applied to breast reconstruction. As this flap is supplied solely from the superficial system, it can be elevated from the anterior rectus sheath to transfer abdominal skin and subcutaneous tissue, without harvesting or incising the muscles7-9. On the other hand, the transverse rectus abdominis myocutaneous (TRAM) flap is associated with considerable donor site morbidity, such as abdominal hernia and prolonged hospital stay10. Moreover, the SIEA flap is particularly advantageous for bilateral autologous tissue breast reconstructions, because the defect at the donor site can be repaired directly, the flap transfer leaves a scar similar to abdominoplasty, and the required superficial dissection at the femoral triangle poses low risk injury to vessels2,11. There were no differences in aesthetic results of breast reconstruction using TRAM, deep inferior epigastric artery perforator (DIEP), or SIEA flaps. The disadvantages of the SIEA flap include inconsistent vascular pedicle anatomy and the shorter and smaller diameter vascular pedicle10.
The SIEA is a direct cutaneous vessel that originates from the medial side of the common femoral artery, approximately two cm below the inguinal ligament. It pierces the cribriform fascia and passes anterior to the inguinal ligament in a superior course through the subcutaneous tissue of the abdominal wall. The area of skin supplied by the artery is 140±100 cm2 and tends to run in a curvilinear manner, 5 cm above the iliac crest. The flap extends from lateral anterior superior iliac spine to lateral border of rectus muscle and from umbilical area to pubis tubercle12,13. The anatomical information of vessels of SIEA flap have been studied in some clinical case series and limited dissections of cadavers. However, the anatomical findings of previous studies seem relatively discrepant. A recent study has shown that the SIEA is more consistently present and larger in caliber than the one previously believed14,15. This study demonstrated a series of 40 cadaver dissections and described the anatomical variations of SIEA and SIEV by caliber and size of flap pedicle, origin or drainage and position of vessels. Also, the correlation between the size and length of SIEA pedicle has been described.
Methods
A series of 40 dissections were performed on 20 preserved or fresh male cadavers. The cadavers' mean age at death was 39.05±14.06 years. An oblique incision was made overlying the inguinal ligament to dissect the skin and subcutaneous tissue of the lower border of the SIEA flap. An additional small incision (2 cm) was carried out longitudinally below the inguinal ligament to identify the precise site of the vessels. The SIEV or venae comitantes and SIEA positions relative to the midpoint of the inguinal ligament were measured along the course of vessels. The SIEA passed superiorly and laterally from the femoral triangle to cross the inguinal ligament deep in Scarpa's fascia. Above the inguinal ligament, the artery penetrated Scarpa's fascia to lie in the subcutaneous tissue. The SIEV was found laterally, or medially superficial, or deep in the SIEA. A number of vessels were identified at each dissection sites. The sites of vessels identified were medial and lateral to the midpoint of the inguinal ligament. The origin of the SIEA from the femoral artery was identified as a single, common trunk with other arteries or double SIEA. The SIEV or venea comitantes were traced towards the femoral vessels. The drainage of SIEV or venae comitantes into the saphenous bulb or other veins was identified as a single or more venous trunk. The external caliber of the SIEA and SIEV was measured using Vernier calipers. In each case, the caliber was measured at the most suitable site for applying microsurgical anastomosis. Also, the caliber of the most suitable vessel trunk was used to calculate the average of the caliber. Measurements of SIEA caliber were considered at the vessel origin from femoral artery or common trunk with other vessels. SIEV measurements were considered at the drainage to the saphenous bulb or other veins. The caliber of venae comitantes was measured independently. The pedicle length of SIEA was considered the distance between the most suitable proximal site and its disappearance into the tissue flap at inguinal ligament. The pedicle length of SIEV was considered the distance from the drainage site of vein or venae comitantes to its disappearance into the tissue flap at inguinal ligament.
Data analysis
Descriptive statistics of variables were summarized as a mean ± SD (range) or as percentage of cadavers having the characteristics. For the categorical variables, the statistical significance of difference among the sites of identification of vessels was evaluated by using χ2 tests. Linear regression analysis was performed to determine the correlation between size and caliber of the vascular pedicle. The level of p<0.05 was considered as statistically significant. Statistical analysis was performed using SPSS version 13 (Chicago, IL, USA).
Results
Position and origin of vessels
From 20 cadavers, the SIEA was identified at inguinal ligament level in 38 (95%) dissections. The SIEA was absent only in one dissection; in another dissection, it was not identified due to a relatively large hematoma at groin. Double SIEAs were observed in two distinct cadavers, arising from common femoral artery (CFA) with common or double trunk. The origin of the individual SIEA arose directly from CFA, common trunk with superficial circumflex iliac artery (SCIA), common trunk with pudendal artery (PA) and superficial femoral artery (SFA) in 22 (57.9%), 7 (18.4%), 2 (5.3%), and 5 (13.2%) of the 38 dissections, respectively. In the remaining two cases, the SIEA originated from external iliac artery or the lateral circumflex femoral branch of deep femoral artery. The SIEA was found within 1 cm of the midpoint of the inguinal ligament in 33 of 38 cadavers. However, in five cases, SIEA was identified within 1 to 2.5 cm far from the midpoint of inguinal ligament. In nine cases, SIEA was found lateral to the midpoint of inguinal ligament. The remaining 28 SIEAs crossed the inguinal ligament at midpoint (20 cases) or medially to midpoint; in one dissection only, two SIEAs crossed the inguinal ligament either medially or laterally to midpoint (Table 1).
In all the dissections, the SIEV was identified as an individual vein or pair of venae comitantes. In 24 dissections (60%), the venous drainage was as an individual vein into the saphenous bulb. In the remaining 16 cases, a pair of venae comitantes drained into the saphenous bulb. In some cases, the venae comitantes joined together; in other cases, the SIEV or venae comitantes were joined by other veins. In the most dissections, SIEV or venae comitantes were drained into the saphenous bulb at midpoint or medially to the midpoint of the inguinal ligament (Table 2).
In 33 cases, the SIEV and SIEA were found within 1 cm of the midpoint of the inguinal. Thus, the SIEV or venae comitantes were identified close to the SIEA crossing the inguinal ligament (p<0.0001) (Table 3).
Length and caliber of vascular pedicle
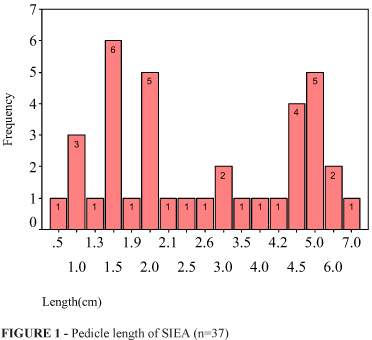
The pedicle length of SIEA was measured in 37 dissections. The mean±SD length of SIEA was 3.04±1.73 (0.5-7) cm. The median length of SIEA was 2.5 cm. In 17 (45.9%) of 37 dissections, the pedicle length of SIEA was 3 cm or longer (Figure 1).
The caliber of the SIEA was measured in 38 dissections. The mean±SD caliber of SIEA was 1.45±0.35 (0.7- 2.1) mm. The median caliber of SIEA was 1.5 mm (Figure 2).
In 20 (52.6%) of 38 cases, the caliber of SIEA was 1.5 mm or longer. In 13 (34.2%) of 38 cases, the caliber of SIEA was less than 1.4 mm. When the SIEA was harvested at origin from common trunk with SCIA in seven dissections, the mean caliber and length of pedicle was 1.63±0.28 mm and 4.09±1.79 cm, respectively. When the SIEA originated directly from CFA and SFA, the mean caliber was 1.36±0.41 mm and 1.48±0.08 mm, respectively. The length of pedicle was 2.5±1.35 cm when the SIEA originated directly from CFA. It was 3.8±2.71 cm when the vessel originated directly from SFA.
The pedicle length of SIEV was measured in 39 dissections. It ranged from 2.2 to 12 cm with a mean±SD of 5.45±2.08. The median length of SIEV was 5 cm (Figure 3).
The pedicle caliber of SIEV was measured in all dissections. It ranged from 1.6 to 4 mm with a mean±SD of 2.14±.45 mm. The median caliber of SIEV was 2 mm (Figure 4).
The linear correlation between the caliber of SIEA (x) and the length of SIEA (y) was expressed by the following equation with r = 0.517 and r2 = 0.268: Y= 0.517X -0.586. The length of SIEA was increased 2.5 mm by 0.1 mm of the caliber of SIEA.
Discussion
The SIEA is a direct cutaneous vessel that originates from the medial side of the femoral artery approximately 2 cm below the inguinal ligament. It pierces the cribriform fascia and passes anterior to the inguinal ligament in a superior course through the subcutaneous tissue of the abdominal wall. The flap extends from anterior superior iliac spine to lateral border of rectus muscle, and from umbilical area to pubis tubercle12,13. However, anatomical findings of previous studies seem relatively discrepant. The anatomical information of the flap was well described by Taylor and Daniel15. In 35 of 100 dissections, the SIEA was absent or could not be identified. The average caliber of SIEA trunk was 1.4 mm (48%) and 1.1 mm (17%) when the artery originated as a common trunk with SCIA and as an independent vessel, respectively. However, the anatomy of consistent veins and length of vascular pedicle was not reported.
In Hester et al.16, only 1 of 16 SIEA flaps was inadequate for free transfer In the series of 27 free SIEA flaps, Stern and Nahai12 reported the mean length of pedicle as 4 cm. In two cases, vein graft was necessary to increase the SIEA length for reconstruction. Arnez et al.2 described 20 breast reconstruction, using SIEA, DIEP, and TRAM flaps. Based on their protocol, exposure of the SIEA was performed for every patient whether its caliber was equal to or larger than 1.5 mm. The SIEA flap was used successfully in five breast reconstructions. Also, The SIEA was absent in 8 of 20 patients2,17. Recently, an anatomical study of 11 cadavers was reported by Reardon et al.13. The SIEA and SIEV were identified in 20 (90.9%) and 21 dissections, respectively. The SIEA originated from CFA within 1 cm of the midpoint of the inguinal ligament in 15 of 20 of cases. The average of SIEA length was 5.2 cm, ranged from 3 to 7 cm in 20 dissections. The mean caliber of SIEA was 1.9 mm (1.2- 2.5). The SIEA had a caliber of 1.5 mm or greater in 16 of 20 cases and a pedicle of 5 cm or longer in 14 cases. The venous drainage was as an individual vein, a pair of venae comitantes or both in 12, 8, and 1 dissections, respectively. Except in one case, all the veins drained into saphenous bulb. The mean caliber and pedicle length of the SIEV was 2.1 mm and 6.4 cm, respectively. Their findings suggested that the SIEA is more constant in its presence and has a greater caliber than the one previously reported. Also, it may have greater potential for clinical use than the one previously assumed 13. Chevray10 conducted a prospective study of 14 SIEA flap breast reconstruction, describing its reliability and limitations. The SIEA flap could not be used in 33 (70%) of 47 reconstructions because its criteria were not met. The SIEA was absent in 24 (51%) cases. In six patients (13%), the SIEA was considered too small for reliable use. The aesthetic results of breast reconstruction by using the SIEA, DIEP, or TRAM flaps were found to be indistinguishable. However, two SIEA flaps that required emergency reoperation were 1.5 mm in diameter8. Offman et al.13studied a series of five cadavers to describe the vascular anatomy of the lateral lumbar region. A dominant SIEA was present in 9 of 10 dissections. Using a technique of arterial injection, the mean length and emerging diameter of SIEA were measured as 96±60 mm and 1.2± 0.4 mm, respectively12.
The authors presented anatomical variations of the SIEA and SIEV in 40 cadaver dissections. In the current study, the SIEA was absent only in one dissection and it could not be identified in another dissection because there was a hematoma at the groin. Also, in all the dissection, the SIEV was identified as an individual vein or pair of venae comitantes. The presence of SIEA vessels was more than what was previously reported. Although two recent series of cadaver dissections had shown that SIEA was present in more than 90% of cases13,14, other clinical or cadaveric explorations had dissimilar findings. In our study, the caliber of SIEA was 1.5 mm or greater in more than 50% of the dissections. In clinical studies of the SIEA flap transfer, the pedicle caliber was found to be satisfactory in less than one-third of the patients2,8,11,15,17. However, Reardon et al.14 reported 80% of the dissections, had a caliber of 1.5 mm or greater. Thus, clinical studies have to be undertaken, especially randomized clinical trails of microsurgical transfer of the SIEA rather than other alternatives. Although the diameter of 1.5 mm has been accepted as the lower limit of successful anastomosis in breast reconstruction, these clinical experiences are inadequate. Although the SIEA is 1.5 mm or less in caliber the flap can be appropriate for other microsurgical reconstructions. Recently, the intraorally or extraorally transferred superficial inferior epigastric artery adiposal flap with a short pedicle has been used successfully for three patients with facial contour deformities. Regarding the anatomy of the superficial inferior epigastric artery system, it seems that the ascending branch of the superficial circumflex iliac artery compensates for the superficial inferior epigastric artery deficit. The superficial inferior epigastric artery flap can be raised in all patients, with the superficial inferior epigastric artery itself or with an ascending branch of the superficial circumflex iliac artery and large superficial epigastric vein system. The major disadvantage of a superficial inferior epigastric artery adiposal flap is that fine technical skills are necessary to dissect and anastomose the small and short pedicle vessels for the superficial inferior epigastric artery flap with a short pedicle. However, this flap seems to be the best application for facial contouring surgery and it is indicated especially for children and for young women who expect to become mothers6.
The length of SIEA is correlated to its caliber, that is, we expect to have longer SIEA with greater caliber during dissections. The SIEA and SIEV are more consistently present than those previously reported. The authors suggest that the SIEA flap can be applied for fasciocutaneous defect repair, potentially in the reconstruction of breast, head and neck, and extensive phalloplasty.
Conclusion
The inferior epigastric artery flap can be applied to microsurgical flap transfer, potentially in breast reconstruction, hemifacial atrophy, phalloplasty, or when extremely large amounts of skin coverage are required.
Acknowledgements
The authors wish to thank SPI Publisher Services LLC for assistance with technical support of English language.
Received: March 4, 2008
Review: May 5. 2008
Accepted: June 10, 2008
Conflict of interest: none
Financial source: none
1 Research performed at the Department of Plastic and Reconstruction Surgery, Medical Sciences, Tehran University, Imam Khomeini Hospital, Tehran, Iran.
- 1. Wood J. Extreme deformity of the neck and forearm. Med Chir Trans. 1863;46:151.
- 2. Arnez ZM, Khan U, Pogorelec D, Planinsek F. Breast reconstruction using the free superficial inferior epigastric artery (SIEA) flap. Br J Plast Reconstr. 1999;52:276-9.
- 3. Antia NH, Buch VI. Transfer of an abdominal dermo-fat graft by direct anastomosis of blood vessels. Br J Plast Surg. 1971;24(1):15-9.
- 4. Stevenson TR, Hester TR, Duus EC, Dingman RO. The superficial inferior epigastric artery flap for coverage of hand and forearm defects. Ann Plast Surg. 1984;12(4):333-9.
- 5. Woodworth BA, Gillespie MB, Day T, Kline RM. Muscle-sparing abdominal free flaps in head and neck reconstruction. Head Neck. 2006;28(9):802-7.
- 6. Koshima I. Short pedicle superficial inferior epigastric artery adiposal flap: new anatomical findings and the use of this flap for reconstruction of facial contour. Plast Reconstr Surg. 2005;116 (4):1091-7.
- 7. Grotting JC. The free abdominoplasty flap for immediate breast reconstruction. Ann Plast Surg. 1991;27(4):351-4.
- 8. Grotting JC, Beckenstein MS, Arkoulakis NS. The art and science of autologous breast reconstruction. Breast J. 2003;9(5):350-60.
- 9. Wolfram D, Schoeller T, Hussl H, Wechselberger G. The superficial inferior epigastric artery (SIEA) flap: indications for breast reconstruction. Ann Plast Surg. 2006;57(6):593-6.
- 10. Chevray PM. Breast reconstruction with superficial inferior epigastric artery flaps: A prospective comparison with TRAM and DIEP flaps. Plast Reconstr Surg. 2004;114(5):1077-83.
- 11. Tachi M, Yamada A. Choice of flaps for breast reconstruction. Int J Clin Oncol. 2005;10(5):280-97.
- 12. Stern HS, Nahai F. The versatile superficial inferior epigastric artery flap. Br J Plast Surg. 1992;45(4):270-4.
- 13. Offman SL, Geddes CR, Tang M, Morris SF. The vascular basis of perforator flaps based on the source arteries of the lateral lumbar region. Plast Reconstr Surg. 2005;115(6):1651-9.
- 14. Reardon CM, O'Ceallaigh S, O'Sullivan ST. An anatomical study of the superficial inferior epigastric vessels in humans. Br J Plast Surg. 2004;57(6):515-9.
- 15. Taylor GI, Daniel RK. The anatomy of several free flap donor sites. Plast Reconstr Surg. 1975;56 (3):243-53.
- 16. Hester TR Jr, Nahai F, Beegle PE, Bostwick J III. Blood supply of the abdomen revisited, with emphasis on the superficial inferior epigastric artery. Plast Reconstr Surg. 1984;74 (5):657-70.
- 17. Arnez ZM, Khan U, Pogorelec D, Planinsek F. Rational selection of flaps from the abdomen in breast reconstruction to reduce donor site morbidity. Br J Plast Surg. 1999;52 (5):351-4.
Publication Dates
-
Publication in this collection
03 Sept 2008 -
Date of issue
Oct 2008
History
-
Accepted
10 June 2008 -
Reviewed
05 May 2008 -
Received
04 Mar 2008